

|
ARTICLE
Yasmin Vitória dos Santos Rodrigues 1
Camila Moraes Garollo Piran 2
Alana Vitória Escritori Cargnin 3
Mariana Martire Mori 4
Viviane Cazetta de Lima Vieira 5
Marcela Demitto Furtado 6
1 Universidade Estadual de Maringá, Brazil
![]() 0009-0002-9926-2491
0009-0002-9926-2491
![]() yasmin18vitoria1818@gmail.com
yasmin18vitoria1818@gmail.com
2 Universidade Estadual de Maringá, Brazil
![]() 0000-0002-9111-9992
0000-0002-9111-9992
![]() camilagarollo@gmail.com
camilagarollo@gmail.com
3 https://orcid.org/0000-0002-7733-2420 Universidade Estadual de Maringá, Brazil
![]() 0009-0002-9926-2491
0009-0002-9926-2491
![]() alanaescritori@gmail.com
alanaescritori@gmail.com
4 Universidade Estadual de Maringá, Brazil
![]() 0000-0003-1744-3580
0000-0003-1744-3580
![]() mari_mmori@hotmail.com
mari_mmori@hotmail.com
5 Universidade Estadual de Maringá, Brazil
![]() 0000-0003-3029-361X
0000-0003-3029-361X
![]() vclvieira2@uem.br
vclvieira2@uem.br
6 Universidade Estadual de Maringá, Brazil
![]() 0000-0003-1427-4478
0000-0003-1427-4478
![]() mdfurtado@uem.br
mdfurtado@uem.br
* This work was conducted with the support of the Araucária Foundation and the Institutional Program for Scientific Initiation Scholarships, through the National Council for Scientific and Technological Development, Brazil.
** El trabajo se realizó con el apoyo de la Fundação Araucária y el Programa Institucional de Bolsas de Iniciação Científica, a través del Conselho Nacional de Desenvolvimento Científico e Tecnológico, Brasil.
*** Este trabalho foi realizado com o apoio da Fundação Araucária e do Programa Institucional de Bolsas de Iniciação Científica, por meio do Conselho Nacional de Desenvolvimento Científico e Tecnológico, Brasil.
Theme: Healthcare technologies
Contributions to the field: The mapping of scientific evidence regarding photobiomodulation in the healthcare of neonates and children, through a scoping review, contributes to gathering references that enable understanding the benefits of applying the technique and its broad spectrum of action. It is a promising non-pharmacological treatment in healthcare, which is easy to apply and contributes to the practice of nurses and other healthcare professionals by assisting in pain management, injury prevention, and tissue repair.
Received: 25/09/2024
Sent to peers: 09/12/2025
Approved by peers: 01/06/2025
Accepted: 03/06/2025
To reference this article / Para citar este artículo / Para citar este artigo Rodrigues YVS, Piran CMG, Cargnin AVE, Mori MM, Vieira VCL, Furtado MD. Photobiomodulation in Neonatal and Pediatric Healthcare: A Scoping Review. Aquichan. 2025;25(3):e2535. DOI: https://doi.org/10.5294/aqui.2025.25.3.5
Introduction: Photobiomodulation is a noninvasive therapy used with neonates and children, with promising results due to its analgesic, antimicrobial, and reparative actions.
Objective: To describe the available evidence on the use of photobiomodulation in nursing care for neonates and children.
Materials and Methods: This is a structured scoping review based on the methodological guidelines of the Joanna Briggs Institute. The PCC mnemonic was applied, where P stands for population (neonates and children), C for concept (photobiomodulation), and C for context (healthcare). The databases searched were Web of Science, Science Direct, Embase, PubMed via MEDLINE, LILACS, BDEnf, WPRIM, and IBECS via the Virtual Health Library (VHL); in addition to the repositories: Preprints bioRxiv, Thesis and Dissertation Catalog, and OpenGrey. The results followed the guidelines from the Preferred Reporting Items for Systematic Reviews and Meta-Analyses Extension for Scoping Reviews (PRISMA-ScR) checklist.
Results: The final sample consisted of 11 studies, with a focus on diode laser application, all developed in the field of dentistry. It was evident that photobiomodulation is a promising and effective non-pharmacological method in nursing care for neonates and children.
Conclusions: Photobiomodulation has a broad spectrum of action and is consolidating itself as a promising, safe, and easily applicable non-pharmacological treatment in child health care.
Keywords (Source: DeCS): Laser therapy; low-level light therapy; child; newborn; child health
Resumen
Introducción: La fotobiomodulación es una terapia no invasiva utilizada en neonatos y niños, con resultados prometedores debido a sus efectos analgésicos, antimicrobianos y reparadores.
Objetivo: Describir la evidencia disponible sobre el uso de la fotobiomodulación en los cuidados de enfermería dirigidos a recién nacidos y niños.
Materiales y métodos: Se realizó una revisión de alcance estructurada según las directrices metodológicas del Instituto Joanna Briggs. Se aplicó el mnemotécnico PCC, en el que P corresponde a la población (neonatos y niños); C, al concepto (fotobiomodulación); y C al contexto (atención en salud). Las bases de datos consultadas fueron: Web of Science, Science Direct, Embase, PubMed vía MEDLINE, LILACS, BDEnf, WPRIM e IBECS a través de la Biblioteca Virtual en Salud (BVS); además de los repositorios: preprints bioRxiv, Catálogo de Teses e Dissertações y OpenGrey. Los resultados se reportaron conforme a las recomendaciones de la lista de verificación Preferred Reporting Items for Systematic Reviews and Meta-Analyses Extension for Scoping Reviews (PRISMA-ScR).
Resultados: La muestra final incluyó 11 estudios, con predominancia en la aplicación de láser de diodo, todos desarrollados en el área odontológica. Se evidenció que la fotobiomodulación es un método no farmacológico prometedor y eficaz en el cuidado de neonatos y niños.
Conclusiones: La fotobiomodulación posee un amplio espectro de acción y se consolida como un tratamiento no farmacológico prometedor, seguro y de fácil aplicación en la atención en salud infantil.
Palabras clave (Fuente: DeCS): Terapia con láser; terapia con luz de baja intensidad; niño; recién nacido; salud del niño
Introdução: A fotobiomodulação é uma terapia não invasiva utilizada com neonatos e crianças, com resultados promissores devido às suas ações analgésica, antimicrobiana e reparadora.
Objetivo: Descrever as evidências disponíveis sobre o uso da fotobiomodu-lação na assistência de enfermagem a recém-nascidos e crianças.
