

|
ARTICLE
Jhon Henry Osorio Castaño 1
Wilson Cañón Montañez 2
Oscar Augusto Bedoya Carvajal 3
John Camilo García Uribe 4
Aníbal Vicente Arteaga Noriega 5
1 Universidad de Antioquia, Colombia
![]() 0000-0001-6272-722X
0000-0001-6272-722X
![]() jhenry.osono@udea.edu.co
jhenry.osono@udea.edu.co
2 Universidad de Antioquia, Colombia
![]() 0000-0003-0729-5342
0000-0003-0729-5342
![]() wilson.canon@udeaedu.co
wilson.canon@udeaedu.co
3 Universidad de Antioquia, Colombia
![]() 0000-0001-6343-8702
0000-0001-6343-8702
![]() oscar.bedoyac@udea.edu.co
oscar.bedoyac@udea.edu.co
4 Corporación Universitaria Remington, Colombia
![]() 0000-0002-3810-5583
0000-0002-3810-5583
![]() john.garcia@uniremington.edu.co
john.garcia@uniremington.edu.co
5 Corporación Universitaria Remington, Colombia
![]() 0000-0002-6612-1169
0000-0002-6612-1169
![]() anibal.arteaga@uniremington.edu.co
anibal.arteaga@uniremington.edu.co
Theme: Health promotion, well-being, and quality of life
Contribution to the field: To highlight the current status of sleep quality in nursing students worldwide, considering that sleep is a functional pattern, a necessity, and a core aspect of health and quality of life for nurses who, in the future, will provide care for the sleep of other humans in different settings, to restore their health and well-being and contribute to the healing and cure of problems and disorders in their vital functioning.
Received: 13/11/2024
Sent to peers: 18/02/2025
Approved by peers: 26/05/2025
Accepted: 03/06/2025
Para citar este artículo / To reference this article / Para citar este artigo Osorio Castaño JH, Cañón Montañez W, Bedoya Carvajal OA, García Uribe JC, Arteaga Noriega AV. Sleep Quality in Nursing Students: Systematic Review and Meta-Analysis of Prevalence Studies. 2025;25(4):e2542. DOI: https://doi.org/10.5294/aqui.2025.25.4.2
Introduction: Since there are no comprehensive studies, it is important to consolidate data on sleep quality in nursing students.
Objective: To estimate the prevalence of poor sleep quality in nursing students worldwide.
Materials and Methods: This is a systematic review and meta-analysis registered on the PROSPERO platform, in which primary studies were searched for in LILACS, PubMed, Science Direct, Scopus, EMBASE, and SAGE in English, Portuguese, and Spanish until May 2024, which had measured the prevalence of sleep quality and had used a scale for that purpose. The Joanna Briggs Institute's (JBI) methodological guidelines for systematic reviews of observational studies were considered. Quality assessment was performed using the institute's tool for prevalence studies. A meta-analysis was also done using a random-effects model, and the weighted mean prevalence, the heterogeneity, and publication bias were calculated using the I2 statistic and Egger's test, respectively.
Results: A total of 25 studies were included in the meta-analysis, representing 5,559 nursing students. A low sleep quality prevalence of 65 % (95 % CI .55-.74) was identified, with Latin America being the region with the highest prevalence, 84 % (95 % CI .65-.97), and Europe the lowest, 38 % (95 % CI .23-.54).
Conclusion: In most world regions, with a higher prevalence in Latin America, the quality of sleep in nursing students is very low. For this reason, its consequences and effects in the short, medium, and long term must begin to be studied and measured systematically in university training institutions.
Keywords (Source: DeCS): Nursing students; sleep quality; prevalence; meta-analysis; world Population
Resumen
Introducción: Debido a que no existen estudios integradores, es relevante consolidar datos sobre la calidad del sueño en estudiantes de enfermería.
Objetivo: Estimar la prevalencia de la baja calidad del sueño en estudiantes de enfermería a nivel mundial.
Materiales y métodos: Revisión sistemática y metaanálisis registrado en la plataforma PROSPERO, en la que se buscaron estudios primarios en LILACS, Pubmed, Science Direct, Scopus, EMBASE y SAGE en idiomas inglés, portugués y español hasta mayo de 2024, que hubiesen medido la prevalencia de la calidad del sueño y que hubiesen utilizado una escala para tal propósito. Se tuvo cuenta la guía metodológica para revisiones sistemáticas de estudios observacionales del Instituto Joanna Briggs. Se realizó la evaluación de la calidad con la herramienta de dicho instituto para estudios de prevalencia. Asimismo, se hizo un metaanálisis bajo un modelo de efectos aleatorios, se calculó el promedio ponderado de la prevalencia, la heterogeneidad a través del estadístico I2 y el sesgo de publicación con la prueba de Egger.
Resultados: Se incluyeron 25 estudios en el metaanálisis, que representan a 5559 estudiantes de enfermería. Se identificó una prevalencia de baja calidad del sueño de 65 % (IC95 % ,55-,74), siendo Latinoamérica la región que presenta la prevalencia más alta, 84 % (IC95 % ,65-,97) y Europa la más baja, 38 % (IC95% ,23-,54).
Conclusión: En la mayoría de las regiones del mundo, con una mayor prevalencia en Latinoamérica, la calidad del sueño en estudiantes de enfermería es muy baja; por esta razón, sus consecuencias y efectos a corto, mediano y largo plazo deben empezar a ser estudiadas y medidas sistemáticamente en las instituciones de formación universitaria.
Palabras clave (Fuente DeCS): Estudiantes de enfermería; calidad del sueño; prevalencia; metaanálisis; población mundial
Resumo
Introdução: Diante da ausência de estudos integrativos, torna-se relevante consolidar dados sobre a qualidade do sono em estudantes de enfermagem.
Objetivo: Estimar a prevalência de baixa qualidade do sono em estudantes de enfermagem em âmbito mundial.
Materiais e métodos: Revisão sistemática e metanálise registrada na plataforma PROSPERO, com busca de estudos primários nas bases de dados LILACS, PubMed, Science Direct, Scopus, EMBASE e SAGE, em espanhol, inglês e português, até maio de 2024. Foram incluídos estudos que mensuraram a prevalência da qualidade do sono e que utilizaram uma escala para esse fim. A revisão seguiu as diretrizes metodológicas para estudos observacionais do Instituto Joanna Briggs. A avaliação da qualidade foi realizada com o instrumento desse instituto específico para estudos de prevalência. Além disso, foi realizada uma metanálise com modelo de efeitos aleatórios, calculando-se a média ponderada da prevalência, a heterogeneidade pelo I2 e o viés de publicação pelo teste de Egger.
Resultados: Foram incluídos 25 estudos, o que representa 5559 estudantes de enfermagem. Identificou-se uma prevalência de baixa qualidade do sono de 65 % (IC 95 % = 0,55-0,74), sendo a América Latina a região com a maior prevalência, 84 % (IC 95 % = 0,65-0,97) e a Europa a menor, 38 % (IC 95 % = 0,23-0,54).
Conclusão: Na maioria das regiões do mundo, com destaque para a América Latina, a qualidade do sono em estudantes de enfermagem é muito baixa Seus efeitos em curto, médio e longo prazo devem ser sistematicamente estudados pelas instituições de ensino superior.
Palavras-chave (Fonte DeCS): Estudantes de enfermagem; qualidade do sono; prevalência; metanálise; população mundial
Sleep and rest constitute one of the functional patterns defined by Marjory Gordon in her eleven functional patterns, and it is one of the basic human needs that must be satisfied, as it is essential for survival 1. Its main function is physical and mental restoration 2. Sleep is a complex phenomenon resulting from the interaction between the neuroendocrine system, the biological clock, and biochemical processes with environmental, social, and cultural aspects that are relevant to people's lives 3. Sleep has a vital role in maintaining the balance of human psychosocial behavior 4. It is controlled by the circadian rhythm over a 24-hour period in a light-dark cycle 5 and is conditioned by factors such as physiological function, related to stimulation in the suprachiasmatic nucleus of the hypothalamus, and exogenous factors such as work schedules and other daily activities 4-5.
Sleep is important for maintaining and promoting good health. Sleep patterns and problems change throughout life 6. Sleep disorders comprise a group of conditions that are becoming increasingly common, and their social implications are considered a public health problem 3. Sleep disorders result in psychosocial stress, psychiatric disorders, decreased work effectiveness, and learning problems 4. Similarly, sleep disorders have been associated with morbidity and mortality in general 7. Therefore, good nighttime sleep is crucial for mental and physical well-being 8.
