Women with Cervical Cancer:
Perceptions about the Papanicolaou Test3
Las mujeres con cáncer de cuello uterino:
percepciones acerca de la prueba de Papanicolaou
As mulheres com câncer de colo do útero:
percepções sobre o exame Papanicolaou
Received: February 4, 2013
Sent to for review: February 14, 2013
Accepted by the reviewers: June 18, 2015
Approved: July 6, 2015
Maria-Teresa Urrutia1
Lauren Poupin2
1 Ph.D., Pontificia Universidad Católica de Chile, Chile.
murrutis@uc.cl
2 Nurse Midwifery, Master Public Health.
lpoupin@gmail.com
3 This research was supported by FONIS (Fondo Nacional de Investigacion en Salud) SA05I20047, CONICYT, MINSAL, Chile. We thank the women who participated in this study.
Para citar este artículo / To reference this article / Para citar este artigo
Urrutia MT. Poupin L. Women with Cervical Cancer: Perceptions about the Papanicolaou Test, Aquichan. 2015;15(4):499-507. DOI: 10.5294/aqui.2015.15.4.5
|
ABSTRACT Objective: Examine perceptions about the Papanicolaou (Pap) test from the perspectives of Chilean women with cervical cancer. Design: A descriptive, cross-sectional study conducted in Santiago, Chile. Participants: 127 Chilean women. Results: The principal reasons for not having had a PAP test were procrastination and barriers related to fear, embarrassment, discomfort, not caring, lack of time, and lack of knowledge. Conclusion: All the reasons given by the Chilean women who took part in the study must be considered by health care professionals who are in a position to advocate for education and cervical cancer screening for women, especially in countries where the disease is still prevalent. These results can serve as a guide for education programs and can be applied in intervention research. KEYWORDS Pap test, cancer, barriers (Source: DeCs, BIREME). |
RESUMEN Objetivo: examinar las percepciones acerca de la prueba de Papanicolaou (Pap) desde la perspectiva de las mujeres chilenas con cáncer cervical. Diseño: un estudio descriptivo, transversal realizado en Santiago, Chile. Participantes: ciento veintisiete mujeres chilenas. Resultados: Las principales razones para no haber hecho la prueba de PAP fueron dilación y obstáculos relacionados con el miedo, la vergüenza, la incomodidad, el hecho de no estar preocupada, la falta de tiempo y la falta de conocimiento. Conclusión: todas las razones dadas por las mujeres chilenas que participaron en el estudio deben ser considerados por los profesionales de la salud que están en una posición para abogar por la educación y la detección del cáncer cervical para las mujeres, especialmente en países donde la enfermedad sigue siendo prevalente. Los resultados pueden servir como una guía para los programas de educación y pueden ser aplicados en la investigación sobre la intervención. PALABRAS CLAVE Prueba de Papanicolaou, el cáncer, las barreras (Fuente: DeCS, BIREME). |
RESUMO Objetivo: examinar as percepções sobre o exame Papanicolaou do ponto de vista das mulheres chilenas com câncer cervical. Desenho: estudo descritivo, transversal, realizado em Santiago (Chile), com 127 mulheres chilenas. Resultados: as principais razões para não terem feito o exame Papanicolaou foram dilação e obstáculos relacionados com o medo, a vergonha, o desconforto, o fato de não estar preocupada, a falta de tempo e a falta de conhecimento. Conclusão: todas as razões dadas pelas mulheres chilenas que participaram do estudo devem ser consideradas pelos profissionais da saúde que estão em condição de defender a educação e a detenção do câncer cervical, especialmente em países onde a doença continua sendo prevalente. Os resultados podem servir como um guia para os programas de educação e podem ser aplicados na pesquisa sobre a intervenção. PALAVRAS CLAVE Exame Papanicolaou, câncer, barreiras (Fonte: DeCS, BIREME). |
Introduction
Cervical cancer (CC) accounts for approximately 10% of all new cases of cancer worldwide (1). CC is one of the cancers with the highest mortality rate in the world (2). In 2005, there were over 500,000 new cases of CC, and over 90% of them were in developing countries (3). Every year, there are 33,000 women who die of CC in Latin America and the Caribbean (4). Over the past three decades, CC rates have fallen in most of the developed world. In contrast, these rates in most developing countries have risen or remained unchanged (3).
Experience in developed countries has shown organized screening programs can significantly reduce CC incidence and mortality (3, 5). The difference between developed and developing countries reflects inequalities in health care and, therefore, is a challenge for global health (3).
