Article
Mauricio Arias-Rojas 1
Sonia Carreño-Moreno 2
Jennifer Rojas-Reyes 3
* Article derived from the PhD thesis entitled "Cuidadores PaliActivos" intervención para el manejo de la incertidumbre y la calidad de vida: ECA fase II.
* Artículo derivado de la tesis doctoral titulada: “Cuidadores PaliActivos” intervención para el manejo de la incertidumbre y la calidad de vida: ECA fase II.
* Artigo derivado da tese de doutorado intitulada: "Cuidadores PaliActivos" intervención para el manejo de la incertidumbre y la calidad de vida: ECA fase II.
1 ![]() 0000-0003-2096-1792. University of Antioquia, Nursing School, Colombia. emauricio.arias@udea.edu.co
0000-0003-2096-1792. University of Antioquia, Nursing School, Colombia. emauricio.arias@udea.edu.co
2 ![]() 0000-0002-4386-6053. National University of Colombia, Nursing School, Colombia. spcarrenom@unal.edu.co
0000-0002-4386-6053. National University of Colombia, Nursing School, Colombia. spcarrenom@unal.edu.co
3 ![]() 0000-0001-8962-5135. University of Antioquia, Nursing School. jennifer.rojasr@udea.edu.co
0000-0001-8962-5135. University of Antioquia, Nursing School. jennifer.rojasr@udea.edu.co
Received: 17/12/2019
Sent to peers: 23/01/2020
Approved by peers: 29/03/2020
Approved: 27/04/2020
Theme: Chronic Care.
Contribution to the subject: Caring for a caregiver of a person in palliative care is a function inherent to the Nursing professionals. Uncertainty towards the disease of a family caregiver is a phenomenon that marks the experience of caring for a person in palliative care. For this reason, knowing and organizing the available evidence on this phenomenon will allow optimizing decision-making both in and for the care practice targeted to family caregivers, as well as developing future research studies in this area. This review contributes to the disciplinary development on the use and application of the Theory of Uncertainty towards the disease, in the context of caring for individuals in palliative care.
Para citar este artículo / To reference this article / Para citar este artigo: Arias-Rojas M, Carreño-Moreno S, Rojas-Reyes J. Uncertainty towards the disease of family caregivers of patients in palliative care: A scoping review. Aquichan. 2020;20(3):e2034. DOI: https://doi.org/10.5294/aqui.2020.20.3.4
|
Abstract Objective: To know the development of the scientific evidence on the uncertainty towards
the disease of family caregivers of patients in palliative care. Keywords (Source DeCS): Uncertainty; Nursing; Caregivers; Palliative Care; Palliative Care at the end of life. |
Resumen Objetivo: conocer el desarrollo de la evidencia científica
sobre la incertidumbre ante la enfermedad de cuidadores familiares de pacientes
en cuidados paliativos. Palabras clave (Fuente: DeCS): Incertidumbre; enfermería; cuidadores; cuidados paliativos; cuidados paliativos al final de la vida. |
Resumo Objetivo: conhecer o desenvolvimento de evidências científicas
sobre a incerteza de cuidadores familiares em relação à doença de pacientes em
cuidados paliativos. Palavras-chave (Fonte DeCS): Incerteza; enfermagem; cuidadores; cuidados paliativos; cuidados paliativos na terminalidade da vida. |
Introduction
Despite the technological advances and the emergence of new treatments, cancer and other chronic diseases have shown an increase worldwide, regardless of the countries’ income levels. For example, in the context of low- and middle- income countries, chronic diseases are the first cause of death (1). Many of them progress and require palliative care due to late diagnosis, disease aggressiveness, or treatment failures (2).
Added to the aforementioned, the experience of a person with an advanced disease in palliative care is characterized for being complex, with important physical and spiritual needs, and the family caregiver accompanies this situation (3). On many occasions, these caregivers must take on their role without adequate training, without the continuous accompaniment by health professionals, and without appropriate support networks, which triggers in them feelings of uncertainty towards the patient’s disease (4). Additionally, becoming a caregiver implies stressful factors, changes in the relationships, and expectations regarding the care tasks, which generate control imbalances (5), emotional instability, and negative feelings towards this new reality (6, 7).
Family caregivers of patients in palliative care experiment sensations and feelings like those described, but with higher intensity, reason why they present greater episodes of anxiety and depression than caregivers of other types of patients (8-9). According to a study supporting that assertion, 80 % and 82 % of the caregivers present anxiety and depression signs, respectively, whereas 69 % noticed overburdens in their duties. Added to this are the characteristics of the context, in which they are constantly close to the death of the person they are caring for, a factor which increases uncertainty towards the disease (10).
Such uncertainty towards the disease is a cognitive state that inhibits the person to determine the meaning of the events related to the disease, which generates inability to assign definite values to objectives and events and to accurately predict consequences (11).
Evidence shows that other aspects related to uncertainty towards the disease of the caregiver are lack of knowledge on the patients’ situation, their home care, and medication management, apart from the absence of follow-up and social support (6-7). Thus, the importance having been described of approaching uncertainty towards the disease for the caregivers of people in palliative care, the aim of this article is to know the development of the scientific evidence on uncertainty towards the diseases of family caregivers of patients in palliative care.