One of the social groups that frequently experiences sleep problems is that of university students 1. After university admission, students' routines become different from what they were in high school 5. Entering the academic world of university is a milestone in a person's life, which includes a set of rules, procedures, groups, and people that are completely unfamiliar, interaction with other students, professors, and employees of the institution, as well as tests and evaluations 9. The interactions established between students and the conditions of study at university can compromise their mental and psychological health. These interactions can affect their autonomy regarding tasks, their degree of satisfaction in performing their work, their perspectives, and the establishment of human relationships 2. Therefore, poor sleep quality is often related to the deprivation of rest time for academic activities, in line with social and personal demands. Sleep habits and specific sleep behaviors influence students' academic success 3, and as a result, several students use central nervous system stimulants to stay awake 10.
Nursing is a profession that has special sleep needs as it consists of rotating shifts. In their professional work, nurses provide the care necessary for individuals to meet their basic needs 1, and it is considered a predominantly female profession, which is why special focus has been placed on mental health. Nursing students require special attention regarding sleep and rest patterns. Similarly, as they are mainly women, they encounter some unique stressors that affect their sleep, such as night shifts, the transition to university life, lifestyle changes, courses with heavy academic workloads, the use of study techniques, family life, and sometimes work, for those students who combine study with work, in addition to issues stemming from interpersonal relationships. All these factors can increase students' susceptibility to sleep pattern problems and mental health issues 11.
Nursing students often experience stress and sleep disturbances related to the effort required to meet their academic needs, which is why well-being is considered the optimal state of health required to successfully perform their various roles 12. Sleep disturbances such as insomnia are common among nursing students and are closely related to their academic performance 13. Nursing students have complicated schedules, with intense courses and varied clinical practice hours 14, and these exogenous factors, combined with endogenous factors such as other activities performed to induce or maintain sleep, become a challenge for them 3. The following have been reported as consequences of poor sleep quality: headache, exhaustion, back pain, symptoms of peptic disease, insomnia, and depression 4,11,15-16, poor academic performance 13, weight gain 6,17, drowsiness 2, and decreased well-being 12 and quality of life 18. During the COVID-19 pandemic, four health problems were identified in nursing students: depression, fear, anxiety, and stress. In addition, there was a prevalence of sleep pattern disturbances of up to 27 % 19.
The sleep quality in nursing students and the factors associated with it have been measured in several parts of the world, frequently using the Pittsburgh scale 20. Prevalence rates of sleep pattern disturbances ranging from 9 % to 95 % have been found in various studies, and it has been shown that high levels of stress are associated with symptoms of drowsiness and poor sleep quality 9,14,21, as well as with smoking cigarettes 22, dissatisfaction with academic performance 5,20,23, and low income 7. Similarly, study habits can determine sleep quality. It has been found that students prefer to study at night, which means losing hours of relaxation to complete academic tasks, and students in more advanced semesters show a higher prevalence of pattern disturbance 2-3. There is an additional associated phenomenon: procrastination; it has been identified that self-regulation of fatigue and problems with cell phone use are positively related to the level of procrastination in going to bed 8,24.
To date, the systematic reviews that exist to synthesize the evidence on sleep quality in students are those reported by Gardani et al. 25; these authors explored the symptoms of insomnia and stress in university students in general, while Seoane et al. 26 reviewed the relationship between academic performance and sleep disturbances in medical students. According to the literature search, no review has explored or evaluated the prevalence of sleep quality in nursing students; therefore, the objective of this research was to estimate the influence of poor sleep quality on nursing students worldwide.
Protocol and Registration
This systematic review and meta-analysis followed the methodological guidelines for reviews of observational studies reporting prevalence rates developed by the Joanna Briggs Institute (JBI) 27. The updated guidelines for the publication of systematic reviews from the 2020 PRISMA statement 28 were also considered. The protocol was registered in the International Prospective Register of Systematic Reviews (PROSPERO) with the code CRD 42024505553.
Study Eligibility Criteria
The inclusion criteria for the primary studies were:
Prevalence and/or cross-sectional analytical studies.
That had measured the prevalence of sleep quality at least once.
That had used a validated scale and/or instrument to measure sleep quality.
Which had been published within the last eight years.
Which had been published in English, Spanish, or Portuguese.
The population included in the primary studies had to be undergraduate nursing students of any age, race, and/or sociodemographic status who were actively enrolled in the program in any semester of education. The study condition for participants was sleep quality, measured at least once with an instrument and/or scale validated for this purpose. All students from any region or country worldwide were included.
Information Sources and Search Strategies
For the identification of studies, a search was conducted in the following databases: Latin American and Caribbean Health Sciences Literature (LILACS), MEDLINE (via PubMed), Science Direct, Scopus, Excerpta Medica Database (EMBASE), and SAGE using the Spanish terms: estudiante, enfermería, sueño, and calidad, and the English terms: student, nursing, sleep, and quality, published within the last eight years, from May 2016 to May 2024. The search equation with the terms and Boolean connectors was as follows in Spanish: ((estudiante:Ti/Ab) AND (enfermería:Ti/Ab)) AND (sueño:Ti/Ab) AND (calidad:Ti/Ab)), and in Enlgish: ((student:Ti/Ab) AND (nursing:-Ti/Ab)) AND (sleep:Ti/Ab) AND (quality:Ti/Ab)). The inclusion criteria defined prior to the search were applied. A database was constructed to record the searches. These were conducted by one researcher, and the studies were screened by two researchers, who considered the title and abstract. A subsequent review of the agreements was conducted, and for disagreements, a third researcher was consulted.
Evaluation of the Methodological Quality of the Studies
The methodological quality evaluation was performed using the tool developed by Munn et al. 29 from the JBI, recommended for systematic reviews of prevalence studies. A chart was developed to show the risk of bias for each article, based on the numerical value obtained in the rating, using the Robvis tool 30. This assessment was performed independently by two researchers, and in the event of disagreement, a third researcher was included to solve it. To define the cut-off points, the agreements obtained for the items evaluated positively by each article were considered, and it was decided that at least five or more agreements classified the study as high quality or low risk of bias. It was decided not to exclude any article, even if its rating was low quality.
Data Extraction
To extract the information, a database was developed that included the following variables: Study title, authors, year, study country, sample size, scales used, variables measured, and prevalence. The information was extracted independently by two researchers; it was entered into the database, and the process was cross-checked. In the event of inconsistencies, a third researcher was consulted to validate the information. The results were integrated narratively based on three main aspects: the characteristics of the studies, the reported prevalences, and the assessment of risk of bias.
Data Analysis
A meta-analysis was performed using a random effects model, as this model factors in variation between studies by assuming that the prevalence estimates for each study follow a normal distribution. The data were transformed using the double arcsine technique, a weighted mean prevalence was calculated with its respective 95 % confidence intervals (CI), and the corresponding chart (forest plot) was presented. In addition, heterogeneity was calculated using the inconsistency statistic (I2). A meta-analysis was also performed for the following regions of the world: Europe, Asia, Latin America, and North America, to identify the respective prevalences under the same conditions as the general meta-analysis. Data analysis was performed using the freely available MetaXL software 31. Publication bias due to missing data was assessed using a funnel plot and Egger's statistical test, with a p-value < 0.05 indicating statistically significant publication bias.
As this study used secondary information sources, in the form of scientific journal articles, it was not necessary to submit it to a Research Ethics Committee for approval. As researchers, we declare our ethical responsibility, framed within respect for authorship, by adequately referencing each manuscript cited in the text, thereby respecting copyright. Likewise, as indicated in this section, the review protocol was registered in PROSPERO to grant greater transparency and rigor to the study.
Figure 1 shows the flowchart of the results of the searches, screening, selection, and total number of articles included in the review. A total of 1,635 articles were identified in all databases. After removing duplicates and those in languages other than Spanish, English, and Portuguese, and screening by title and abstract, only 25 studies were included.