Materiais e métodos: Trata-se de uma revisão de escopo estruturada conforme orientações metodológicas do Instituto Joanna Briggs. Aplicou-se o mnemônico PCC, em que P se refere à população (neonatos e crianças); C, ao conceito (fotobiomodulação); e C, ao contexto (cuidado à saúde). As bases de dados consultadas foram: Web of Science, Science Direct, Embase, PubMed via MEDLINE, LILACS, BDEnf, WPRIM e IBECS via Biblioteca Virtual em Saúde (BVS); além dos repositórios: Preprints bioRxiv, Catálogo de Teses e Dissertações e OpenGrey. Os resultados seguiram as recomendações do checklist do Preferred Reporting Items for Systematic Reviews and Meta-Analyses Extension for Scoping Reviews (PRISMA-ScR).
Resultados: A amostra final foi composta por 11 estudos, com predominância da aplicação do laser de diodo, todos desenvolvidos na área da odontologia. Evidenciou-se que a fotobiomodulação é um método não farmacológico promissor e eficaz na assistência de enfermagem a neonatos e crianças.
Conclusões: A fotobiomodulação apresenta um amplo espectro de ação e vem se consolidando como um tratamento não farmacológico promissor, seguro e de fácil aplicabilidade na assistência à saúde infantil.
Palavras-chave (Fonte DeCS): Terapia a laser; terapia com luz de baixa intensidade; criança; recém-nascido; saúde da criança
Introduction
Photobiomodulation (PBM), also known as low-level laser therapy (LLLT) or light-emitting diode (LED) therapy, has gained interest in the health field for being a non-invasive tool 1 with satisfactory short-term results. Its applicability in vulnerable populations, such as neonates and children, has drawn attention due to the possibility of safe, painless, and well-tolerated interventions. Although the terms are often used interchangeably in the literature, in this study, the term "photobiomodulation" is adopted as the standard designation, as it is more comprehensive and current 2-4.
The first laser device was developed in 1959 to accelerate the regeneration of damaged tissue, promoting nerve response to restore the action potential threshold, and stimulating adjacent or contralateral neuromodulation to perform the role of the injured nerve 4.
It is a therapeutic approach capable of regulating numerous metabolic processes through biochemical and photophysical resources. PBM has the propensity to promote biological effects, such as pain relief 5. These characteristics make the technique appealing for use in children, as it avoids the side effects typical of conventional and invasive treatments. The ability to modulate the inflammatory process promotes the repair of injured tissue, stimulating the increase of growth factors, such as the stimulation of endothelial cells and fibroblasts, in addition to promoting the proliferation of keratinocytes 1,6.
PBM consists of applying light to a biological system, relieving pain, promoting tissue regeneration, and reducing inflammation. Unlike other procedures that use lasers, LLLT has no ablative or thermal effects. Instead, it causes a photochemical effect, in which light is absorbed and results in a chemical reaction 2. It is classified as a low-level technique due to the low energy density used, and these ideal levels are not comparable to those of other laser therapy techniques used for cutting, thermal coagulation of tissues, and even ablation 7.
PBM has also been widely used in healthcare as it uses monochromatic radiation and has a wider spectral range. Laser waves allow for more precise collimation, while LED waves are incoherent, enabling the treatment of larger areas 8.
The intensity of the PBM effect is affected by wavelength, energy density (fluence), power density, lesion type, and photoreceptor absorption spectrum 9. However, the main difference between laser types is related to the wavelength spectrum 1,6.
PBM emerged as a complementary alternative to conventional therapies and has presented several advantages, including being painless, providing rapid pain relief, being practical to use, cost-effective, and promoting good healing. It is also an appropriate alternative for pediatric patients, due to the low level of fear associated with the device and technique 2,10.
PBM has the potential to alleviate pain and inflammation, promote healing, and facilitate tissue regeneration 11,12. Due to its numerous benefits, it has been applied as an auxiliary treatment for various pathologies 11,13,14.
Since PBM is an innovative method that is increasingly present in healthcare practices, and there is a scarcity of systematic studies on the use of PBM in neonates and children, this study aims to describe the available evidence on the use of PBM in nursing care for neonates and children.
Unlike other reviews, which address PBM in general clinical contexts or in other populations, this review focuses specifically on the pediatric and neonatal population, with an emphasis on the nursing practice. This delimitation aims to contribute to scientific production in this field and guide evidence-based clinical practices.
Materials and Methods
This is a scoping review, characterized as a systematic, exploratory review, which aims to explore the concepts of the theme in question, in addition to understanding the scope and nature of the studies, as well as mapping and highlighting existing gaps in the literature 15.
To formulate the research question, the PCC mnemonic strategy was used, where P stands for population (neonates and children), C stands for concept (PBM), and C stands for context (health care) 15. Given this, the following question was formulated: What scientific evidence is available on the use of PBM in the health care of neonates and children?
The search for materials was conducted by two independent researchers between January and February 2024. Studies whose population consisted of individuals aged 0 to 12 years were included, and the sample selection was guided by the following inclusion criteria: articles without language restrictions; with or without free access; studies with varying methodological designs; no time frame, and manuals, theses, dissertations, and legislation. The exclusion criteria included studies that used PBM in combination with other treatments (due to possible interference with the observed effects), studies without presentation of results, works with incomplete information that compromised the thematic analysis, as well as letters to the editor, abstracts, event proceedings, and documents not available in full, even after contacting the authors. The Rayyan® software was used to manage the references.
The study selection was conducted independently by two reviewers. Discrepancies in the inclusion or exclusion of studies were settled by consensus between the reviewers and, when necessary, with the participation of a third reviewer. Data extraction was also performed independently by both reviewers, with cross-checking to ensure consistency of information.
The adapted Joanna Briggs Institute tool was used in the data extraction stage, covering aspects such as title, publication year, author(s), objective, methodological design, and main results. Although these categories guided the initial extraction, the process was conducted iteratively, allowing for adjustments as the data were analyzed, in line with the exploratory nature of the scoping review 15.
The descriptors were defined after searching the following electronic databases: Web of Science and PubMed via MEDLINE, to identify key terms related to the topic under study and, based on them, select controlled descriptors using the Health Sciences Descriptors (DeCS) and Medical Subject Headings (MeSH) tools: terapia a laser/laser therapy; terapia com luz de baixa intensidade/low-level light therapy; criança/child; saúde da criança/child health; cuidado da criança/child care; recémnascido/infant newborn. As uncontrolled descriptors, the following were used: /otobiomodulação/photobio-modulation; and neonato/neonate.