Although several tests can be used in screening for CC, the Papanicolaou (Pap test) is the only one that has been shown to reduce CC incidence and mortality (3). In fact, it is still considered the principal method for early detection of carcinoma of cervix (6). Cervical cancer control can be achieved if screening is organized and as many women as possible in the target group are screened (3). For this reason, it is important to know what barriers exist to participating in PAP testing.
In studies of Central and South American women, the factors found to be related to participation in CC screening include: knowledge about the Pap test (7, 8), gynecological symptoms (7,8), being over age 30, a higher socioeconomic level (9), higher education, having medical insurance, and having a primary health care provider (9, 10). The aim of this study was to examine Chilean women's perceptions concerning the Pap test.
Methods
Design and Sample
The ethics committees from the Pontificia Universidad Católica de Chile School of Nursing and the Southeast Metropolitan Public Health Service (Servicio de Salud Metropolitano Sur-Oriente, Santiago, Chile) reviewed and approved this research. Written informed consent was obtained from the women participants.
Women's perceptions about participating in Pap testing, from the perspective of Chilean women with CC, were examined using a descriptive, cross sectional design. Content analysis of personal interviews generated a thematic description of the women's perceptions about obtaining PAP testing.
The sample included 127 women who sought care at urban health clinics of the Southeast Metropolitan Public Health Service in Santiago, Chile. The women who go to these clinics are low-income and receive health care at two public hospitals. The women all had a diagnosis of CC, confirmed by biopsy, and received health care from the Cervical Cancer "AUGE" Program during 2004 and 2005. AUGE is a new program in Chile; the acronym stands for "Universal Access to Explicit Guaranties in Health" [Acceso Universal a Garantías Explícitas en Salud]. The women were enrolled in the study between May 2006 and October 2006.
Data Collection and Analysis
Data collection was conducted by twelve baccalaureate-prepared nurse midwives who interviewed the women in their homes. The interviewers were trained in a one-day educational session. The training included content about CC, an explanation about the study, and an introduction to the questionnaire. The nurse midwives role-played conducting the interviews, and rehearsed how to elicit responses. This study analyzed the answer to two questions: 1) "Why do you think women do not get a Pap test?" and 2) "Why do you think women do not return to the clinic for the results of their Pap test?" The answers were recorded verbatim on the interview form.
Content analysis was used according to the methods described by Krippendorf (11). The unit of analysis was a sentence or phrase that represented one idea. The first level of analysis involved identifying the common ideas; the second level of analysis was to group the common ideas into like themes. The criterion for a theme was that each theme demonstrated an originally different topic with respect to the others. The themes describe the responses the women gave to the questions about having a Pap test and obtaining the results of the test. The first and second levels of analysis were performed by the two authors separately, then discussed until a consensus was reached. The number of women who contributed to each theme was calculated.
Findings
The 127 participants ranged in age from 25 to 81; the mean age was 49 (SD ± 13). Twenty-eight percent of the women had never had a Pap smear before being diagnosed with CC.
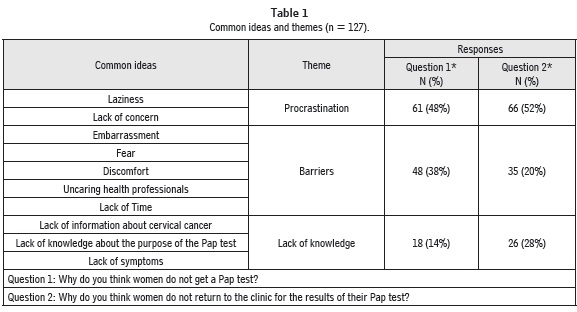
The analysis of the responses to the questions about why women do not get a Pap test and why women do not return to the clinic for their results was summarized into three themes. The themes were: 1) Procrastination, 2) Barriers, and 3) Lack of Knowledge. Procrastination was a tactic used to put off obtaining the Pap test and/or claiming the test results. Barriers to having a Pap test included embarrassment, discomfort, lack of caring by health professionals, and lack of time. The barrier to obtaining Pap test results was fear of a cancer diagnosis. Lack of knowledge was related to the need for information about CC screening and diagnosis (see Table 1).