Materials and methods
A descriptive review of the scoping review type (12) which aims to answer the following questions: What is the current state of the scientific knowledge on the phenomenon of uncertainty towards the disease in caregivers of patients in palliative care? What kind of evidence is found on the theme and what are the gaps in research? The search was conducted in the Embase, ScienceDirect, Medline, Academic Search Complete, and Scopus databases, in the English, Spanish, and Portuguese languages, and was limited to the 2000-2019 period. The MeSH terms and the Boolean operators were used as follows: uncertainty AND palliative care OR end of life AND nursing AND caregiver.
The inclusion criteria considered for this review are original articles or those derived from research which included subjects such as caregivers of patients with cancer or with other chronic diseases in advances stages, at the end of their lives, or in palliative care. Books and theses were excluded due to their extension, as well as reflection and narrative review articles, for the impossibility of cataloging them within the levels of evidence given by the Joanna Briggs Institute (JBI) (13). The classification of the evidence used was by levels of effectiveness and meaning, which apply to quantitative and qualitative studies, respectively. The highest level of evidence was classified with 1 and the lowest, with 5.
This type of classification was selected because it is one of the broadest in the inclusion of various methodological approaches. The strategy for conducting the search and selecting the articles is detailed in Figure 1. The bibliographic search lead to the selection of 145 original articles, 65 being excluded due to failures in their internal validity; after applying the CASP-e instrument, 50 original articles or research results were selected for analysis.
Figure 1. Flowchart of the strategy for conducting the search and selecting the articles. Bogotá, 2020.
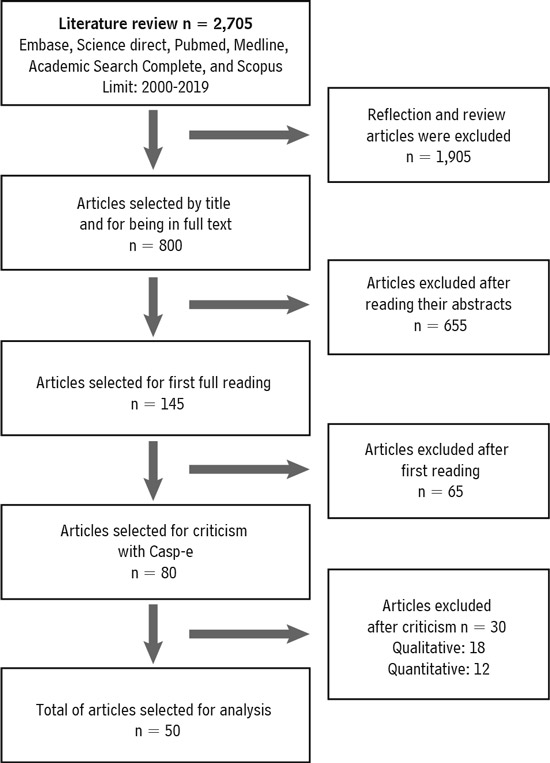
Source: Own elaboration.
The steps proposed by the selected review methodology were developed (12), which include: question, objective, inclusion criteria, participants, main concept, context, search and selection of articles, extraction and classification of results, and discussion (12). To analyze the information, the articles were compiled in Microsoft Excel, where a matrix was created in which the following were defined as variables to be considered: research approach, study design, data collection means, analysis used, its main results, and conclusions. Subsequently, the quality of the article was criticized by means of the CASP-e instruments, a series of checklists to assess the contents of quantitative and qualitative studies. Those checklists contain questions to identify if, in the research article, there is a clear definition of the study objectives, coherence in the methodology employed, and adequate selection of participants, among other aspects (14).
The information was organized by common characteristics and a name was assigned to each group of articles, taking into account the criteria of thematic or methodological affinity. This process generated a total of five groups: 1) Characterization of uncertainty in the caregiver, 2) Factors influencing uncertainty, 3) Resources to manage uncertainty, 4) Uncertainty assessment, and 5) Therapies and interventions to approach uncertainty.
Faced with the ethical considerations of the study, the researches took into account the principles of copyright when using and referencing all the material analyzed.
Results
The thematic distribution of the information lead to an integration of the most frequently approached concepts in the articles. It was found that the most frequently approached concept was that of factors influencing uncertainty, with 36 % of the total frequency of the themes. In the case of the methodological approach, the qualitative research was predominant, with 38 % of the total analyzed, as well as the development of interventions for caregivers, with 8 %. The information is presented in Table 1.
Table 1. Distribution of the reviewed articles according to methodology and theme. Medellin, Colombia, 2020
Themes |
Methodological approach |
Total n (%) |
|||
Qualitative n (%) |
Quantitative |
Systematic |
|||
Non-experimental |
Experimental |
||||
Characterization of uncertainty in the caregiver |
1 (2) |
5 (10) |
- |
4 (8) |
10 (20) |
Factors influencing uncertainty |
10 (20) |
7 (14) |
- |
1 (2) |
18 (36) |
Resources to manage uncertainty |
6 (12) |
3 (6) |
3 (6) |
- |
12 (24) |
Uncertainty assessment |
2 (4) |
2 (4) |
- |
2 (4) |
6 (12) |
Therapies and interventions to approach uncertainty |
- |
- |
4 (8) |
- |
4 (8) |
Total |
19 (38) |
17 (34) |
7 (14) |
7 (14) |
50 (100) |
Source: Review data, 2009-2019.
Apart from the contributions found in each of the reviewed articles, Table 2 presents the predominant level of evidence according to the JBI (13) and the voids in the research according to each thematic category.