The research sources were Web of Science, Science Direct, Embase, PubMed via MEDLINE, LILACS, BDEnf, WPRIM, IBECS via the Virtual Health Library (VHL); in addition to the repositories: Preprints bioRxiv, Thesis and Dissertation Catalog of the Coordination for the Improvement of Higher Education Personnel (Capes) and Open-Grey. The references of the selected articles were analyzed to identify other studies.
The following search operators were used to develop the search engine: ("Laser Therapy" OR "Low-Level Light Therapy" OR "photobiomodulation") AND ("Child" OR "Child Health" OR "Child Care" OR "Infant Newborn" OR "neonate"), as shown in Table 1.
Table 1 Search Strategies in Databases and Repositories
Database |
Strategy |
No. |
|---|---|---|
LILACS, BDEnf, WPRIM, IBECS via BVS |
(("laser therapy" OR "low-level light therapy" OR "photobiomodulation") AND ("child" OR "child health" OR "child care" OR "infant newborn" OR "neonate")) AND (db:("WPRIM" OR "LILACS" OR "IBECS" OR "BDEnf")) |
385 |
PubMed via MEDLINE |
("Laser Therapy"[All Fields] OR "Low-Level Light Therapy"[All Fields] OR "photobiomodulation"[All Fields]) AND ("Child"[All Fields] OR "Child Health"[All Fields] OR "Child Care"[All Fields] OR "Infant Newborn"[All Fields] OR "neonate"[All Fields]) |
4147 |
Web of Science |
ALL= ((("Laser Therapy" OR "Low-Level Light Therapy" OR "photobiomodulation") AND ("Child" OR "Child Health" OR "Child Care" OR "Infant Newborn" OR "neonate"))) |
266 |
Science Direct |
ALL= ((("Laser Therapy" OR "Low-Level Light Therapy" OR "photobiomodulation") AND ("Child" OR "Child Health" OR "Child Care" OR "Infant Newborn" OR "neonate"))) |
3933 |
Embase |
((("Laser Therapy" OR "Low-Level Light Therapy" OR "photobiomodulation") AND ("Child" OR "Child Health" OR "Child Care" OR "Infant Newborn" OR "neonate")))('laser therapy' OR 'low-level light therapy' OR 'photobiomodulation') AND ('child' OR 'child health' OR 'child care' OR 'infant newborn' OR 'neonate') |
2732 |
OpenGrey |
((("Laser Therapy" OR "Low-Level Light Therapy" OR "photobiomodulation") AND ("Child" OR "Child Health" OR "Child Care" OR "Infant Newborn" OR "neonate"))) |
292 |
Preprints bioRxiv |
Laser Therapy OR Low-Level Light Therapy OR photobiomodulation AND Child OR Child Health OR Child Care OR Infant Newborn |
3 |
Capes Catalog ofTheses and Dissertations |
((("Laser Therapy" OR "Low-Level Light Therapy" OR "photobiomodulation") AND ("Child" OR "Child Health" OR "Child Care" OR "Infant Newborn" OR "neonate"))) |
68 |
Source: Prepared by the authors.
Following this, a thematic analysis was conducted to identify the potentialities and gaps in the theme. The summary of the results is presented in tables with the main findings, which are discussed narratively. Finally, the study presents the results following the suggestions of the PRISMA-ScR 16 checklist, as shown in Figure 1. The review protocol is registered in the Open Science Framework, under number 10.17605/OSF.IO/WAZUM.
Figure 1 PRISMA-ScR Flowchart for Identifying and Selecting Articles Included in the Scoping Review Using Information Sources. Maringá, Paraná, Brazil, 2024
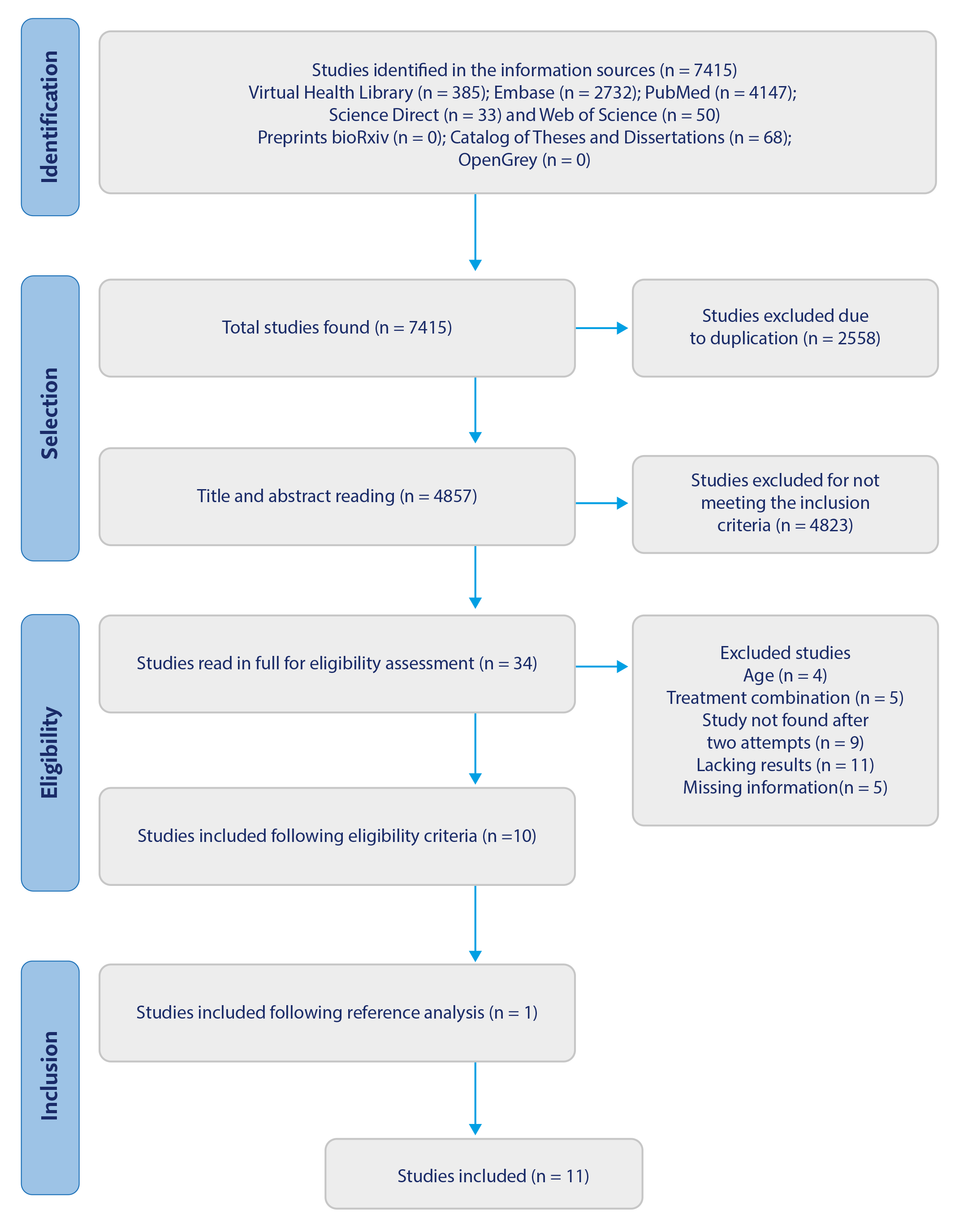
Source: Adapted from PRISMA-ScR 16.