Procrastination
Procrastination was the tactic used by a majority of the women to delay getting a PAP test and to put off claiming the results. Forty-eight percent (n = 61) of the women used procrastination excuses to postpone getting a PAP test, and 52% (n = 66) used procrastination excuses for not claiming their PAP test results. These characteristics are individual attributes that would prevent women from performing any health behavior. Some women attributed their procrastination to a lack concern about their health over the demands of caring for others. Chilean women put the needs of family members first, before their own . One woman said "Las mujeres no se preocupan por si mismas, siempre son otros más importantes que ella." [Women don't worry about themselves, others are always more important.] Other women attributed their procrastination to "laziness". One woman said, 'Algunas veces la mujer se olvida y dice... cuando vaya a control, voy a pedirlo...pero eso nunca pasa." [Sometimes, a woman forgets and says to herself, "When I go for a routine check-up, I will request it. ..but it never happens"],
Barriers
Thirty-eight percent (n=48) of the women reported barriers to having a PAP test, and 20% (n=35) reported barriers to claiming PAP test results. The barriers are related to negative experiences the women had. Embarrassment, discomfort, and an uncaring attitude on the part of health professionals were the barriers reported by the women. One woman said, "Es muy vergonzoso para la mujer Algunas veces duele y es incómodo. Además los profesionales no la tratan bien." [It (PAP test) is very embarrassing for a woman. It is sometimes painful and you feel uncomfortable. Also, health care professionals aren't very kind or considerate to women.]
Fear was identified as a reason why the women did not return to the clinic to get their results. Women were afraid the PAP test result would show cancer. Women said, "Algo puede estar mal." [ Something could be wrong.] As for the PAP test result, it was said, "Las mujeres tienen temor a lo que el PAP pueda encontrar." [Women fear what the PAP test might find.] One woman said, "...miedo a la palabra cáncer, a saber que ellas tienen algo malo." [...fear of the word cancer, fear if knowing they have something bad].
Lack of time also was reported as a reason for not having the PAP test and for not getting the results of the test. One woman said. "La mujer tiene problemas para ir al médico, porque la mujer trabaja, y no puede pedir permiso." [It is a problem for a woman to go to the doctor's office, because if the woman works, she can't get time off]
Lack of Knowledge about CC
Fourteen percent of the participants (n=18) reported a lack of knowledge about CC as a reason why women do not get a PAP test, and 28% (n=26) said lack of knowledge contributed to not claiming PAP test results. Women expressed the need for more information about cervical cancer, including screening and diagnosis. One woman said, "Falta información; las mujeres ven distante la posibilidad de tener cáncer." [Women lack information and do not consider cancer as a possible diagnosis for themselves].
The women reported they did not think a PAP test was necessary if one had no symptoms that indicated something was wrong. One of the women said,"...porque ella cree que está bien, que está sana." [...because she thinks she is healthy and well.] "...Si ellas se sienten bien, ¿por qué necesitan ir?"[If they feel fine, why do they need to go?], "Si ella está sana, no necesita el examen." [If she is healthy, she does not need the test].
Discussion
Chile is a South American country where CC claims the lives of many women. The incidence of CC in Chile was 18.7/100,000 women in 2003, with a mortality rate of 8.5 /100,000. This study sought to explain what Chilean women understand about the PAP test, which is the major screening test for CC.
It is the first qualitative study designed to ask Chilean women with cervical cancer about their views on the Pap test. One limitation of the study is that only women with CC were interviewed and the results are not representative of the Chilean context, owing to the methodology used. Because these women were diagnosed and treated for CC, this group is more sensitive to the topic. Therefore, these women may have given a great deal of thought as to how their cancer might have been prevented. However, a similar study was conducted with a group of women in Chile who do not have CC , and the results were very similar to those of this study (12).
The theme of procrastination found in this sample is similar to the finding of McFarland (13), who detected a "lack of motivation" to obtain the Pap test among women in Botswana. Byrd and colleagues also reported procrastination among Hispanic women in Texas (14). The procrastination noted in this study was the principal answer to both study questions; therefore, it should be considered in future nursing education interventions.
The women in this study reported barriers to getting a Pap test and to claiming the test results; these include fear, embarrassment, discomfort, uncaring professionals, and lack of time. Fear has been reported as related to pain, and to the diagnosis as well (12,15,16). It also has been cited as a reason for not taking the Pap test (17). Similar to our finding, fear was related to the test result and to the pain associated with the pelvic exam (14, 18). In fact, some women believed a piece of the uterus would be cut during the exam (19).
As in the study described here, others have reported women expressed embarrassment about exposing their genitals during a PAP test (18-22). Some women said they would like to substitute the PAP test for another, less embarrassing procedure (14). The percentage of Hispanic women who have cited embarrassment as a barrier is nearly 50% (20); it was as high as 87% in a study of Brazilian women (23).
The women in our study said uncaring behavior by health care professionals was a barrier to getting a Pap test. Others have reported similar issues, such as long waiting times (19, 24), poor physical facilities (24), poor communication on the part of health care professionals (13, 19), lack of continuity with health care professionals (21), and difficulty in PAP test scheduling (21). Long waiting times to obtain health care is a common situation in Latin American countries, and women have reported long waiting times as a barrier to obtaining health care (25).