Figure 1 Study Screening and selection diagram
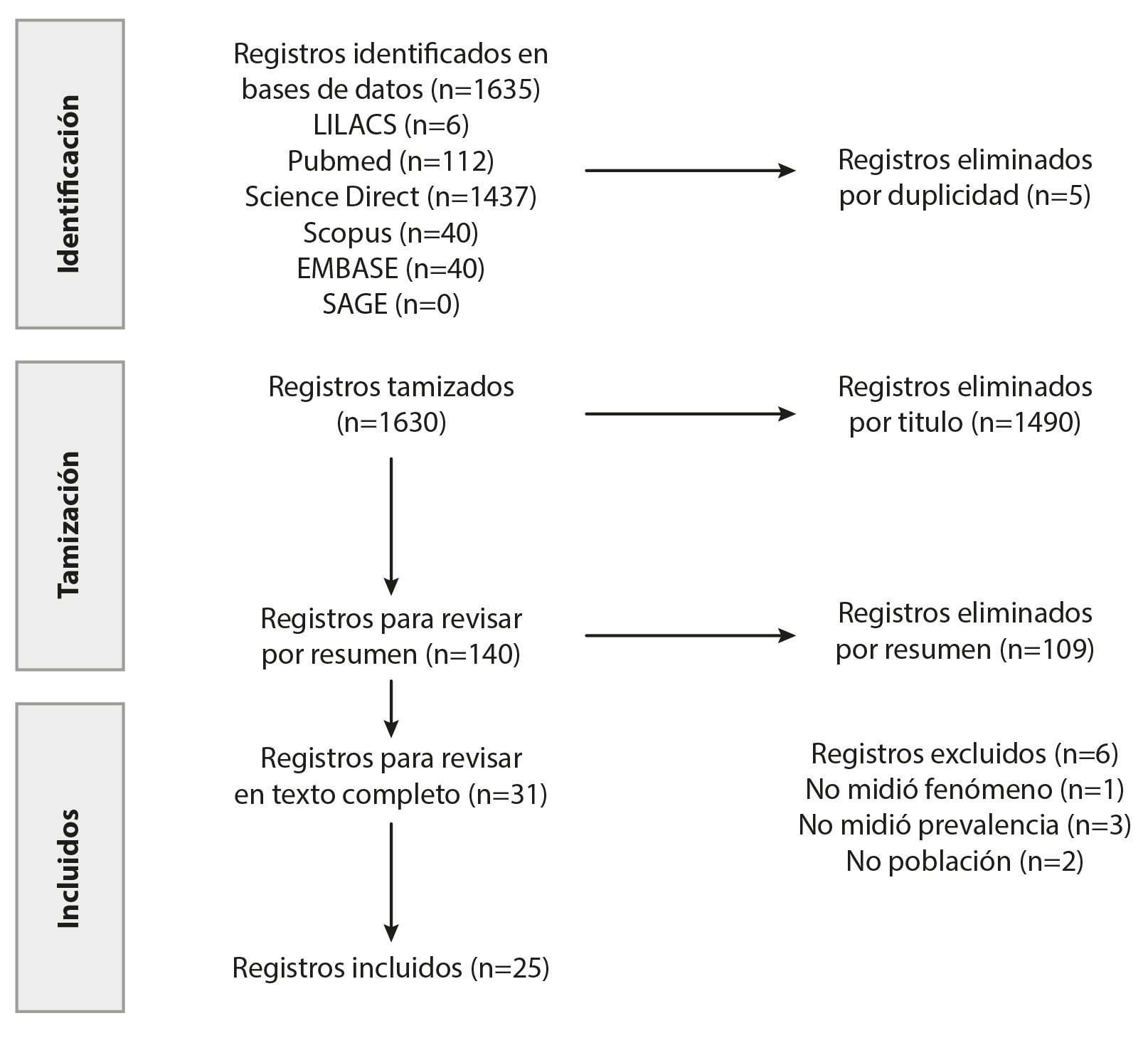
Source: Prepared by the authors.
Characteristics of the Studies Included
The studies were published between 2016 and 2023, with 2020 and 2023 seeing the highest number of articles (7 and 5, respectively). All studies had a cross-sectional analytical design. Six studies were conducted in Brazil 2,5,7,9,17,32, three in Italy 20,33-34 and the United States 11,14,35, two each in Turkey 21-22, Indonesia 13,36, and India 23,37, and one each in Chile 38, Mexico 39, South Korea 12, Spain 40, Iran 15, Morocco 41, and Portugal 42. When grouped by regions of the world, it was found that 32 % of the studies were conducted in Latin America, 28 % in Europe, 24 % in Asia, 12 % in North America, and the remaining studies in Africa.
A total of 5,559 nursing students participated in the 25 studies included. Table 1 shows the characteristics of studies. In relation to the academic year in which the students were enrolled, 17 articles included students from all semesters and three included students in theoretical training. The rest of the studies measured students in different years. Twenty-two studies used the Pittsburgh Sleep Quality Index and three applied the Sleep and Daytime Habits Questionnaire. Twenty-two studies applied other additional scales. The prevalence ranges for poor sleep quality ranged from 5.9 % to 100 %. By region, the following prevalence ranges were observed: Africa, 64 %; Asia, 40 % to 82 %; Europe, 6 % to 56 %; Latin America, 35 % to 100 %; and North America, 66 % to 73 %.
Table 1 Characteristics of the Studies Included
Authors |
Year |
Country |
Sample |
Time of measurement |
Sleep Quality |
Prevalence (%) |
|---|---|---|---|---|---|---|
Belingheri et al. |
2020 |
Italy |
202 |
Professional practice |
Sleep and Daytime |
9.4 |
Belingheri et al. |
2022 |
Italy |
202 |
Prior to professional |
Sleep and Daytime |
5.9 |
Dos Santos et al. |
2020 |
Brazil |
286 |
Theoretical training |
Pittsburgh Sleep Quality Index |
86.3 |
Dwi et al. |
2020 |
Indonesia |
492 |
Theoretical training |
Pittsburgh Sleep Quality Index |
70.5 |
Fernandes et al. |
2019 |
Brazil |
117 |
Theoretical training |
Pittsburgh Sleep Quality Index |
94.8 |
Fernández et al. |
2020 |
Spain |
334 |
The entire course |
Pittsburgh Sleep Quality Index |
45.5 |
Ghosh et al. |
2021 |
India |
91 |
1 and 2 years |
Pittsburgh Sleep Quality Index |
82.4 |
Gianfredi et al. |
2018 |
Italy |
117 |
The entire course |
Sleep and Daytime Habits Questionnaire |
30.7 |
Günef y Arslantaf |
2017 |
Turkey |
379 |
The entire course |
Pittsburgh Sleep Quality Index |
51.1 |
Higbee et al. |
2022 |
USA |
272 |
The entire course |
Pittsburgh Sleep Quality Index |
73.1 |
Lima et al. |
2020 |
Brazil |
159 |
The entire course |
Pittsburgh Sleep Quality Index |
99 |
Medeiros et al. |
2020 |
Brazil |
167 |
The entire course |
Pittsburgh Sleep Quality Index |
35.3 |
Nunes et al. |
2016 |
Brazil |
42 |
2 and 3 years |
Pittsburgh Sleep Quality Index |
100 |
Park et al. |
2019 |
South Korea |
237 |
The entire course |
Pittsburgh Sleep Quality Index |
69.6 |
Praxedes et al. |
2020 |
Brazil |
195 |
2nd, 4th, 6th, and 8th semesters |
Pittsburgh Sleep Quality Index |
71 |
Yilmaz et al. |
2017 |
Turkey |
223 |
The entire course |
Pittsburgh Sleep Quality Index |
56 |
Zhang et al. |
2018 |
USA |
242 |
The entire course |
Pittsburgh Sleep Quality Index |
66 |
Naderi et al. |
2021 |
Iran |
143 |
The entire course |
Pittsburgh Sleep Quality Index |
60 |
Pérez et al. |
2023 |
Mexico |
134 |
The entire course |
Pittsburgh Sleep Quality Index |
50 |
Zhang et al. |
2018 |
USA |
242 |
The entire course |
Pittsburgh Sleep Quality Index |
66 |
El Madani et al. |
2023 |
Morocco |
405 |
The entire course |
Pittsburgh Sleep Quality Index |
64 |
Kalal et al. |
2023 |
India |
160 |
The entire course |
Pittsburgh Sleep Quality Index |
40 |
Muñoz et al. |
2023 |
Chile |
165 |
The entire course |
Pittsburgh Sleep Quality Index |
87.8 |
Setyowatia et al. |
2023 |
Indonesia |
150 |
The entire course |
Pittsburgh Sleep Quality Index |
70 |
Silva et al. |
2016 |
Portugal |
403 |
The entire course |
Pittsburgh Sleep Quality Index |
29.5 |
Source: Prepared by the authors.