Table 2. Levels of evidence and explicit voids found by theme. Medellin, Colombia, 2020
Themes |
Level of evidence according to the JBI* |
Explicit voids |
Characterization of uncertainty in the caregiver |
Levels 1B, 2B, and 4B in effectiveness |
Research must point to the development of studies which comparatively establish uncertainty levels in caregivers of individuals at the end of their lives, as a consequence of diseases other than cancer. It is necessary to characterize the uncertainty of the caregivers and its relation with mental health and the coping processes they go through. |
Factors influencing uncertainty |
Level 3 in meaning and Level 4B in effectiveness |
Studies must be conducted which verify the influence of various factors on the levels of uncertainty towards the diseases of the caregivers. |
Resources to manage uncertainty |
Level 2 in meaning and Level 4B in effectiveness |
Health professionals are one of the resources that can best help control uncertainty in the caregivers; however, what the literature describes shows the lack of training in palliative care and in communicative skills to approach those caregivers. It is then important to know the perception and experience of these professionals towards end of life, as well as to develop interventions that favor these competences for palliative care. |
Uncertainty assessment |
Levels 4B and 4B in effectiveness |
Research must be targeted to the development of valid and reliable instruments with enough sensitivity to assess the uncertainty of the caregiver in different contexts of diseases in advanced stages and at the end of life. With this, the expectation would be being able to determine the schooling level of the caregivers, the social support they have, their perception of the health professionals, and the coping strategies leading to a positive or negative assessment of uncertainty towards the disease. |
Therapies and interventions to approach uncertainty |
Levels 1C and 2C in effectiveness |
This theme is the one that presents the fewest studies. There are few existing interventions to approach uncertainty in caregivers of individuals in palliative care. Thus, the need emerged to develop different intervention strategies about uncertainty towards the disease and its influencing factors and, to this end, it is necessary to assess its acceptance by the caregivers, its impact, and its effect. |
Source: Review data, 2009-2019.
Discussion
Below are the findings in the literature for each thematic category.
Characterization of uncertainty in the caregiver
In a descriptive manner, the literature reports that the caregivers of individuals in palliative care have higher levels of uncertainty than other types of caregivers of people in acute or chronic conditions. For example, a study (15) assessed the level of uncertainty in caregivers of patients with prostate cancer and found a mean value of uncertainty of 60 out of 140 points; however, such values are lower than those found in another study (16), which discovered a medium level of uncertainty of 92 points out of 155 in caregivers of patients in palliative care. The studies suggest that these levels occur due to aspects like the specific characteristics of the palliative care context, the absence of adequate support for the caregivers, the discontinuity of care, and the lack of professional skills to identify the caregiver’s needs, apart from limited planning and evaluation of the objectives of patient’s caregiver (17-18).
As observed, there are some unique characteristics associated with caring for a person in palliative care, and they are related to the appearance of uncertainty towards the disease. The caregivers report high prevalence of unmet care needs that trigger negative results in the execution of their role. Those needs include access to truthful information (about themes like the physical care of the patient), psychological support, access to funding support, and spiritual well-being. The studies (19) show that there is a 26 % to 100 % prevalence of unmet needs in aspects such as receiving information related to the care for the patient, the disease, its treatment, management of symptoms, nutrition, and medication. The unmet needs of the physical type represent 42 % and are related to the quality of care; the psychological needs vary from 17 % to 78 % and refer to the management of sadness and solitude, among other aspects; the financial needs vary from 17 % to 67 % and are related to finding financial support and governmental benefits for the caregiver and for the patient; the spiritual needs vary from 3.8 % to 100 %, and imply re-signifying the experience; finally, the social needs vary from 42 % to 71 % and are connected to the absence of social support to help in the care provided.
These reported needs differ from those of other caregiver populations, since the health condition and care demands of a person in palliative care increase with time. Additionally, not only care in basic activities of daily life is required but also, as the disease progresses, the management of complex devices such as drainage systems or infusion pumps becomes necessary, as well as of medications like opioids and anxiolytics (20). Finally, having to face the end of life, death, and the imminent loss of a loved one (21) makes the experience of caring for a person in palliative care unique and complex, for having to fight an anticipated duel every day, faced with the expectation of the condition worsening or of the appearance of new symptoms in the patient, with the addition of uncertainty about the future (22).
In many occasions, the uncertainty towards the disease experienced by the caregivers generates negative outcomes in them. For example, mental health problems have been reported due to the fact that the same caregivers mention a care burden which ends up affecting their own psychological well-being. Other negative outcomes are related to the reduction in quality of life, the appearance of fatigue, depression, anxiety, isolation, solitude, sadness, and frustration (23-24). Thus, uncertainty towards the disease is characterized by bringing along problems in all the dimensions of the family caregiver’s quality of life.
Factors influencing uncertainty
This part describes what the literature reports about the factors associated to uncertainty in the family caregiver of a person in palliative care; they are circumscribed to lack of knowledge, invisibilization of the caregiver role, absence of social support, and quality of life.
As regards the lack of knowledge about the disease, diverse studies have found that it increases uncertainty towards the disease. It has also been reported that, although there is lack of knowledge in the caregivers, certain duality is experienced between what the caregivers want to know what they actually know. A research study described that caregivers are in for big surprises when they discover that the patient’s disease is incurable or that it is in a terminal phase (25), a notion that is seldom clear for the caregivers and is minimally approached by the health professionals (26). The consequence of the aforementioned is a phenomenon called ambiguous loss (27), which is characterized by the caregivers’ inability to work on the feelings of loss of their loved ones, since the disease prognosis or the final outcome are not clear (28).