Key: Combination treatment - studies that combined PBM with a clinical protocol, a combination of low- and high-intensity lasers, medications, analgesics, or therapy; No results - these are proposals for studies that have not yet been completed and, therefore, the results have not been described; Missing information - these are studies that did not provide necessary information, such as the age and type of laser used.
Since this is a scoping review based on publicly available secondary data, it was not necessary to submit it to a research ethics committee, in compliance with national and international guidelines for research of this nature.
Results
The final sample consisted of 11 studies. Table 2 shows the articles included, according to general characteristics: authorship, publication year, country where the study was conducted, objective, study design, location, and participants' age, according to the methodological criteria proposed by the scoping review, highlighting the characteristics of contexts, populations, interventions, and outcomes observed.
Table 2 Studies Included in the Review. Maringá, Paraná, Brazil, 2024
ID |
Authorship/Year |
Country |
Objective |
Study design |
Location |
Age |
Funding |
|---|---|---|---|---|---|---|---|
A1 17 |
McLoone E, O'Keefe M, McLoone S, Lanigan B/2006 |
Ireland |
To evaluate the long-term functional and structural outcomes of premature neonates who underwent diode laser photocoagulation for retinopathy of prematurity. |
Cohort study |
Ophthalmology Clinic at the Children's Hospital |
Average age of 11 years |
Not declared |
A2 18 |
Kuhn A, Porto FA, Miraglia P, Brunetto, AL/2008 |
Brazil |
To determine whether LLLT can reduce the duration of chemotherapy-induced oral mucositis. |
Controlled and randomized |
Pediatric Oncology Service at Hospital de Clínicas |
Average age of 8.2 years |
Not declared |
A3 19 |
Pinto FC, Chavantes MC, Pinto NC, Alho EJ, Yoshimura EM, Matushita H et al./2010 |
Brazil |
To analyze the effect of LLLT on tissue repair following corrective surgical incision in neonates with myelomeningocele. |
Prospective pilot study |
Pediatric Nursery at the Hospital de Clínicas |
Neonates |
Not declared |
A4 20 |
Cepera F, Torres FC, Scanavini MA, Paranhos LR, Capelozza L, Cardoso MA et al./2012 |
Brazil |
To evaluate the effects of low-intensity laser on bone regeneration in rapid maxillary expansion procedures. |
Comparative study, controlled and randomized trial |
Orthodontic clinic |
Ages 8 and 11 |
Not declared |
A5 21 |
Cauwels R, Martens L, Van De Velde V, Benoit Y/2013 |
Belgium |
To research the pain relief and wound healing capabilities of LLLT in chemotherapy-induced oral mucositis. |
Pilot study | University Hospital |
Average age of 9,4 years |
Not declared |
A6 22 |
Stein S, Korbmacher-Steiner H, Popovic N, Braun A/2015 |
Germany |
Pain-reducing effect of low-intensity laser therapy in pediatric patients undergoing orthodontic separation. |
Retrospective and randomized study |
Orthodontic clinic |
Average age of 8.05 years |
Not declared |
A7 23 |
Elbay M, Tak Ö, Çermet Elbay EUA, Kaya C, Eryilmaz K/2016 |
Turkey |
To determine whether LLLT can reduce the gag reflex in children undergoing intraoral radiography of the maxilla. |
Randomized, controlled, double-blind clinical trial |
Pediatric Dentistry Center |
Ages 6 to 12 |
Not declared |
A8 24 |
Vieira KA, Bastos CM, Vitor MGC, Deana AM, Fernandes KPS, Rodrigues MFSD et al./2018 |
Brazil |
To evaluate the effect of low-power laser on saliva in children aged 1 to 5 years with protein-energy malnutrition. |
Cross-sectional experimental study |
Educational and Nutritional Recovery Center |
Ages 1 to 5 |
Not declared |
A9 25 |
Bardellini E, Veneri F, Amadori F, Conti G, Majorana A/2020 |
Italy |
To evaluate the effectiveness of PBM in relieving pain and reducing lesions in children with recurrent aphthous stomatitis. |
Controlled and randomized study |
Orthodontic clinic |
Ages 5 to 12 |
Not declared |
A10 26 |
Oliveira AB, Ferrisse TM, Salomão KB, Miranda ML, Bufalino A, Brighent FL/2021 |
Brazil |
To evaluate the effectiveness of PBM therapy for the treatment of xerostomia associated with hyposalivation. |
Case report |
Pediatric clinic |
7 years |
Capes |
A11 27 |
Wu BY, Ou-Yang MC, Liu CT, Huang HC, Hu WL, Chen Illinois et al./2023 |
China |
To research the analgesic effect of LLLT during heel pricking compared to breast milk in healthy term neonates. |
Prospective, single-center, open-label, randomized, controlled study |
Hospital Nursery |
Neonates |
Kaohsiung Chang Gung Memorial Hospital |
Source: Prepared by the authors.
Table 3 presents the aspects of the included studies according to identification, type of PBM used, laser spot energy, laser wavelength, site where the laser was applied, and PBM outcome.