Methodological Quality Assessment
Figure 2 shows the results of the risk of bias assessment using the JBI tool for prevalence studies, which reported a score of 9 out of 9 for twelve studies, 8 out of 9 for seven studies, and 7 out of 9 for five studies; only one study obtained a score of 5 points. This indicates that all studies except one had a low risk of bias. The study by Nunes 2, classified as having a high risk of bias or low quality, had problems in the detailed description of the subjects and the study setting, in the analyses performed, and in the management of the low response rate of the participants. It was decided not to exclude this article since the sample size (n=42) did not affect the result, and its percentage weight is like that of the other studies included in the meta-analysis, both globally and regionally, in this case, Latin America.
Prevalence of Poor Sleep Quality
Figure 3 shows the grouped prevalence of poor sleep quality in nursing students, determined by a random effects model, which was 65 % (95 % CI 0.55-0.74) with considerable heterogeneity (Q=1334.25, p < 0.005, I2= 98 %), which shows that more than half of nursing students worldwide experience poor sleep quality.
Figure 4 shows the prevalence rates grouped by region of the world and shows that in Latin America, in 8 studies with a total of 1,184 students, the prevalence rate was 84 % (95 % CI 0.65-0.97), with a heterogeneity of (Q=359.80, p < 0.005, I2=98 %). For North America, it was 69 % (95 % CI 0.64-0.73), with 3 studies, 756 participants, and a heterogeneity of (Q=4.08, p= 0.13, I2=51 %). In Europe, a grouped prevalence of 38 % (95 % CI 0.23-0.54) was identified, with 7 studies, 1,860 students, and a heterogeneity of (Q=286.11, p< 0.005, I2=98 %). Finally, for Asia, the grouped prevalence was 66 % (95 % CI 0.57-0.75), with 6 studies, 1,273 participants, and a heterogeneity of (Q=58.05, p< 0.005, I2= 91 %).
Publication Bias or Bias Due to Missing Data
The assessment of publication bias using Egger's test indicates that there is no significant risk for the prevalence of poor sleep quality in students (p=0.11).
Figure 2 Risk of Bias Assessment of the Studies Included
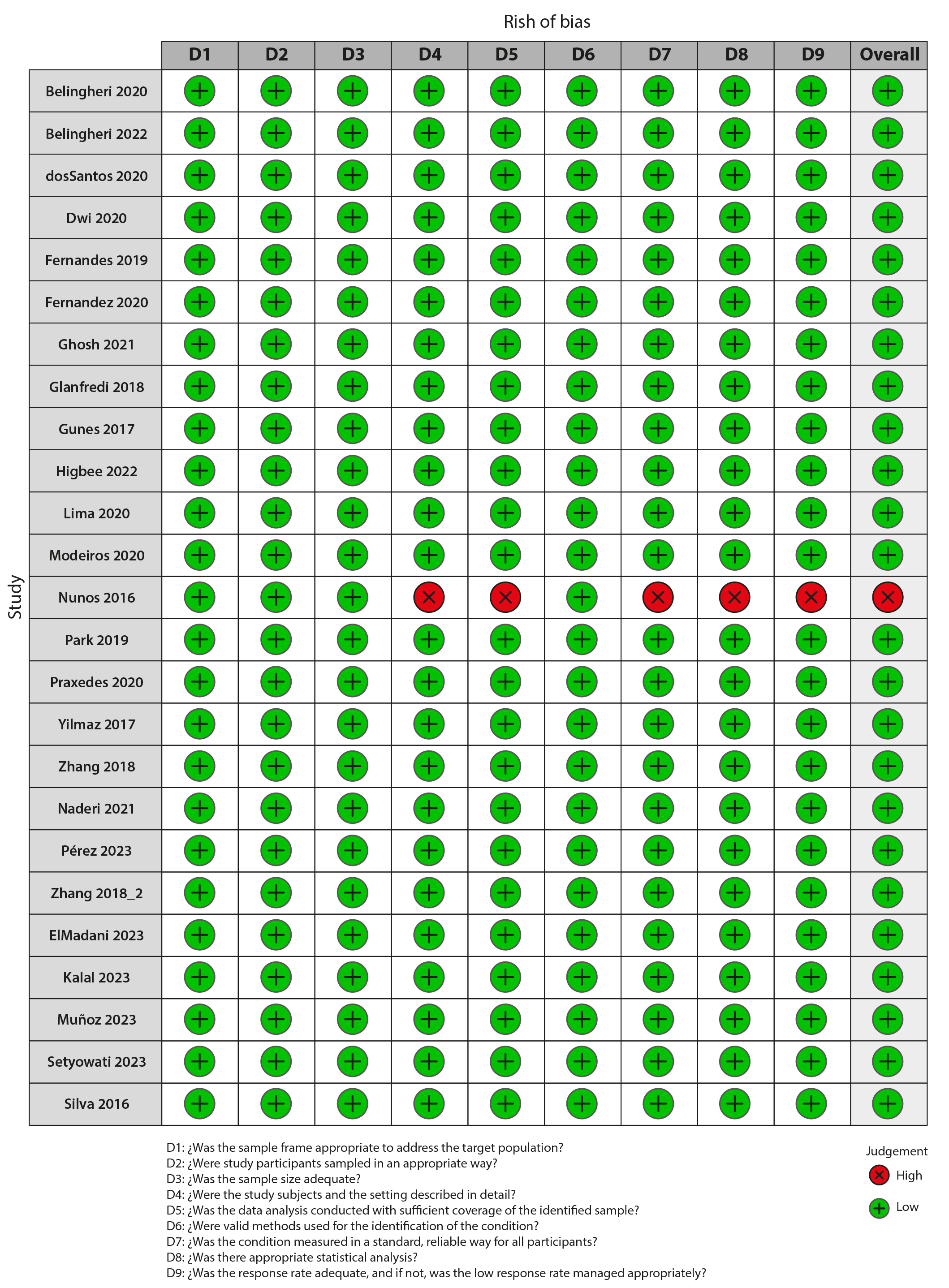
Source: Prepared by the authors.
Figure 3 Prevalence of Poor Sleep Quality Worldwide
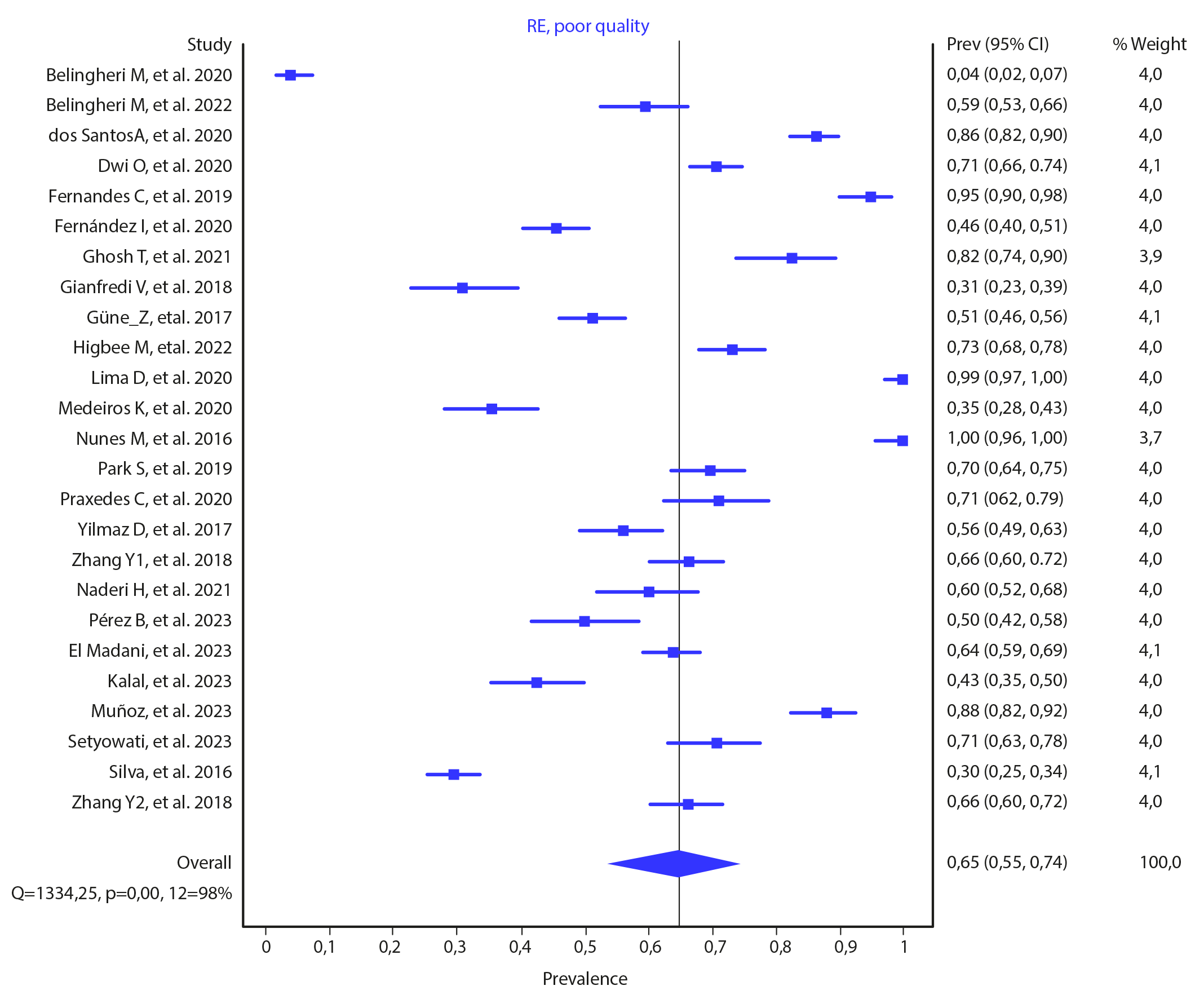
Source: Prepared by the authors.