On the other hand, caregivers refer to having little knowledge related to the physical care for the patient, in aspects like medication, pain control, and support for the activities of daily life. In a study it was reported that, out of twenty caregivers interviewed, only six recognized the term opioid (29). It was also found that the caregivers possess false beliefs related to the addiction to pain killers, and that they feel overwhelmed by the complexity of the administration of analgesia, the use of the subcutaneous route, the assessment of pain, and the anxiety for the onset of uncontrolled pain episodes. This situation derives from the health professionals not acknowledging the role of the caregivers and their work in pain management (30).
As regards the educational needs targeted to the activities of daily life, the caregivers do not receive any training on mobilization, lifting, change of positions in the bed, taking the patient to the bathroom, hygiene in the bed, care for the skin of the patient, or prescribed diet (25, 30). For this reason, they must learn them through the trial-and-error method, which exposes the patients and their caregivers to a high risk of physical injuries (31), as well as to feelings of frustration in the caregivers, due to the scarce feedback they receive on the success or failure of their efforts.
Regarding the invisibilization of the caregiver role, the literature reports that the non-inclusion of the role by the health professionals in the care processes for the patients generates in them anxiety and fear in relation to the responsibilities they must take on in the home, responsibilities for which they do not feel prepared (32-33). An example is the case of the caregivers stating that the health professionals do not listen to them, do not have time to talk and discuss care issues, and do not include them in decision-making, making them more vulnerable to stress and to uncertainty (33).
Likewise, non-inclusion and lack of recognition of the caregivers leads to a dynamics in which they do not want to disturb or hinder the work of the health professionals, for perceiving themselves as obstacles for the care provided (34); however, they expect that the health professionals establish an assertive, honest, simple, and empathetic communication on the patient’s condition, decision-making on the removal of futile treatments, and the expectations they can have about their care and end of life (35). In the caregivers, these behaviors increase self-confidence and reduce the feeling of being navigating with no defined course (36).
With respect to social support, the caregiver of a person in palliative care perceives its reduction as the disease progresses. Some studies show that its availability and quality decrease after a year of the diagnosis, which implies a great challenge for the caregivers of patients with pathologies like advanced cancer, who need stronger support systems as the disease progresses (37-38). The aforementioned generates in the caregivers consequences like job loss or reduction in the number of hours devoted to it, physical and emotional exhaustion, absence of an effective coping, and limited time for themselves (39).
Finally, various research studies concluded that uncertainty towards the disease is an influencing factor on the caregivers’ quality of life. In a study (40), it was found that uncertainty towards the patient’s disease was a weak negative predictor in the report of quality of life related to the health of the caregiver [r = -0.29, p = 0.002]. Likewise, another study (41) identified that, in family caregivers of adolescents with brain tumors, uncertainty was related to a reduction in the psychological dimension of quality of life. Another study (42) showed that, when fewer fears and doubts exist about the disease, uncertainty is low, the caregivers’ quality of life improves, and they better cope with the situation. Such aspects ratify the importance of the support that health professionals must provide to family caregivers.
Resources to manage uncertainty
The resources available for the caregiver play an important role in reducing uncertainty towards the disease, and are related to education for the caregiver, to social support, and to accompaniment by the health professionals.
Diverse studies support the importance of education in the reduction of uncertainty, among them Henson et al. (43), who discovered that the caregiver’s decision-making process about going to the urgency service with the patient derived from the education imparted by the health professionals. Additionally, Teno et al. (44) determined that lack of education made the caregivers feel excluded from the decisions about the patient’s treatment. They also found that some caregivers do not want to listen to opinions on the progress of the disease (45) or receive excess information; they rather reject the subject (46).
The studies presented coincide in considering education as a predictor of the caregiver’s overload (B.17, p = 0.017) (47). That is to say, the family caregivers of individuals in palliative care who have been advised on the disease, the treatments, the symptoms, and the probable outcome understand the situation they are facing and, by using their coping mechanisms, moderate the onset of the care burden and, consequently, the appearance of uncertainty towards the disease (48).
On the other hand, some studies show that social support modulates uncertainty in the caregiver. For example, those caregivers who managed to share their experiences and express their doubts and fears to people in their same situation consider themselves better prepared for providing care (p = 0.014) (49). Parallelly, those who have close friends or relatives who are health professionals, and who better explain to them the medical terms, learn to change their life perspectives and to feel validated in their duties (50). On the other hand, it has been proved that high levels of uncertainty are associated with a low perception of social support (r = -0.36, p < 0.05) (51), as well as with higher levels of anxiety and of depressive symptoms (52).
Finally, as regards the due accompaniment by the health professionals to the family caregivers of individuals in palliative care, it was evidenced that the caregivers experience uncertainty towards the disease when they resort to the health professional looking for answers they do not find: this frustrates them (53). Hence, as credible authorities, health professionals must be willing to listen to the caregivers and guide them in relation to their concerns. In this regard, another research study (54) concluded that, when the caregivers have the opportunity to talk to the health professionals about themes related to the patient’s disease, they feel recognized, empowered and supported, and this reduces their uncertainty towards the disease.
Uncertainty assessment
The context of the care provided to a person with an advanced disease and in palliative care differs from the conditions that arise when caring for someone with another chronic or critical disease, since the complexity of the care situation increases as the patient nears end of life. The assessment that the caregivers make about the uncertainty they experiment is often negative, that is, they evaluate it as a constant chaos where no relationship among the events experienced is perceived (55). For example, it has been found that uncertainty is assessed negatively when there is a daily fluctuation in the symptoms, such as pain in the patient (56).