With respect to the waiting time for health care, it is a situation previously described in other Latin American countries, where women said it has been a factor in lessening their interest to come back again for health care (25). Women have reported that having a male health care professional is a barrier to getting a Pap test (13,15, and 26). If women are not comfortable with a health care provider or the environment at a clinic, they may not want to return for the results of a Pap test. This is an important point to bear in mind.
Not having enough time to obtain a PAP test was reported by the women in our study, as well as by others (14,24). The reasons included long waiting times at clinics (15, 23), not being able to take time off from work (27) or difficulty in scheduling appointments. The issue of taking time off from work is becoming more important, because 40.3% of Chilean women are now employed (28). The increase in the work force can explain the lack of time or the difficulties women have with the Pap test. The solution to scheduling appointments at convenient times for women with family responsibilities and for working women rests with the Chilean health care system. The health care system must become responsive to women's need for flexibility in scheduling appointments on Saturdays and in the evening.
A lack of knowledge about CC symptoms and screening was reported by the women in our sample. Others have reported that lack of knowledge about PAP testing is found worldwide (13, 29,33). Women reported not knowing about the importance of screening (14, 18) and about how to obtain a Pap test (14,18). They also reported a lack of knowledge about their reproductive anatomy (30). In a sample of adolescents, some believed the PAP test was the same as a pelvic exam (29). In a South African study (34), women thought a PAP test was a treatment for infertility, or that it was a "cleaning of the womb". Some women believed a piece of the uterus would be cut during the exam (19). Clearly, there is a need for education to help women understand what CC is, its anatomic location, screening for CC, and the importance of detection.
The same as was reported by others, the women in our sample interpreted a lack of symptoms to mean there was no need for a PAP test (13, 17, and 34). The women thought pain or abnormal bleeding were necessary indicators for a Pap test. This belief indicates a lack of knowledge about the preventive purpose of the Pap test to detect cervical cancer.
Conclusion
The US Centers for Disease Control (CDC) has identified the need to increase access to CC early detection and treatment services, to develop strategies for better screening for women, and to implement public education (35). WHO has charged health professionals with designing and implementing interventions to reduce CC in the Latina population (3).
This study provides insights into how Chilean women view Pap testing. The Chilean women in this study reported: a) using procrastination to delay obtaining a Pap test, b) barriers to obtaining a Pap test, including embarrassment and lack of time, and c) a lack of knowledge about CC and the purpose of the Pap test.
Health care professionals are in a good position to address the concerns expressed by women about PAP testing. First, they must lead information campaigns about cervical cancer and the need for screening. This could be accomplished by securing funding and creating posters to be displayed in public transportation systems. Secondly, they can provide education programs to increase knowledge about CC. Education can be imparted on a one-to-one basis during primary or obstetrics and gynecology care. Third, they can protect women's need for privacy to minimize embarrassment during PAP testing. Finally, clinical environments need to be changed to provide timely and sensitive care. Health care professionals can be advocates for making changes in the health care delivery system.
The health care professional's role is to empower women with respect to their responsibility and participation in self-care, without forgetting the responsibility health care providers have to convey test results appropriately. It is necessary to be sure women understand the procedures at clinics. Understanding and shielding or protecting women is a task nurses must perform. Women's health is an important issue, and it is necessary for health care professionals to work in the best way possible to achieve that goal.
References
1. Orbell, S., Hagger, M., Brown, V., & Tidy, J. (2006). Comparing two theories of health behavior: a prospective study of noncompletion of treatment following cervical cancer screening. Health Psychology, 25(5), 604-615.
2. OPS. (2007). Prevención y detección temprana pueden evitar una escalada de muertes por cáncer en las Américas. Retrieved September, 1, 2008, from http://www.paho.org/Spanish/DD/PIN/ps070204.htm
3. WHO. (2006). Comprehensive cervical cancer control. A guide to essential practice. Retrieved January, 25, 2007, from http://www2.alliance-hpsr.org/reproductivehealth/publications/cervical_cancer_gep/text.pdf
4. OPS. (2008). Expertos en la Américas piden mejoras para evitar muertes por cáncer de cuello uterino. Retrieved September1, 2008, from http://www.paho.org/Spanish/DD/PIN/ps080514.htm
5. PAHO, & WHO. (2007). Regional Strategy and Plan of Action for Cervical Cancer Prevention and Control. Retrieved September1, 2008, from http://www.paho.org/English/GOV/CE/ce14014-e.pdf
6. Michalas, S. P. (2000). The Pap test: George N. Papanicolaou (1883-1962). A screening test for the prevention of cancer of uterine cervix. European Journal of Obstetrics, Gynecology,and Reprodustive Biology, 90(2), 135-138.