Figure 4 Prevalence of Poor Sleep Quality by Region of the World
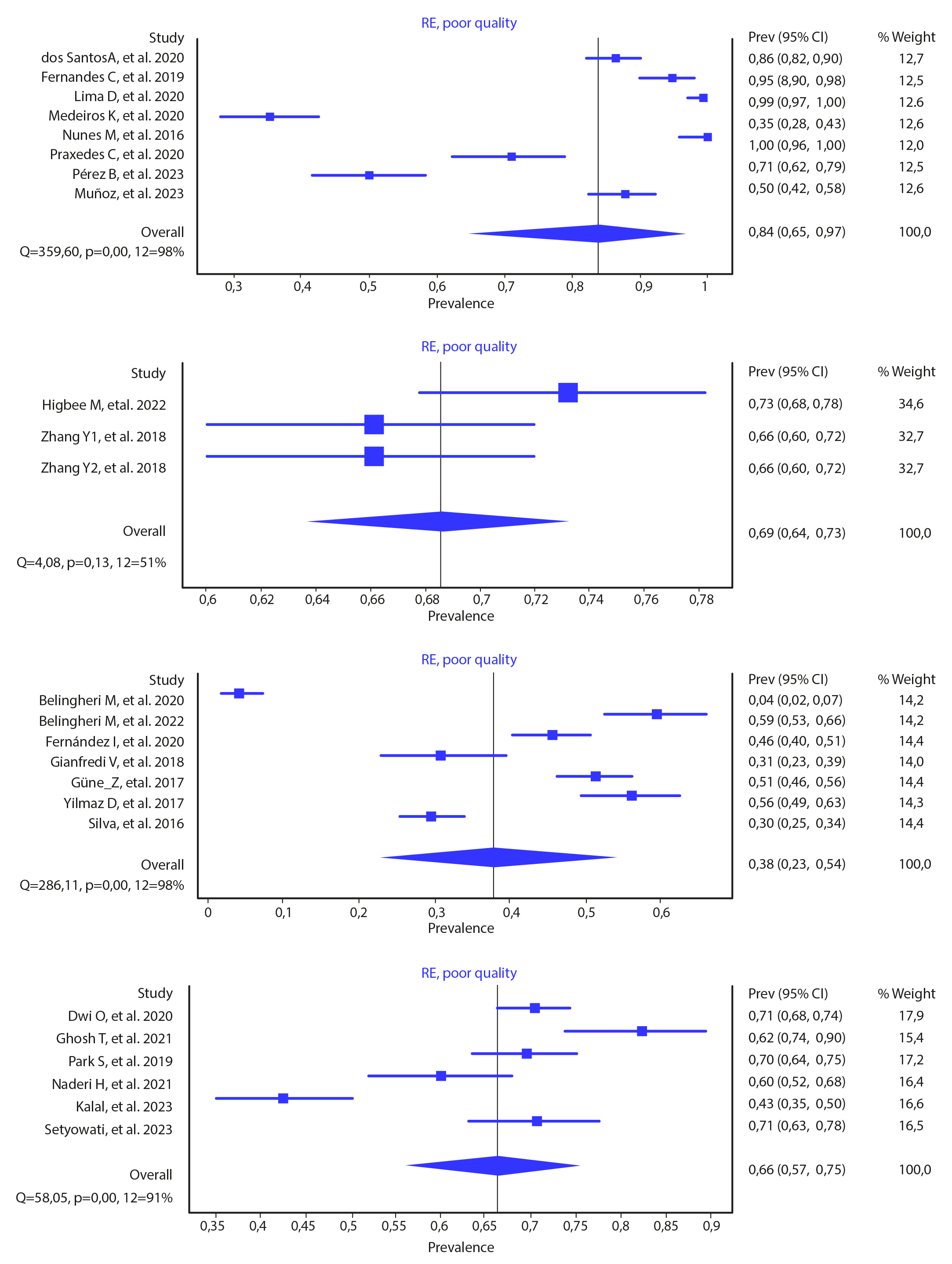
Source: Prepared by the authors.
Figure 5 Publication Bias
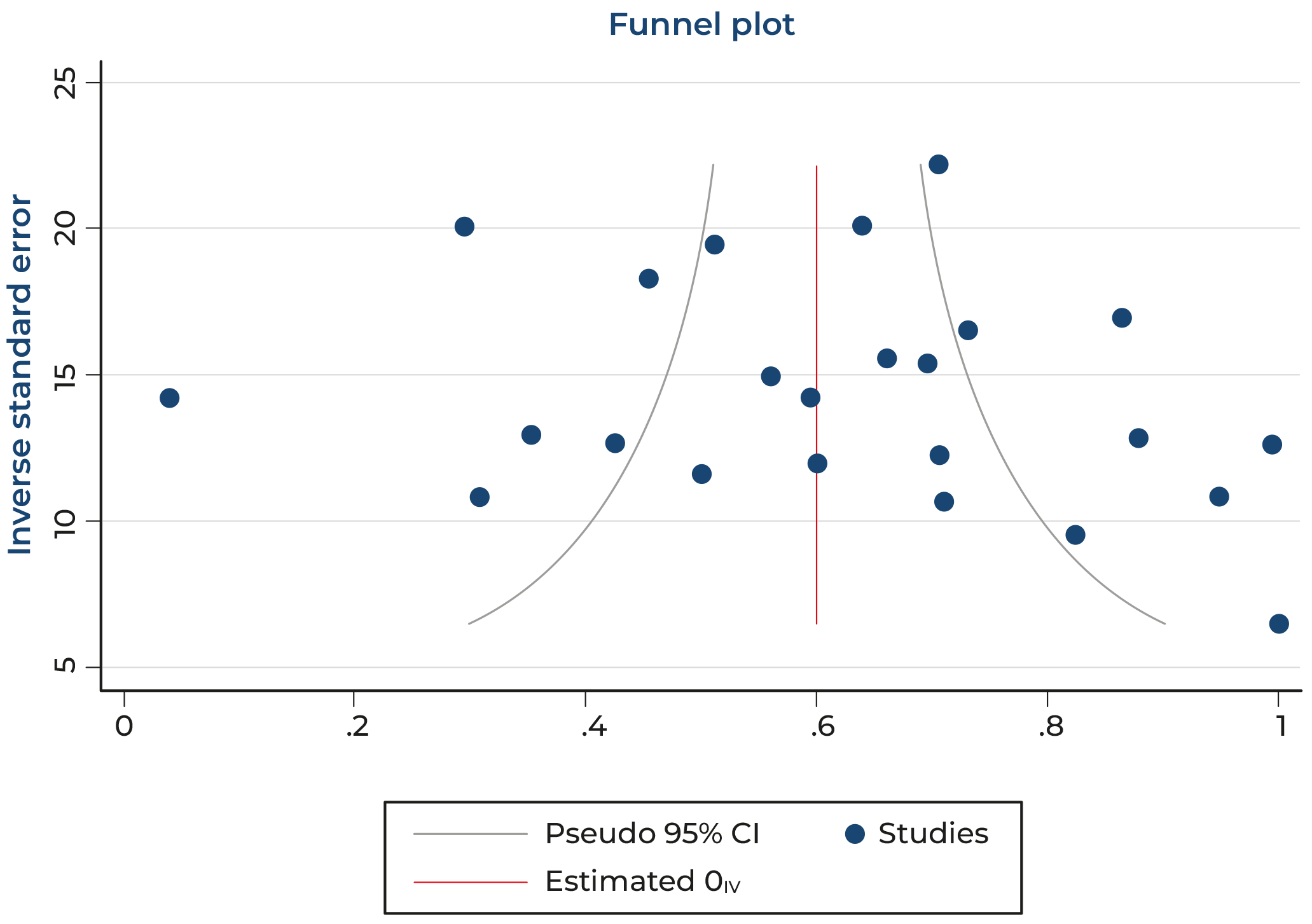
Source: Prepared by the authors.