In view of the panorama described, it is fundamental that the caregivers familiarize themselves with the situation, the disease, its evolution, and its care, which is attained with time and through experience. Those caregivers who do not receive information on the prognosis of their patients report high levels of uncertainty, as a result of facing reality differently than what they had expected (57), because they did not expect the patients’ conditions to worsen so markedly or for them to approach end of life so suddenly. Experiences like seeing that the patient was fine in the morning and then entered into an agony situation in the afternoon are frequent (58).
In contrast, some studies have found a positive assessment of uncertainty in contexts of less adverse diseases, with caregivers of patients under prolonged treatments (59). In these cases, as time passes, uncertainty is seen as an opportunity for personal growth and for strengthening the relationship with the loved one in palliative care. Added to this is the re-establishment of hope about new goals, the re-signification of the experience, and a better coping process for death and its subsequent grief (60-61).
Therapies and interventions to approach uncertainty
In the literature included in this review, few studies deal with uncertainty towards the disease in the family caregiver. Additionally, the few studies reported have not been effective in the approach of this phenomenon. The most representative study (62) applied an intervention to early- and late-stage cancer patients and their family caregivers. By means of three family visits lasting 90 minutes each and two telephonic sessions of 30 minutes each, it was found that the caregivers in the experimental group improved their negative assessment of the care provided after the intervention, but no changes were detected in the level of uncertainty towards the disease or in coping in either group. The author describes that these results were due to the fact that the research did not focus exclusively on patients in palliative care, who have special needs given the context of their advanced diseases, but also in patients with early stages of cancer.
The contributions of this research for the development of knowledge in Nursing are mainly related to describing the level of evidence around the five themes extracted for the review of the articles. As regards the characterization of uncertainty in the caregiver and the influencing factors, the findings allow the Nursing professionals to know the levels of uncertainty in palliative care and to identify some of its triggering factors. In the same sense, it describes the possibility of continuing researching the uncertainty levels by comparing them with other populations. In relation to the resources to manage uncertainty, the evidence shows that it is necessary to continuously train the caregivers on palliative care, as it is a basic resource for its management. Regarding the uncertainty assessment, the review shows the need to conduct systematic assessments of the level of uncertainty in the caregiver and, with this information, set forth therapies to approach it since, according to the results, few therapies and interventions have been set out to manage this phenomenon in the caregivers.
Conclusions
Uncertainty towards the disease of family caregivers of cancer patients in palliative care obeys multi-factorial causes such as knowledge on the disease, communication, recognition of their role in palliative care, fulfillment of needs, and social support. When caregivers experience uncertainty towards the disease, they are unable to determine the meaning of all its related events, that is, to assign definite values to objects and events, as well as to accurately predict consequences related to the disease, due to the scarcity of information and knowledge to do so.
The reviewed literature of a twenty-year period only reports a formal intervention for the management of uncertainty towards the disease. From this finding the need is interpreted of developing Nursing interventions that may offer accompaniment to the caregivers who experiment uncertainty towards the disease of patients in palliative care and, in the same way, impact on other variables, like their quality of life. Such interventions are necessary in contexts like the Colombian one, where the care provided to patients in palliative care and the accompaniment of their family caregivers are still precarious.
< p class="normal">Funding: This research has not received any specific help from public or commercial agencies, nor from any non-profit organization.Conflict of interests: None declared.
References
1. World Health Organization. Noncommunicable diseases country profiles, 2018. Ginebra: World Health Organization; 2018. [Citado 2019 dic. 20]. Disponible en: https://apps.who.int/iris/handle/10665/274512
2. World Health Organization. Definition of palliative care. Ginebra: World Health Organization; 2015. [Citado 2019 dic. 20]. Disponible en: http://www.who.int/cancer/palliative/definition/en/#
3. Garcia-Rueda N, Carvajal VA, Saracibar-Razquin M, Arantzamendi SM. The experience of living with advanced-stage cancer: A thematic synthesis of the literature. Eur J Cancer Care. 2016;25(3):551-69. DOI: https://doi.org/10.1111/ecc.12523
4. Arias-Rojas M, Carreño-Moreno S, Chaparro L. Incertidumbre ante la enfermedad crónica. Revisión integrativa. Rev Latinoam Bioética. 2019;19(36-1):91-104. DOI: https://doi.org/10.18359/rlbi.3575
5. Meleis AI, Sawyer LM, Im EO, Hilfinger Messias DK, Schumacher K. Experiencing transitions: An emerging middle-range theory. Adv Nurs Sci. 2000;23(5):12-28. DOI: https://doi.org/10.1097/00012272-200009000-00006
6. Carreño MS, Chaparro DL, Blanco SP. Cuidador familiar del niño con cáncer: un rol en transición. Rev Latinoam Bioética. 2017;17(33-2):18-30. DOI: https://doi.org/10.18359/rlbi.2781
7. Moreno CS, Palomino MP, Moral FL, Frías OA, Del Pino CR. Problemas en el proceso de adaptación a los cambios en personas cuidadoras familiares de mayores con demencia. Gac Sanit. 2016;30(7):201-7. DOI: https://doi.org/10.1016/j.gaceta.2016.02.004
8. Holm M, Årestedt K, Öhlen J, Alvariza A. Variations in grief, anxiety, depression, and health among family caregivers before and after the death of a close person in the context of palliative home care. Death Stud. 2019(8);23:1-9. DOI: https://doi.org/10.1080/07481187.2019.1586797
9. Gotze H, Brahler E, Gansera L, Schnabel A, Gottschalk-Fleischer A, Kohler N. Anxiety, depression and quality of life in family caregivers of palliative cancer patients during home care and after the patient’s death. Eur J Cancer Care. 2018;27(9)(2):e12606. DOI: https://doi.org/10.1111/ecc.12606
10. Domínguez JA, Ruíz M, Gómez I, Gallego E, Valero J, Izquierdo MT. Ansiedad y depresión en cuidadores de pacientes dependientes. Semergen. 2012;38(10):16-23. DOI: https://doi.org/10.1016/j.semerg.2011.05.013
11. Clayton M, Dean M, Mishel M. Theories of uncertainty in illness. En: Smith MJ, Liehr P, editoras. Middle range theory for nursing. 4.ª ed. Nueva York: Springer Publishing Company; 2018. p. 49-82.