Table 3 Presentation of the studies included in the review. Maringá, Paraná, Brazil, 2024
ID |
Type of |
Spot |
Wavelength |
Application |
Outcome |
|---|---|---|---|---|---|
A1 17 |
Diode laser |
- |
- |
Ocular retina |
PBM showed long-term benefits, preserving distance and near vision in eyes with threshold retinopathy of prematurity. |
A2 18 |
GaAlAs laser |
100 mW |
830 nm |
Oral mucosa |
Low-intensity laser therapy can reduce the duration of chemotherapy-induced oral mucositis. |
A3 19 |
Diode laser |
21 mW |
685 nm |
Surgical incision |
There was a significant decline in surgical wound dehiscence in neonates undergoing PBM. |
A4 20 |
Diode laser |
40 mW |
780 nm |
Soft palate of the maxilla |
The laser accelerated the bone regeneration process, improving tissue regeneration of the midpalatal suture opening. |
A5 21 |
Diode laser |
150 mW |
830 nm |
Oral mucosa |
The diode laser reduces the severity and duration of oral mucositis, significantly alleviating the pain symptom. |
A6 22 |
Diode laser |
100 mW |
660 nm |
Mesial interproximal space of molars |
Pain reduction was significant on the first day, demonstrating the effectiveness of immediate symptom relief. |
A7 23 |
Diode laser |
300 mW |
810 nm |
Acupuncture points PC 6 (located on the underside of the wrist) |
Laser therapy has proven to be a useful technique in controlling the gag reflex, enabling children to tolerate the maxillary radiography procedure. |
A8 24 |
Diode laser |
100 mW |
808 nm |
Parotid glands bilaterally |
PBM stimulated increased salivary production, as well as the source needed for increased protein energy. |
A9 25 |
Diode laser |
100 mW |
645 nm |
Oral mucosa |
The laser significantly reduced wound size and pain compared to the placebo group. |
A10 26 |
Red and infrared laser |
100 mW |
660 nm or 808 nm |
Sublingual glands |
PBM increased salivary flow, alleviating xerostomia and improving chewing and swallowing. |
A11 27 |
Red and infrared laser |
150 mW |
810 nm |
Yintang Acupoint (EX-HN3) (midpoint between the medial ends of the eyebrows) |
The group in which PBM was applied had a shorter crying interval, associated with a shorter period of pain during heel pricking. |
Source: Prepared by the authors.
Discussion
In the studies included in the summary table, there are indications that the use of PBM may have therapeutic effects in reducing pain in invasive and surgical treatments 22,27, in enhancing tissue repair 20,28, and improving and regenerating wounds 19,22,27, as well as its application as a non-pharmacological treatment that can help manage recurrent aphthous stomatitis and oral mucositis in pediatric cancer patients 18,21,25, in preserving vision in children with retinopathy of prematurity 17, in the energy-protein effect of laser therapy in malnourished children, and in inhibiting the gag reflex through laser acupuncture 23,24.
Experimental studies were the most recurrent in this study, highlighting the researchers' interest in proving the effectiveness of therapeutic interventions associated with the use of PBM in pediatric patients. The results suggest that this non-pharmacological technique has shown promise, with satisfactory effects in certain contexts, although further studies are still needed for its validation 29-31.
In line with this finding, it is noted that, among the health sciences, dentistry was the field that invested the most in PBM research, while no studies were identified in the field of nursing. It should be noted, however, that nursing has been known to use PBM in wound treatment, analgesia, increased microcirculation, and acceleration of the tissue repair process, among other recently explored applications 32.
It is believed that PBM is an innovative practice in nursing 32, unlike dentistry, which has been using it for some years in clinical procedures 31. Therefore, it is necessary to produce further robust evidence to support current knowledge on the theme to avoid gaps and expand the dissemination of the technique in all fields of healthcare 33.
Pain is an important factor that can compromise a child's well-being, since, in more severe cases, it interferes with patients' eating, hydration, movement, and speech 34. Pain relief has been one of the focuses of pediatric treatment, as it contributes to reducing anxiety and fear. In this context, PBM, as a non-pharmacological method, has been explored for its potential to improve children's ability to cope with painful experiences, although the evidence is still preliminary 34.
Therefore, the analgesic effect of PBM is related to the increased release of serotonin, ß-endorphin, and enkephalins (natural endogenous opioid neuropeptides), acting on the release of substance P (neuropeptide) and the secretions of histamine, bradykinin, and prostaglandin E2, leading to inhibition of pain afferent fibers 11 and reversibly altering membrane permeability. Thus, therapeutically applied photons activate cell proliferation and reduce the activity of delta C and A fibers 35,36.
In addition, PBM modifies nerve conduction and excitation in peripheral neurons due to its action on the Na+/K+ pump channel, reducing noxious stimuli through its effects on the transient receptor potential cation channel subfamily V member 1 (TRPV1) and nerve growth factor (NGF), consequently decreasing their expressions (blocking inflammatory thermal hyperalgesia [37]). A study conducted in India identified that PBM is an effective way to better manage procedures that some patients find painful, without the need for prescription medications, which often have various side effects 38.
Light can have positive or negative effects on living cells and tissues, depending on wavelength, coherence, and dose or intensity 39. The wavelength (energy range) between 600 and 700 nm, in the red light spectrum, has been shown to be effective in inducing cell proliferation and differentiation, as it promotes greater biostimulation 40.
The prevalence of studies with children can be justified by the fact that they find it easier to communicate and express their pain, allowing the use of visual, audible, and tactile methods that lead them to understand the procedure performed and the importance of the proposed treatment, leading to greater closeness with the professional and contributing to greater adherence to their treatment 41. This reality is not perceived in neonates due to their inability to verbalize pain. In these cases, the painful sensation can be perceived through facial expressions, crying, and changes in physiological parameters 42.
PBM has beneficial effects on tissue regeneration and wound healing 10,11,43,44, matrix deposition, and cell layer regeneration 39,43. PBM has an anti-inflammatory effect on oral mucosal cells. Its mechanism of action occurs at the mitochondrial cellular level, related to the absorption of light by cytochrome C oxidase for cellular metabolism. Thus, it stimulates oxidative phosphorylation in mitochondria, reducing pain and accelerating wound healing. This increases adenosine triphosphate synthesis, produces inflammatory responses, and exhibits beneficial effects on inflammation and wound healing 9.
In addition, PBM controls secondary infections, as different wavelengths (energy ranges) induce different bacteria. Thus, at 830 nm, it controls infections at different stages since visible light reduces bacteria in infected wounds. However, it is necessary to check the type of bacterial infection before starting local irradiation 45.
A study conducted in Italy with pediatric patients found that PBM laser irradiation was effective in accelerating lesion resolution and increasing wound healing rates 34. In addition, it is considered a non-invasive and painless treatment, with high acceptance rates among pediatric patients. Given the positive results achieved, it is a viable therapy for the prevention and treatment of oral mucositis 46,47.