The purpose of this systematic review and meta-analysis was to evaluate the overall prevalence of sleep quality in nursing students worldwide. Despite the high heterogeneity found in this meta-analysis (I2 = 98 %), the results remain valuable and relevant. The heterogeneity can be attributed to variations in the characteristics of the study population and sample sizes. Other studies conducted on university students have found low sleep quality prevalence rates of 57 % 43 and 63 % 44, close to the overall prevalence rate found in this study: 65 % (95 % CI 0.55-0.74). Subgroup analyses in different regions indicate that a significant part of this variability is reduced when studies with more homogeneous designs and populations are considered. Except for the studies conducted, a consistent general trend of a prevalence of low sleep quality greater than 50 % was found in Europe. This trend was different in Latin American regions, due to socioeconomic conditions and cultural factors that appear to play a crucial role in altering sleep patterns, reflecting population differences between continents. Factors such as economic inequality, limited access to healthcare services, and the high prevalence of informal jobs with irregular hours can significantly influence sleep habits 45. In addition, cultural customs, such as long working hours and a tendency toward nightlife, also contribute to these differentiated patterns, affecting sleep quality compared to other regions of the world.
Although results vary, evidence suggests that poor sleep quality is a common problem in students and persists despite cultural differences. Studies have been conducted in Latin America to assess sleep quality in different types of university students, and the results are like those presented in this study. Among them, de la Portilla et al. 45 found that in the city of Manizales, Colombia, only 24 % of university students had no sleep problems. In nursing students, the prevalence of sleep problems was found to be over 80 %; of these, 24 % had scores close to that of the worst sleep quality 38; furthermore, similar prevalence rates were found in Peru in the same student population 46, which is very different from the population characteristics described above, given that factors related to sleep do not depend solely on physiological aspects, but rather on several other factors.
In terms of factors, Latin American countries are characterized by shift work, many of which are night shifts, differences in labor frameworks, low incomes, and, in some cases, caregiving responsibilities, in addition to social problems. This imbalance can contribute to and increase the probability of psychosocial and physical problems, which can have a direct impact on sleep quality 47. In this regard, it has been reported that the income-needs ratio is associated with a higher prevalence of sleep disorders, which is why the population of some low- and middle-income countries tends to be more affected 48. It should be noted that the possibility of having unstable jobs and unmet needs can contribute to both economic and social stress, and can affect sleep quality with consequences for mental and physical health. This impact can also affect people's general well-being and their environment.
Studies have already reviewed the prevalence of sleep disorders in different types of populations worldwide; a meta-analysis 49 included 89 studies on higher education students, which found that during the pandemic, the prevalence of sleep disorders was 33 %. A relevant aspect is that, while in most studies in Latin America sleep disturbances are attributed to the multiple roles performed by students, in many studies of non-Latin American populations, a large share of these disturbances is associated with mental health disorders and/or problems. This contrast highlights the need to consider the cultural and social context when addressing sleep problems in different populations 50-51. Along the same lines, a meta-analy-sis that evaluated sleep quality in African medical students found a prevalence of 39.8 % 52, while another study 53 with populations from different parts of the world found a prevalence of 55 %; both somewhat lower than that found in this study, which is why it would be necessary to compare the factors related to sleep disorders among nursing and medical students.
Academic demands and chronic stress contribute to sleep disturbances in students, especially in terms of contributing factors such as physical inactivity and the use of psychoactive substances 21. Sleep disturbances and mental health seem to have a bidirectional relationship, cause, and consequence; that is, sleep disorders can trigger anxiety, depression, and, in the long term, dementia; these same conditions are often associated with sleep problems, which can have consequences that are difficult to stabilize and increase or precipitate mental health deterioration. This indicates that the treatment of sleep disorders must be approached holistically and balanced to improve people's quality of life 54-55.
As far as the authors are aware, and based on a review of the previous literature, this is the first systematic review and meta-analysis conducted on nursing students covering sleep quality. This meta-analysis therefore provides a global reference image of the prevalence of poor sleep quality in this population, and although the phenomenon within the included studies was measured using standardized instruments, there was no clinical confirmation of sleep disorders in the participating students. However, this meta-analysis shows a reality that highlights the changes in sleep patterns that students must implement to respond to the demands and requirements of university training processes. Although it varies from country to country and region to region, the prevalences shown indicate that there is at least a minimal impact on this need in this population, which, contrary to what is occurring, requires rest to optimize learning. Therefore, the results of this study should encourage a review of the policies and training plans for nursing professionals to promote truly flexible curricula that contribute to the well-being and quality of life of students and encourage universities to promote sleep care and conservation as a crucial element in people's lives.
In this regard, it is vital that educational institutions develop comprehensive support programs that not only address academic demands but also promote self-care and time management. It is also crucial, within the framework of the academic training of healthcare professionals, to delve into the physiological aspects and architecture of sleep, as well as its implications for people's physical and mental well-being. In the university setting, it is also necessary to implement sleep hygiene strategies among the student population, promote mental health, and provide resources for stress management, including workshops that foster emotional skills such as resilience and emotional intelligence. These programs should be continuous and tailored to the specific needs of students, also integrating personalized counseling and access to recreational and relaxation activities that contribute to a healthy balance between academic and personal life. This will allow for a more holistic approach, where physical, emotional, and mental well-being are addressed comprehensively, creating a more favorable environment for learning and personal development.
In various regions of the world, with a higher prevalence in Latin America, nursing students report poor sleep quality. For this reason, its long-, medium-, and short-term consequences must begin to be studied and measured systematically in university training institutions to propose timely and effective interventions that contribute to satisfaction, harmony, and happiness in studying in a field that contributes to the care of individuals, families, and communities.
This study has some limitations. First, the literature was not identified in all existing and available databases, although an attempt was made by searching for those of greatest worldwide relevance. Second, this review only included studies in English, Portuguese, and Spanish, excluding other languages in which important results on sleep quality in this population have probably also been published. However, these two limitations are unlikely to significantly change the result of the study, since according to this meta-analysis, the prevalence of poor sleep quality in nursing students is high worldwide. Third, the heterogeneity of the studies did not allow for analyses beyond the measurement of prevalence, so it was not possible to report other results related to factors associated with sleep quality. This is important since more rigorous and standardized studies are needed on the factors associated with this phenomenon, allowing for integrative exercises by regions of the world. Although standardized instruments (mainly Pittsburgh's) were used to measure sleep quality, differences in study designs, cultural contexts, and educational systems may have influenced the reported prevalence rates. This scenario reinforces the need to establish more common and global variable measurements. In addition, the lack of clinical confirmation of sleep disorders in participants represents a significant limitation in some studies. Future research must include clinical assessments and consider factors such as sleep duration, sleep efficiency, and the presence of comorbidities to provide a more complete picture of the impact of sleep on nursing students, as well as contextual, family, personal, and educational factors that are contributing to the phenomenon of poor sleep quality.
Conflict of interest: The authors declare that they have no conflicts of interest.