12. Peters MD, Godfrey CM, Khalil H, McInerney P, Parker D, Soares CB. Guidance for conducting systematic scoping reviews. Int J Evid Based Healthc. 2015;13(12)(3):1416. DOI: https://doi.org/10.1097/XEB.0000000000000050
13. Joanna Briggs Institute. Levels of evidence. South Australia: The University of Adelaide; 2013 [Citado 2019 dic. 10]. Disponible en: https://joannabriggs.org/sites/default/files/2019-05/JBI-Levels-of-evidence_2014_0.pdf
14. Critical Appraisal Skills Programme Español (CASPe). Instrumentos para lectura crítica: herramientas para análisis de reportes de investigación. Alicante, España: CASPe; 2016. [Citado 2019 dic. 10]. Disponible en: http://www.redcaspe.org/herramientas/instrumentos
15. Northouse LL, Mood DW, Montie JE, Sandler HM, Forman JD, Hussain M, et al. Living with prostate cancer: Patients’ and spouses’ psychosocial status and quality of life. J Clin Oncol. 2007;25(15):4171-7. DOI: https://doi.org/10.1200/JCO.2006.09.6503
16. Arias-Rojas M, Carreño–Moreno S, Posada C. Incerteza dos cuidadores familiares na doença de pacientes sob cuidados paliativos e fatores associados. Rev Latino-Am Enferm. 2019;27(16):e3200. DOI: https://doi.org/10.1590/1518-8345.3185.3200
17. Kimbell B, Boyd K, Kendall M, Iredale J, Murray SA. Managing uncertainty in advanced liver disease: A qualitative, multiperspective, serial interview study. BMJ Open. 2015;5(17):e009241.DOI: http://doi.org/10.1136/bmjopen-2015-009241
18. Hudson PL, Aranda S, Kristjanson LJ. Meeting the supportive needs of family caregivers in palliative care: Challenges for health professionals. J Palliat Med. 2004;7(18):19-25. DOI: https://doi.org/10.1089/109662104322737214
19. Wang T, Molassiotis A, Chung BPM, Tan J-Y. Unmet care needs of advanced cancer patients and their informal caregivers: A systematic review. BMC Palliat Care. 2018;17(1):96. DOI: https://doi.org/10.1186/s12904-018-0346-9
20. Hudson PL, Remedios C, Thomas K. A systematic review of psychosocial interventions for family carers of palliative care patients. BMC Palliat Care. 2010;9:17. DOI: https://doi.org/10.1186/1472-684X-9-17
21. Candy B, Jones L, Drake R, Leurent B, King M. Interventions for supporting informal caregivers of patients in the terminal phase of a disease. Cochrane database Syst Rev. 2011;(21):CD007617. DOI: https://doi.org/10.1002/14651858.CD007617.pub2
22. Zavagli V, Raccichini M, Ercolani G, Franchini L, Varani S, Pannuti R. Care for carers: An investigation on family caregivers’ needs, tasks, and experiences. Transl Med UniSa. 2019;19(22):54-9. Disponible en: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6581485/
23. Haley WE, LaMonde LA, Han B, Narramore S, Schonwetter R. Family caregiving in hospice: Effects on psychological and health functioning among spousal caregivers of hospice patients with lung cancer or dementia. Hosp J. 2001;15(23):1-18. DOI: https://doi.org/10.1080/0742-969x.2000.11882959
24. Cortijo PX, Ortíz AG, Cibrián LT. Comparación psicoafectiva entre cuidadores principales de pacientes psiquiátricos y con cáncer en estadios avanzados de la enfermedad. Rev Acta Médica del Cent. 2019;13(24):93-100. Disponible en: http://www.revactamedicacentro.sld.cu/index.php/amc/article/view/980/1243
25. Rabow MW, Hauser JM, Adams J. Perspectives on care at the close of life. Supporting family caregivers at the end of life: “They don’t know what they don’t know.” J Am Med Assoc. 2004;291(25):483-91. DOI: https://doi.org/10.1001/jama.291.4.483
26. Murray SA, Boyd K, Kendall M, Worth A, Benton TF, Clausen H. Dying of lung cancer or cardiac failure: Prospective qualitative interview study of patients and their careers in the community. BMJ Br Med J. 2002;325(7370):929-32. DOI: https://doi.org/10.1136/bmj.325.7370.929
27. Collins A, McLachlan SA, Philip J. How should we talk about palliative care, death and dying? A qualitative study exploring perspectives from caregivers of people with advanced cancer. Palliat Med. 2018;32(27):861-9.DOI: https://doi.org/10.1177/0269216317746584
28. Gardner DS. Cancer in a dyadic context: Older couples’ negotiation of ambiguity and search for meaning at the end of life. J Soc Work End Life Palliat Care. 2008;4(28):135-59.DOI: https://doi.org/10.1080/15524250802353959