The prevalence of diode laser application is due to its widespread use in orthodontics, as this type of laser has been widely used in dental practice. The diode laser is easier to handle, has an anti-inflammatory effect, accelerates healing, intensifies neovascularization, causes less temperature elevation in target tissues, and, when used adequately, according to manufacturing protocols, does not cause harmful effects 4,48.
Treatment for oral mucositis is mainly palliative, using analgesics and anti-inflammatory medications, specific agents for the mucosa, and mouthwashes 49. The photochemical effect of the laser causes the damaged tissue to absorb the laser radiation and transform it into energy, preventing the progression of the wound in a preventive manner and avoiding the development of ulcers in the oral cavity. As oral mucositis arises, laser therapy will act in a curative manner, allowing therapeutic action on painful symptoms and accelerating the healing of this condition. Thus, it can be used as a complement to other treatment methods 12.
Another possible use for lasers is in the treatment of hyposalivation, which can impact children's daily lives, due to discomfort and pain, and potentially lead to oral health problems. In this context, the use of PBM in pediatric patients with hyposalivation has shown an increase in the quality of saliva flow, as well as improved chewing and swallowing 26.
Stimulation using LLLT can prevent gagging and reduce the gag reflex in pediatric patients undergoing intraoral radiography of the maxilla. Therefore, dentists should consider managing the gag reflex based on the type of treatment, the severity of the gagging, and the patient's age 50. In addition, stimulation through PBM can significantly reduce the incidence of postoperative vomiting in children undergoing strabismus surgery 23,50.
Study limitations
The methodological heterogeneity of the studies analyzed, both in terms of design and conduct of interventions, hindered a standardized analysis of the applicability and safety of PBM. This limitation compromises the generalization of results and hinders more robust conclusions regarding the technique's efficacy. In view of this, there is a need for efforts by the scientific community to develop study protocols that define specific parameters - such as wavelength, energy dose, application sites, and type of laser used -to ensure the reproducibility of studies and to obtain consistent and comparable results.
Conclusions
This scoping review mapped the available evidence on the use of PBM in neonatal and child healthcare. The studies found indicate that PBM has been used as a promising, safe, and easily applicable non-pharmacological method, with varying degrees of evidence and a range of protocols. This reinforces the need for training and adequate handling by healthcare professionals across the board, regardless of their field of expertise.
In addition, it contributes to the practice of healthcare professionals by providing resources on the use of PBM in neonatal and child health, highlighting its social and clinical relevance. However, due to the heterogeneity and limitations of the studies, it is not possible to conclusively state its clinical effectiveness.
Considered an easily applicable, painless, and non-invasive method, PBM tends to occupy an increasingly prominent place as a complementary therapy in the healthcare network for pain management, injury prevention, and tissue repair.
Given the relevance of this therapy, further primary studies are recommended, using distinct and rigorous methodologies, focused on the neonatal and pediatric population, especially in the field of nursing, to expand and consolidate knowledge on the use of PBM in varying clinical contexts, both in hospital and non-hospital settings.
Acknowledgements
We would like to thank the teaching staff of the Nursing Department at the Universidade Estadual de Maringá, the collaborators in this research, as well as the National Council for Scientific and Technological Development and the Fundação Araucária.
Conflict of interest: There are no conflicts of interest.
References
1. Hanna R, Dalvi S, Bensadoun RJ, Benedicenti S. Role of Photobiomodulation Therapy in Modulating Oxidative Stress in Temporomandibular Disorders. A Systematic Review and Meta- Analysis of Human Randomised Controlled Trials. Antioxidants. 2021;10(7):1028. DOI: https://doi.org/10.3390/antiox10071028
2. Couto GF, Chaves CT de OP, Nunez SC, Frade-Barros AF. O uso da fotobiomodulacao (FBM) na melhora da hidratacao cutánea na dermatite atopica leve ou moderada. Revista Novos Desafios. 2023;3(1):78-85. Disponivel em: http://novosdesafios.inf.br/index.php/revista/article/view/66
3. Silva T, Tobelem D da C, Malavazzi TC dos S, de Mendonca JFB, Andreo L, Chavantes MC et al. Effect of Photobiomodulation Combined with Physiotherapy on Functional Performance in Children with Myelomeningocele: Randomized, Blind Clinical Trial. Journal of Clinical Medicine. 2023;12(8):2920. DOI: https://doi.org/10.3390/jcm12082920
4. Costa CN. Uso do laser de baixa potencia para o tratamento de parestesia: uma revisao de literatura. 2023. Disponivel em: https://repositorio.bahiana.edu.br:8443/jspui/handle/bahiana/7513
5. Da Silva ELMS. Uso da fotobiomodulacao associada a camomila (Matricaria recutita L.) no tratamento da mucosite oral em criancas e adolescentes sob tratamento antineoplasico: um ensaio clinico randomizado [tese]. Recife: Universidade Federal de Pernambuco; 2022. Disponivel em: https://repositorio.ufpe.br/handle/123456789/44641
6. Hanna R, Dalvi S, Benedicenti S, Amaroli A, Saălaăgean T, Pop ID et al. Photobiomodulation Therapy in Oral Mucositis and Potentially Malignant Oral Lesions: A Therapy Towards the Future. Cancers. 2020;12(7):1949. DOI: https://doi.org/10.3390/cancers12071949
7. Farivar S, Malekshhabi T, Shiari R. Biological effects of low-level laser therapy. J Lasers Med Sci. 2014;5(2):58-62. Disponivel em: https://pubmed.ncbi.nlm.nih.gov/25653800/
8. Heiskanen V, Hamblin MR. Photobiomodulation: Lasers vs. Light emitting diodes?. Photochemical & Photobiological Sciences. 2018;17(8):1003-17. DOI: https://doi.org/10.1039/c8pp00176f