1. Kavurmaci M, Dayapoğlu N, Tan M. Effect of Music Therapy on Sleep Quality. Alternative Therapies. 2020;26(14):22-26. https://pubmed.ncbi.nlm.nih.gov/31221932/
2. Nunes M, Pereira F, Bortolon R, Lunardi W, Ilha S, Martins A. Sleep patterns in nursing students at Public State University. Revista Cubana de Enfermería. 2016;32(2):1-8. http://scielo.sld.cu/scielo.php?script=sci_arttext&pid=S0864-03192016000200003
3. Gallego I, González R, González R, Vera T, Balanza S, Simonelli J, et al. Relationship between Sleep Habits and Academic Performance in University Nursing Students. BMC Nursing. 2021;20(1):1-8. DOI: https://doi.org/10.1186/s12912-021-00635-x
4. Menon B, Karishma P, Mamatha V. Sleep Quality and Health Complaints among Nursing Students. Annals of Indian Academy of Neurology. 2015;18(3):363-364. DOI: https://doi.org/10.4103/0972-2327.157252
5. Fernandes C, da Silva S, da Silva R, Siqueira A, Coelho F, Dantas D, et al. Association of Sleep Quality and Academic Profile with Stress of Nursing Students. Revista Baiana de Enfermagem. 2019;33:1-9. DOI: https://doi.org/10.18471/rbe.v33.33482
6. Kayaba M, Matsushita T, Katayama N, Inoue Y, Sasai-Sakuma T. Sleep-Wake Rhythm and Its Association with Lifestyle, Health- Related Quality of Life and Academic Performance among Japanese Nursing Students: A Cross-Sectional Study. BMC Nursing. 2021;20(225):1-9. DOI: https://doi.org/10.1186/s12912-021-00748-3
7. dos Santos A, Carneiro F, da Silva C, de Souza C, Santos M. Sleep Quality and Associated Factors in Nursing Unadergraduates. Acta Paul Enferm. 2020;33:1-8. DOI: http://dx.doi.org/10.37689/actaape/2020AO0144
8. Chen D, Zhang Y, Lin J, Pang D, Cheng D, Si D. Factors Influencing Bedtime Procrastination in Junior College Nursing Students: A Cross-Sectional Study. BMC Nursing. 2022;21(97):1-9. DOI: https://doi.org/10.1186/s12912-022-00881-7
9. Lima D, de Queiroz E, da Silva R, Siqueira A, das Chagas I, Stina A. Fatores de estresse associados à sintomatologia depressiva e qualidade do sono de acadêmicos de enfermagem. REVISA. 2020;9(4):834-845. DOI: https://doi.org/10.36239/revisa.v9.n4.p834a845
10. Siqueira L, Marques R, Aruaste R, Vieir G, Carneiro F, Pinheiro K, et al. Estresse, má qualidade do sono e desfechos negativos a saúde em estudantes de enfermagem. Journal Health NPEPS. 2021;6(2):164-184. DOI: https://doi.org/10.30681/252610105355
11. Zhang Y, Peters A, Bradstreet J. Relationship among Sleep Quality , Coping Styles, and Depressive Symptoms among College Nursing Students: A Multiple Mediator Model. J Professionel Nursing. 2018;34(4):320-325. DOI: https://doi.org/10.1016/j.profnurs.2017.12.004
12. Park S, Lee Y, Yoo M, Jung S. Wellness and Sleep Quality in Korean Nursing Students: A Cross-Sectional Study. Applied Nursing Research. 2019;48:13-18. DOI: https://doi.org/10.1016/j.apnr.2019.05.008
13. Dwi M, Kuo S, Bloomfield J, Lee H, Ruhyanudin F, Yuangi M, et al. Gender Differences in the Relationship between Sleep Disturbances and Academic Performance among Nursing Students. Nurse Education Today. 2020;85:1-7. DOI: https://doi.org/10.1016/j.nedt.2019.104270
14. Higbee R, Gipson S, El-Saidi M. Caffeine Consumption Habits, Sleep Quality, Sleep Quantity, and Perceived Stress of Undergraduate Nursing Students. Nurse Educator. 2022;47(2):120-124. DOI: https://doi.org/10.1097/NNE.0000000000001062
15. Kotera Y, Cockerill V, Chircop E, Forman D. Mental Heatlh Shame, Self-Compassion and Sleep in UK Nursing Students: Complete Mediation of Self-Compassion in Sleep and Mental Health. Nursing Open. 2021;8(3):1325-1335. DOI: https://doi.org/10.1002/nop2.749
16. Naderi H, Dehghan H, Dehrouyeh S, Tajik E. Academic Burnout among Undergraduate Nursing Students: Predicting the Role of Sleep Quality and Healthy Lifestyle. Research and Development in Medical Education. 2021;10(1):16-16. DOI: https://doi.org/10.34172/rdme.2021.016
17. Owens H, Polivka B, Christian B, King K, Ridner L. Mediating Effect of Sleep Behaviors When Predicting Weight Related Behaviors in Nursing Students. Journal of the American Association of Nurse Practitioners. 2019;31(5):309-318. DOI: https://doi.org/10.1097/JXX.0000000000000151
18. Praxedes C, Soares S, Figueiredo M. Profile of Nursing Students: Quality of Life, Sleep and Eating Habits. Revista Brasileira de Enfermagem. 2020;73(1):1-8. DOI: https://doi.org/10.1590/0034-7167-2019-0365
19. Mulyadi M, Tonapa I, Luneto S, Lin T, Lee O. Prevalence of Mental Health Problems and Sleep Disturbances in Nursing Students during the COVID-19 Pandemic: A Systematic Review and Meta-Analysis. Nurse Education in Practice. 2021;5(7):1-12. DOI: https://doi.org/10.1016/j.nepr.2021.103228
20. Buysse D, Reynolds C, Monk T, Berman R, Kupfer J. The Pittsburgh Sleep Quality Index: A New Instrument for Psychiatric Practice and Research. Psychiatry Res. 1989; 28(2):193-213. DOI: https://doi.org/10.1016/0165-1781(89)90047-4
21. Belingheri M, Luciani M, Ausili D, Paladino E, Di Mauro S, De Vito G, et al. Sleep Disorders and Night Shift Work in Nursing Students: A Cross-Sectional Study. Medicina Del Lavoro. 2022;113(1):1-7. DOI: https://doi.org/10.23749/mdl.v113i1.12150
22. Yilmaz D, Tanrikulu F, Dikmen Y. Research on Sleep Quality and the Factors Affecting the Sleep Quality of the Nursing Students. Current Health Sciences Journal. 2017; 43(1):20-24. DOI: https://doi.org/10.12865/CHSJ.43.01.03
23. Güneş Z, Arslantaş H. Insomnia in Nursing Students and Related Factors: A Cross-Sectional Study. International Journal of Nursing Practice. 2017;23(5):1-10. DOI: https://doi.org/10.1111/ijn.12578
24. Ghosh T, Sarkar D, Sarkar K, Dalai, Ghosal A. A Study on Smartphone Addiction and Its Effects on Sleep Quality among Nursing Students in a Municipality Town of West Bengal. Journal of Family Medicine and Primary Care. 2021;10(1):378-386. DOI: https://doi.org/10.4103/jfmpc.jfmpc_1657_20
25. Gardani M, Bradford R, Russell K, Allan S, Beattie L, Ellis G, et al. A Systematic Review and Meta-Analysis of Poor Sleep, Insomnia Symptoms and Stress in Undergraduate Students. Sleep Medicine Reviews. 2022;61:1-17. DOI: https://doi.org/10.1016/j.smrv.2021.101565
26. Seoane A, Moschetto L, Orliacq F, Orliacq J, Serrano E, Cazenave I, et al. Sleep Disruption in Medicine Students and Its Relationship with Impaired Academic Performance: A Systematic Review and Meta-Analysis. Sleep Medicine Reviews. 2020;53:1-10. DOI: https://doi.org/10.1016/j.smrv.2020.101333
27. Munn Z, MClinSc M, Lisy K, Riitano D, Tufanaru C. Methodological Guidance for Systematic Reviews of Observational Epidemiological Studies Reporting Prevalence and Cumulative Incidence Data. International Journal of Evidence-Based Healthcare. 2015;13(3):147-153. DOI: https://doi.org/10.1097/XEB.0000000000000054
28. Page M, McKenzie J, Bossuyt P, Boutron I, Hoffman T, Mulrow C, et al. Declaración PRISMA 2020: una guía actualizada para la publicación de revisiones sistemáticas. Rev Esp Cardiol. 2021;74(9):790-799. DOI: https://doi.org/10.1136/bmj.n71