29. Garcia-Toyos N, Escudero-Carretero MJ, Sanz-Amores R, Guerra-De Hoyos JA, Melchor-Rodriguez JM, Tamayo-Velazquez MI. Preferences of caregivers and patients regarding opioid analgesic use in terminal care. Pain Med. 2014;15(29):577-87. DOI: https://doi.org/10.1111/pme.12376
30. Wennman-Larsen A, Tishelman C. Advanced home care for cancer patients at the end of life: A qualitative study of hopes and expectations of family caregivers. Scand J Caring Sci. 2002;16(3):240-7. DOI: https://doi.org/10.1046/j.1471-6712.2002.00091.x
31. Hasson F, Kernohan WG, McLaughlin M, Waldron M, McLaughlin D, Chambers H, et al. An exploration into the palliative and end-of-life experiences of carers of people with Parkinson’s disease. Palliat Med. 2010;24(7):731-6. DOI: https://doi.org/10.1177/0269216310371414
32. McIlfatrick S. Assessing palliative care needs: Views of patients, informal carers and healthcare professionals. J Adv Nurs. 2007;57(1):77-86. DOI: https://doi.org/10.1111/j.1365-2648.2006.04062.x
33. Hanratty B, Holmes L, Lowson E, Grande G, Addington-Hall J, Payne S, et al. Older adults’ experiences of transitions between care settings at the end of life in England: A qualitative interview study. J Pain Symptom Manage. 2012;44(1):74-83. DOI: https://doi.org/10.1016/j.jpainsymman.2011.08.006
34. Printz C. Cancer caregivers still have many unmet needs. Cancer. 2011;117(7):1331. DOI: https://doi.org/10.1002/cncr.26075
35. Steinhauser KE, Christakis NA, Clipp EC, McNeilly M, Grambow S, Parker J, et al. Preparing for the end of life: Preferences of patients, families, physicians, and other care providers. J Pain Symptom Manage. 2001;22(3):727-37. DOI: https://doi.org/10.1016/s0885-3924(01)00334-7
36. Lee HTS, Melia KM, Yao CA, Lin CJ, Chiu TY, Hu WY. Providing hospice home care to the terminally ill elderly people with cancer in Taiwan: Family experiences and needs. Am J Hosp Palliat Care. 2014;31(6):628-35 DOI: https://doi.org/10.1177/1049909113499603
37. Arora NK, Finney Rutten LJ, Gustafson DH, Moser R, Hawkins RP. Perceived helpfulness and impact of social support provided by family, friends, and health care providers to women newly diagnosed with breast cancer. Psychooncology. 2007;16(5):474-86. DOI: https://doi.org/10.1002/pon.1084
38. Cardoso F, Harbeck N, Mertz S, Fenech D. Evolving psychosocial, emotional, functional, and support needs of women with advanced breast cancer: Results from the Count Us, Know Us, Join Us and Here & Now surveys. Breast. 2016;28:5-12. DOI: https://doi.org/10.1016/j.breast.2016.04.004
39. Tallman K, Greenwald R, Reidenouer A, Pantel L. Living with advanced illness: Longitudinal study of patient, family, and caregiver needs. Perm J. 2012;16(3):28-35. DOI: https://doi.org/10.7812/tpp/12-029
40. Fortier MA, Batista ML, Wahi A, Kain A, Strom S, Sender LS. Illness uncertainty and quality of life in children with cancer. J Pediatr Hematol Oncol. 2013;35(5):366-70. DOI: https://doi.org/10.1097/MPH.0b013e318290cfdb
41. Buchbinder DK, Fortier MA, Osann K, Wilford J, Shen V, Torno L, et al. Quality of life among parents of adolescent and young adult brain tumor survivors. J Pediatr Hematol Oncol. 2017;39(8):579-84. DOI: https://doi.org/10.1097/MPH.0000000000000947
42. Kershaw TS, Mood DW, Newth G, Ronis DL, Sanda MG, Vaishampayan U, et al. Longitudinal analysis of a model to predict quality of life in prostate cancer patients and their spouses. Ann Behav Med. 2008;36(2):117-28. DOI: https://doi.org/10.1007/s12160-008-9058-3
43. Henson LA, Higginson IJ, Daveson BA, Ellis-Smith C, Koffman J, Morgan M, et al. “I’ll be in a safe place”: A qualitative study of the decisions taken by people with advanced cancer to seek emergency department care. BMJ Open. 2016;6(11):e012134. DOI: https://doi.org/10.1136/bmjopen-2016-012134
44. Teno JM, Casey VA, Welch LC, Edgman-Levitan S. Patient-focused, family-centered end-of-life medical care: Views of the guidelines and bereaved family members. J Pain Symptom Manage. 2001;22(3):738-51. DOI: https://doi.org/10.1016/s0885-3924(01)00335-9
45. Sparla A, Flach-Vorgang S, Villalobos M, Krug K, Kamradt M, Coulibaly K, et al. Individual difficulties and resources: A qualitative analysis in patients with advanced lung cancer and their relatives. Patient Prefer Adherence. 2016;10:2021-9. DOI: https://doi.org/10.2147/PPA.S110667
46. Collier A, Breaden K, Phillips JL, Agar M, Litster C, Currow DC. Caregivers’ perspectives on the use of long term oxygen therapy for the treatment of refractory breathlessness: A qualitative study. J Pain Symptom Manage. 2017;53(1):33-39. DOI: https://doi.org/10.1016/j.jpainsymman.2016.06.007