9. Silva T, de Queiroz JR, Turcio KHL, Tobelem D da C, Araujo TR, Coutinho KSL et al. Effect of Photobiomodulation Combined with Physical Therapy on Functional Performance in Children with Myelomeningocele: A Protocol Randomized Clinical Blind Study. PLOS One. 2021;16(10):e0253963. DOI: https://doi.org/10.1371/journal.pone.0253963
10. Borba CR, Silva DM, Rodrigues NH, Souza E, Silva LGA, Besckow AE. Laser Therapy in Pressure Injuries in Pediatric Patients: An Experience Report. Journal of Nursing and Health. 2021;11(4):e2111421034. DOI: https://doi.org/10.15210/jonah.v11i4.21034
11. Silva YME. Estudo da terapia por fotobiomodulacao associada ao diazepam no controle da alodinia e na modulacao de receptores de dor em modelo experimental de tendinite [tese]. Sao Paulo: Universidade Nove de Julho; 2021. Disponivel em: http://bibliotecatede.uninove.br/handle/tede/2676
12. Spezzia S. Mucosite oral em pacientes cancerosos submetidos a tratamento quimioterapico. Revista Ciencias e Odontologia. 2020;4(1):36-40. Disponivel em: https://revistas.icesp.br/index.php/RCO/article/view/887
13. Наседкин АН, Москвин СВ. Оптимизация параметров лазерной терапии при заболеваниях глоточной миндалины у детей. Вопросы курортологии, физиотерапии и лечебной физической культуры. 2022;99(4):29-35. DOI: https://doi.org/10.17116/kurort20229904129
14. Montemor AR, Ramos RR. Laser de baixa intensidade em cirurgia bucomaxilofacial. Revista Ibero-Americana de Humanidades, Ciencias e Educacao. 2022;8(5):1845-64. DOI: https://doi.org/10.51891/rease.v8i5.5594
15. Aromataris E, Lockwood C, Porritt K, Pilla B, Jordan Z. JBI Manual for Evidence Synthesis. JBI. 2024. DOI: https://doi.org/10.46658/JBIMES-24-01
16. Tricco AC, Lillie E, Zarin W, O’Brien KK, Colquhoun H, Levac D et al. PRISMA Extension for Scoping Reviews (PRISMA-ScR): Checklist and Explanation. Ann Intern Med. 2018;169(7):467-73. DOI: https://doi.org/10.7326/M18-0850
17. Mcloone E. Long Term Functional and Structural Outcomes of Laser Therapy for Retinopathy of Prematurity. Br J Ophthalmol. 2006;90(6):754-9. DOI: https://doi.org/10.1136/bjo.2005.068304
18. Kuhn A, Porto FA, Miraglia P, Brunetto AL. Low-Level Infrered Laser Therapy in Chemotherapy Induced Oral Mucositis: A Randomized Placebo Controlled Trial in Children. J Pediatr Hematol Oncol. 2009;31(1):33-7. DOI: https://doi.org/10.1097/MPH.0b013e318192cb8e
19. Pinto FC, Chavantes MC, Pinto NC, Alho EJ, Yoshimura EM, Matushita H et al. Novel Treatment Immediatly after Myelomeningocele Repair Applying Low Level Laser Therapy in Newborns: A Pilot Study. Pediatr Neurosurg. 2011;46(4):249-54. DOI: https://doi.org/10.1159/000319363
20. Cepera F, Torres FC, Scavani MA, Paranhos LR, Capelloza Filho L, Cardoso MA et al. Effect of a Low-Level Laser on Bone Regeneration Rapid Maxillary Expansion. Am J Orthod Dentofacial Orthop. 2012;141(4):444-50. DOI: https://doi.org/10.1016/j.ajodo.2011.10.023
21. Cauwels RG, Martens LC. Low level Laser Therapy in Oral Mucositis: A Pilot Study. Eur Arch Paediatr Dent. 2011;12(2):118-23. DOI: https://doi.org/10.1007/BF03262791
22. Stein S, Korbmacher-Steiner H, Popovic N, Braun A. Pain Reduced by Low Level Laser Therapy during Use of Orthodontic Separators in Early Mixed Dentition. J Orofac Orthop. 2015;76(5):431-9. DOI: https://doi.org/10.1007/s00056-015-0306-4
23. Elbay M, Tak O, Şermet Elbay U, Kaya C, Eryılmaz K. The Use of Low Level Laser Therapy for Controlling the Gag Reflex in Children during Intraoral Radiography. Lasers Med Sci. 2016;31(2):355-61. DOI: https://doi.org/10.1007/s10103-016-1869-z
24. Vieira KA, Bastos CM, Vitor MGC, Deana AM, Fernandes KP, Rodrigues MF et al. Use of Low Level Laser Therapy on Children Aged 1 to 5 Years with Energy Protein Malnutrition: A Clinical Trial. Medicine. 2018;97(17):e0538. DOI: https://doi.org/10.1097/MD.0000000000010538
25. Bardellini E, Veneri F, Amadori F, Conti G, Majorana A. Photobiomodulation Therapy for the Management of Recurrent Aphthous Stomatitis in Children: Clinical Effective and Parental Satisfaction. Med Oral Patol Oral Cir Bucal. 2020;25(4):549. DOI: https://doi.org/10.4317/medoral.23573
26. Oliveira AB, Ferrisse TM, Salomao KB, Miranda LM, Bufalino A, Brighenti FL. Fotobiomodulacao no tratamento da xerostomía associada a hipossalivacao em paciente pediatrico com esclerodermia sistemica. Autopsy and Case Reports. 2021;11:e2020220. DOI: https://doi.org/10.4322/acr.2020.220
27. Wu BY, Ou-Yang MC, Liu CT, Huang HC, Hu WL, Chen IL et al. Analgesic Effect of Low-Level Laser Therapy before Heel Lance for Pain Management in Healthy Term Neonates: A Randomized Controlled Trial. Children. 2023;10(12):1901. DOI: https://doi.org/10.3390/children10121901
28. Oliveira AB, Ferrisse TM, Salomao KB, Miranda ML, Bufalino A, Brighenti FL. Photobiomodulation in the Treatment of Xerostomia Associated with Hyposalivation in a Pediatric Patient with Systemic Scleroderma. Autopsy and Case Reports. 2020;11:e2020220. DOI: https://doi.org/10.4322/acr.2020.220
29. Ferreira M, Bezinelli L, Eduardo F, Castro F, Gobbi M, Lopes R et al. Efeito da fotobiomodulacao nas alteracoes do paladar em pacientes sob transplante de celulas hematopoieticas: estudo clinico randomizado. Hematol Transfus Cell Ther. 2023;45:904-5. DOI: https://doi.org/10.1016/j.htct.2023.09.1627
30. Carvalho MB dos S, Blascovich HB, Moreira TG de P. Fotobiomodulacao com duplo comprimento de onda na prevencao de mucosite oral em criancas e adolescentes com cancer. Rev Enferm Atual In Derme. 2024;98(1):02425. DOI: https://doi.org/10.31011/reaid-2024-v.98-n.1-art.1992
31. Braga KNF, Oliveira AC. O uso da fotobiomodulacao no tratamento da mucosite oral em pacientes pediatricos oncologicos: revisao de literatura. 2023. Disponivel em: https://repositorio.unifametro.edu.br/handle/123456789/1971
32. Caires JM, Oliveira JC, Simonetti SH, Leal MR, Felix MC, Sampaio VM, Marreira M. Terapia a laser de baixa intensidade aplicada pelo enfermeiro: Qual o seu cenario de atuacao e uniformidade de parametros terapeuticos?. Research, Society and Development. 2023;12(13):88121344139. DOI: https://doi.org/10.33448/rsd-v12i13.44139
33. Tonazio CH, Girondi JB, Silva RD, Frison SS. Fotobiomodulacao no Tratamento de Feridas: Evidencias para a Atuacao do Enfermeiro. Rio de Janeiro: Thieme Revinter; 2024.