29. Munn Z, Moola S, Riitano D, Lisy K. The Development of a Critical Appraisal Tool for Use in Systematic Reviews Addressing Questions of Prevalence. International Journal of Health Policy and Management. 2014;3(3):123-128. DOI: https://doi.org/10.15171/ijhpm.2014.71
30. McGuiness L, Higgins J. Risk-of-bias VISualization (robvis): An R Package and Shiny Web App for Visualizing Risk-Of-Bias Assessment. Res Synth Methods. 2021;12(1):55-61. DOI: https://doi.org/10.1002/jrsm.1411
31. Barendregt J, Doi A, Lee Y. Meta-Analysis of Prevalence. J Epidemiol Community Health. 2013; 67:974-978. DOI: https://doi.org/10.1136/jech-2013-203104
32. Medeiros K, Figueiredo M, Bandeira C, Lima A, da Silva D, Targino J. Stress and Quality Of Sleep In Undergraduate Nursing Students. Revista Brasileira de Enfermagem. 2020;73(1):1-6. DOI: https://doi.org/10.1590/0034-7167-2018-0227
33. Belingheri M, Pellegrini A, Facchetti R, De Vito G, Cesana G, Riva A. Self-Reported Prevalence of Sleep Disorders among Medical and Nursing Students. Occupational Medicine. 2020;70:127-130. DOI: https://doi.org/10.1093/occmed/kqaa011
34. Gianfredi V, Nucci D, Tonzani A, Amodeo R, Benvenuti A, Villarini M, et al. Sleep Disorders, Mediterranean Diet and Learning Performance among Nursing Students: Insomnia, A Cross-Sectional Study. Ann Ig. 2018;30:470-481. DOI: https://doi.org/10.7416/ai.2018.2247
35. Zhang Y, Peters A, Chen G. Perceived Stress Mediates the Associations between Sleep Quality and Symptoms of Anxiety and Depression among College Nursing Students. International Journal of Nursing Education Scholarship. 2018;2017:1-9. DOI: https://doi.org/10.1515/ijnes-2017-0020
36. Setyowati L, Dwi A, Lestari W, Karuncharernpanit S. Association between Social Media Addiction and Sleep Quality amog Undergraduate Nursing Students: A Cross-Sectional Study. Frontiers of Nursing. 2023;10(2):233-239. DOI: https://doi.org/10.2478/fon-2023-0025
37. Kalal N, Vel N, Angmo S, Choyal S, Bishnoi S, Dhaka S, et al. Smartphone Addiction and Its Impact on Quality of Life of Sleep and Academic Performance among Nursing Students. Institutional Based Cross-Sectional Study in Western Rajasthan (India). Invest. Educ. Enferm. 2023;41(2):135-146. DOI: https://doi.org/10.17533/udea.iee.v41n2e11
38. Muñoz C, Mendoza P, Olivares C, Palma C, Vidal L. Sleep in Nursing Students at a University in Southern Chile. Horizonte de Enfermería. 2023;34(3):610-623. DOI: https://doi.org/10.7764/Horiz_Enferm.34.3.610-623
39. Pérez B, Lara R, Aguilera P, Fang M, Flores F. Asociación entre calidad y cantidad de sueño con índice de masa corporal en adolescentes universitarios: Estudio transversal. Rev Cuid. 2023;14(3):1-11. DOI: https://doi.org/10.15649/cuidarte.3032
40. Fernandez I, Ruiz M, Hernández J, Granero J, Fernández C, Jiménez M, et al. Adherence to the Mediterranean Diet and Self-efficacy as Mediators in the Mediation of Sleep Quality and Grades in Nursing Students. Nutrients. 2020; 12:32-65. DOI: https://doi.org/10.3390/nu12113265
41. El Madani H, El Harch I, Tachfouti N, El Fakir S, Aalouane R, Berraho M. Psychological Stress and Its Related Factors among Moroccan Nursing Students: A Cross-Sectional Study. Enfermería Clínica. 2023;33:205-2015. DOI: https://doi.org/10.1016/j.enfcle.2023.02.001
42. Silva M, Chaves C, Duarte J, Amaral O, Ferreira M. Sleep Quality Determinants among Nursing Students. Procedia - Social and Behavioral Sciences. 2016;217:999-1007. DOI: https://doi.org/10.1016/j.sbspro.2016.02.090
43. Leow H, Chiang J, Chua X, Wang S, Tan C. The Relationship between Smartphone Addiction and Sleep among Medical Students: A Systematic Review and Meta-Analysis. PLoS ONE. 2023;18(9):1-14. DOI: https://doi.org/10.1371/journal.pone.0290724
44. Nakie G, Takelle M, Rtbey G, Andualem F, Tinsae T, Kassa A, et al. Sleep Quality and Associated Factors among University Students in Africa: A Systematic Review and Meta-Analysis Study. Frontiers in Psychiatry. 2024;15:1-15. DOI: https://doi.org/10.3389/fpsyt.2024.1370757
45. de la Portilla S, Dussán C, Montoya M, Taborda J, Nieto S. Sleep Quality and Excessive Day Drowsiness in University Students from Different Careers. Hacia La Promoción de La Salud. 2019;24(1):84-96. DOI: https://doi.org/10.17151/hpsal.2019.24.1.8
46. Granados Z, Bartra A, Bendezú D, Huamanchumo J, Hurtado E, Jiménez J, et al. Calidad del sueño en una facultad de medicina de Lambayeque. An Fac Med. 2013;74(4):311-314. http://www.scielo.org.pe/scielo.php?script=sci_arttext&pid=S1025-55832013000400008
47. Zapata S, Betancourt J. Cambios en la calidad del sueño durante el semestre académico en estudiantes de la salud. Universidad y Salud. 2023;25(1):7-14. DOI: https://doi.org/10.22267/rus.232501.290
48. Sosso E, Khoury T. Socioeconomic Status and Sleep Disturbances among Pediatric Population: A Continental Systematic Review of Empirical Research. Sleep Science. 2021;14(3):245- 256. DOI: https://doi.org/10.5935/1984-0063.20200082
49. Deng J, Zhou F, Hou W, Silver Z, Wong Y, Chang O, et al. The Prevalence of Depressive Symptoms, Anxiety Symptoms and Sleep Disturbance in Higher Education Students during the COVID-19 Pandemic: A Systematic Review and Meta-Analysis. Psychiatry Research. 2021;301:1-21. DOI: https://doi.org/10.1016/j.psychres.2021.113863
50. Akhtarul M, Barna D, Raihan H, Nafiul M, Tanvir M. Depression and Anxiety among University Students during the COVID-19 Pandemic in Bangladesh: A Web-Based Cross-Sectional Survey. PLoS ONE. 2020;15(8):1-12. DOI: https://doi.org/10.1371/journal.pone.0238162
51. Ibrahim K, Kelly J, Adams E, Glazebrook C. A Systematic Review of Studies of Depression Prevalence in University Students. Journal of Psychiatric Research. 2013;47(3):391-400. DOI: https://doi.org/10.1016/j.jpsychires.2012.11.015
52. Gao C, Guo J, Gong T, Lv J, Li X, Liu F, et al. Sleep Duration/Quality with Health Outcomes: An Umbrella Review of Meta-Analyses of Prospective Studies. Frontiers in Medicine. 2022;8:1-15. DOI: https://doi.org/10.3389/fmed.2021.813943
53. Binjabr A, Alalawi S, Alzahrani A, Albalawi S, Hamzah H, Ibrahim S, et al. The Worldwide Prevalence of Sleep Problems Among Medical Students by Problem, Country, and COVID-19 Status: a Systematic Review, Meta-analysis, and Meta-regression of 109 Studies Involving 59427 Participants. Current Sleep Medicine Reports. 2023;9(3):161-179. DOI: https://doi.org/10.1007/s40675-023-00258-5
54. Mansano C, Ceolim F. Factors Associated with Poor Sleep Quality in Women with Cancer. Revista Latino-Americana de Enfermagem. 2017;25:1-8. DOI: https://doi.org/10.1590/1518-8345.1478.2858
55. Sánchez S, Solarte E, Correa T, Imbachí Y, Anaya L, Mera Y, et al. Factores relacionados con la calidad del sueño y la somnolencia diurna en universitarios del suroccidente colombiano. Duazary. 2021;18(3):232-246. DOI: https://doi.org/10.21676/2389783X.4230