47. Vahidi M, Mahdavi N, Asghari E, Ebrahimi H, Eivazi Ziaei J, Hosseinzadeh M, et al. Other side of breast cancer: Factors associated with caregiver burden. Asian Nurs Res. 2016;10(3):201-6. DOI: https://doi.org/10.1016/j.anr.2016.06.002
48. Borneman T, Sun V, Williams AC, Fujinami R, Del Ferraro C, Burhenn PS, et al. Support for patients and family caregivers in lung cancer: Educational components of an interdisciplinary palliative care intervention. J Hosp Palliat Nurs. 2015;17(4):309-18. DOI: https://doi.org/10.1097/NJH.0000000000000165
49. Hudson PL, Trauer T, Lobb E, Zordan R, Williams A, Quinn K, et al. Supporting family caregivers of hospitalised palliative care patients: A psychoeducational group intervention. BMJ Support Palliat Care. 2012;2(2):115-20. DOI: https://doi.org/10.1136/bmjspcare-2011-000131
50. Waldrop DP, Kramer BJ, Skretny JA, Milch RA, Finn W. Final transitions: Family caregiving at the end of life. J Palliat Med. 2005;8(3):623-38. DOI: https://doi.org/10.1089/jpm.2005.8.623
51. Germino BB, Mishel MH, Belyea M, Harris L, Ware A, Mohler J. Uncertainty in prostate cancer. Ethnic and family patterns. Cancer Pract. 1998;6(2):107-13. DOI: https://doi.org/10.1046/j.1523-5394.1998.1998006107.x
52. Ling SF, Chen ML, Li CY, Chang WC, Shen WC, Tang ST. Trajectory and influencing factors of depressive symptoms in family caregivers before and after the death of terminally ill patients with cancer. Oncol Nurs Forum. 2013;40(1):E32-40. DOI: https://doi.org/10.1188/13.ONF.E32-E40
53. Richardson A, Wagland R, Foster R, Symons J, Davis C, Boyland L, et al. Uncertainty and anxiety in the cancer of unknown primary patient journey: A multiperspective qualitative study. BMJ Support Palliat Care. 2015;5(4):366-72. DOI: https://doi.org/10.1136/bmjspcare-2013-000482
54. Aoun SM, Deas K, Howting D, Lee G. Exploring the support needs of family caregivers of patients with brain cancer using the CSNAT: A comparative study with other cancer groups. PLoS One. 2015;10(12):e0145106. DOI: https://doi.org/10.1371/journal.pone.0145106
55. Kendall M, Carduff E, Lloyd A, Kimbell B, Cavers D, Buckingham S, et al. Different experiences and goals in different advanced diseases: Comparing serial interviews with patients with cancer, organ failure, or frailty and their family and professional carers. J Pain Symptom Manage. 2015;50(2):216-24. DOI: https://doi.org/10.1016/j.jpainsymman.2015.02.017
56. Butow PN, Price MA, Bell ML, Webb PM, DeFazio A, Friedlander M. Caring for women with ovarian cancer in the last year of life: A longitudinal study of caregiver quality of life, distress and unmet needs. Gynecol Oncol. 2014;132(3):690-7. DOI: https://doi.org/10.1016/j.ygyno.2014.01.002
57. Bristowe K, Carey I, Hopper A, Shouls S, Prentice W, Caulkin R, et al. Patient and carer experiences of clinical uncertainty and deterioration, in the face of limited reversibility: A comparative observational study of the AMBER care bundle. Palliat Med. 2015;29(9):797-807. DOI: https://doi.org/10.1177/0269216315578990
58. Wordingham SE, McIlvennan CK, Dionne-Odom JN, Swetz KM. Complex care options for patients with advanced heart failure approaching end of life. Curr Heart Fail Rep. 2016;13(1):20-9. DOI: https://doi.org/10.1007/s11897-016-0282-z
59. Kang Y. Effect of uncertainty on depression in patients with newly diagnosed atrial fibrillation. Prog Cardiovasc Nurs. 2006;21(2):83-8. DOI: https://doi.org/10.1111/j.0889-7204.2006.04810.x
60. Daneault S, Lussier V, Mongeau S, Yelle L, Cote A, Sicotte C, et al. Ultimate journey of the terminally ill: Ways and pathways of hope. Can Fam Physician. 2016;62(8):648-56. Disponible en: https://pubmed.ncbi.nlm.nih.gov/27521394-ultimate-journey-of-the-terminally-ill-ways-and-pathways-of-hope/
61. Bjork M, Sundler AJ, Hallstrom I, Hammarlund K. Like being covered in a wet and dark blanket: Parents’ lived experiences of losing a child to cancer. Eur J Oncol Nurs. 2016;25:40-5.DOI: https://doi.org/10.1016/j.ejon.2016.08.007
62. Northouse L, Kershaw T, Mood D, Schafenacker A. Effects of a family intervention on the quality of life of women with recurrent breast cancer and their family caregivers. Psychooncology. 2005;14(6):478-91. DOI: https://doi.org/10.1002/pon.871