34. Hanna R, Miron IC, Benedicenti S. A Novel Therapeutic Approach of 980 nm Photobiomodulation Delivered with Flattop Beam Profile in Management of Recurrent Aphthous Stomatitis in Paediatrics and Adolescents: A Case Series with 3-Month Follow-Up. Journal of Clinical Medicine. 2024;13(7):2007. DOI: https://doi.org/10.3390/jcm13072007
35. Chung H, Dai T, Sharma SK, Huang YY, Carroll JD, Hamblin MR. The Nuts and Bolts of Low-level Laser (Light) Therapy. Ann Biomed Eng. 2011;40:516-33. DOI: https://doi.org/10.1007/s10439-011-0454-7
36. Hanna R, Dalvi S, Bensadoun RJ, Raber-Durlacher JE, Benedicenti S. Role of Photobiomodulation Therapy in Neurological Primary Burning Mouth Syndrome. A Systematic Review and Meta-Analysis of Human Randomised Controlled Clinical Trials. Pharmaceutics. 2021;13(11):1838. DOI: https://doi.org/10.3390/pharmaceutics13111838
37. Hanna R, Bensadoun RJ, Beken SV, Burton P, Carroll J, Benedicenti S. Outpatient Oral Neuropathic Pain Management with Photobiomodulation Therapy: A Prospective Analgesic Pharmacotherapy Paralleled Feasibility Trial. Antioxidants. 2022;11(3):533. DOI: https://doi.org/10.3390/antiox11030533
38. Khan BS, Setty JV, Srinivasan I, Kibriya S, Anu S, Radhakrishna S, Milit Y. Low-level Laser Therapy to Alleviate Pain of Local Anesthesia Injection in Children: A Randomized Control Trial. International Journal of Clinical Pediatric Dentistry. 2023;16(S3):283. DOI: https://doi.org/10.5005/jp-journals-10005-2699
39. Ebrahiminaseri A, Sadeghizadeh M, Moshaii A, Asgaritarghi G, Safari Z. Combination Treatment of Dendrosomal Nanocurcumin and Low Level Laser Therapy Develops Proliferation and Migration of Mouse Embryionic Fibroblasts and Alter TGF-β, VEGF, TNF-α and IL-6 Expression Involved in Wound Healing Process. PLOS One. 2021;16(5):e0247098. DOI: https://doi.org/10.1371/journal.pone.0247098
40. Wilden L, Karthein R. Import of Radiation Phenomena of Electrons and Therapeutic Low Level Laser in Regard to the Mitochondrial Energy Transfer. J Clin Laser Med Surg. 1998;16(3):159-65. DOI: https://doi.org/10.1089/clm.1998.16.159
41. Nova PV, Parente AT, Fonseca AF, Silva GG, Paranhos SB, de Castro NJC et al. Brinquedo terapeutico e o brincar: a compreensao a partir do academico de enfermagem. Revista Eletronica Acervo Saude. 2023;23(3):e12201. DOI: https://doi.org/10.25248/reas.e12201.2023
42. Sousa DN, Bonfim KC, Olivindo DD. Assistencia de enfermagem ao recem-nascido prematuro na unidade de terapia intensiva neonatal: revisao integrativa. Research, Society and Development. 2022;11(7):e46911730351. DOI: https://doi.org/10.33448/rsd-v11i7.30351
43. Mello DC. Terapia por fotobiomodulacao modula a organizacao tecidual e manutencao das propriedades mecanicas em modelo experimental de lesao cutanea [tese]. Sao Paulo: Universidade Nove de Julho; 2021. Disponivel em: http://bibliotecatede.uninove.br/handle/tede/2879
44. Becheleni MT, Ferreira AF, Nascimento LD, Muniz SK, Pinto TD, de Oliveira FL et al. Influencia da terapia de fotobiomodulacao na cicatrizacao tecidual e prevencao de complicacoes decorrentes de exodontia: uma revisao de literatura. Revista CPAQV-Centro de Pesquisas Avancadas em Qualidade de Vida. 2024;16(1):12. DOI: https://doi.org/10.36692/V16N1-112R
45. Evans DH, Abrahamse H. Efficacy of Three Different Wavelengths for in Vitro Wound Healing. Photodermatol Photoimmunol Photomed. 2008;24(4):199-210. DOI: https://doi.org/10.1111/j.1600-0781.2008.00362.x
46. Elad S, Cheng KKF, Lalla RV, Yarom N, Hong C, Logan RM et al. MASCC/ISOO Clinical PRactice Guidelines for the Management of Mucositis Secondary to Cancer Therapy. Cancer. 2020;126(19):4423-31. DOI: https://doi.org/10.1002/cncr.33100
47. Elad S, Cheng KKF, Lalla RV, Yarom N, Hong C, Logan RM et al. Mucositis Guidelines Leadership Group of the Multinational Association of Supportive Care in Cancer and International Society of Oral Oncology (MASCC/ISOO). MASCC/ISOO clinical practice guidelines for the management of mucositis secondary to cancer therapy. Erratum in: Cancer. 2021;127(19):3700. DOI: https://doi.org/10.1002/cncr.33549
48. Dias BRL. Utilizacao de laser diodo na regressao de lesoes apicais [dissertacao]. Porto: Universidade Fernando Pessoa; 2023. Disponivel em: https://bdigital.ufp.pt/entities/publication/a9d57cb6-feee-418d-b569-a96cfd0eff9b
49. Andrade J de M, Davatz GC. Protocolos de laserterapia para a prevencao e tratamento da mucosite oral induzida por radioterapia ou quimioterapia. Revista Feridas. 2022;52:1877-85. DOI: https://doi.org/10.36489/feridas.2022v10i52p1877-1885
50. Mehdizadeh M, Mohammadbeigi A, Sharifinejad A. An Overview about New Methods in Management of Gag Reflex during Dental Treatment: a Systematic Review. J Dentistry. 2023;24(4):372. DOI: https://doi.org/10.30476/dentjods.2022.96360.1934