7. Aguilar-Perez, J. A., Leyva-Lopez, A. G., Angulo-Najera, D., Salinas, A., & Lazcano-Ponce, E. C. (2003). [Cervical cancer screening: knowledge of Pap smear benefits and utilization in Mexico]. Revista Saude Publica, 37(1), 100-106.
8. Lazcano-Ponce, E., Moss, S., Cruz-Valdez, A., Alonso de Ruiz, P., Casares-Queralt, S., Martinez-Leon, C., et al. (1999). Factores que determinan la participación en el tamizaje de cáncer cervical en el estado de Moreros. Salud Publica de México, 41(4), 278-285.
9. Lucumi, D., & Gomez, L. (2004). Accesibilidad a los servicios de salud en la práctica de citología reciente de cuello uterino en una zona urbana de Colombia. Revista Espanola de Salud Publica, 78, 367-377.
10. Oliveira, M. M., Silva, A., Oliveira, L., & L., C. (2006). Coverage and factors associated with not performing Pap smear screening tests in São Luís, Maranhão, Brazil. Rev Bras. Epidemiol., 9(3), 325-334.
11. Krippendorf, K. (2004). Content Analysis. An introduction to its methodology. Thousand Oaks: Sage Publications.
12. Urrutia, M.T., Poupin, L., Concha, X., Viñales, D., Iglesias, C., Reyes, V. (2008)¿Por que las mujeres no se toman el Papanicolaou? Barreras percibidas por un grupo de mujeres ingresadas al programa de cáncer cérvicouterino AUGE. Revista Chilena de Obstetricia y Ginecología, 73(2), 98-103.
13. McFarland, D. M. (2003). Cervical cancer and Pap smear screening in Botswana: knowledge and perceptions. International Nursing Review, 50(3), 167-175.
14. Byrd, T. L., Chavez, R., & Wilson, K. M. (2007). Barriers and facilitators of cervical cancer screening among Hispanic women. Ethnicity & Disease, 17(1), 129-134.
15. Agurto, I., Bishop, A., Sanchez, G., Betancourt, Z., & Robles, S. (2004). Perceived barriers and benefits to cervical cancer screening in Latin America. Preventive Medicine, 39(1), 91-98.
16. Hunter, J. L. (2005). Emelda's story: applying ethnographic insights to cultural assessment and cervical cancer control. Journal of Transcultural Nursing, 16(4), 322-330.
17. Lee-Lin, F., Pett, M., Menon, U., Lee, S., Nail, L., Mooney, K., et al. (2007). Cervical cancer beliefs and pap test screening practices among Chinese American immigrants. Oncology Nursing Forum, 34(6), 1203-1209.
18. Ho, V., Yamal, J. M., Atkinson, E. N., Basen-Engquist, K., Tortolero-Luna, G., & Follen, M. (2005). Predictors of breast and cervical screening in Vietnamese women in Harris County, Houston, Texas. Cancer Nursing, 28(2), 119-129; quiz 130-111.
19. Wiesner -Ceballos, C., Vejarano -Velandia, M., Caicedo -Mera, J. C., Tovar -Murillo, S. L., & Cendales -Duarte, R. (2006). Cervical cytology in Soacha, Colombia: social representation, barriers and motivation. Revista de Salud Pública (Bogotá), 8(3), 185-196.
20. Fernandez Esquer, M. E., & Cardenas Turanza, M. (2004). Cervical cancer screening among Latinas recently immigrated to the United States. Preventive Medicine, 38, 529-535.
21. Smith, M., French, L., & Barry, H. (2003). Periodic abstinence from Pap (PAP) smear study: women's perceptions of Pap smear screening. Annals of Family Medicine, 1(4), 203-208.
22. Barbosa, R., de Vasconcelos, G., Rosendo da Silva, R., Rosenado da Silva, D. (2005). Conhecimiento de mulheres de una unidades basica de saude da cidade de Natal/RN sobre o exame de Papanicolaou. Revista Escola Enfermagem, USP, 39(3), 296-302.
23. Fernandes, S., Hardy, E., Zeferino, L., & Namura, I. (2001). Knowledge, attitudes, and practices related to the Pap smear among women with cervical cancer. Cadernos de Saúde Pública, 17(4), 909-914.
24. Greenwood S de, A., Machado M de, F., & Sampaio, N. M. (2006). Motivos que llevam mulheres a ñao retornarem para receber o resultado de exame Papanicolau. Revista Latino-Americana de Enfermagem, 14(4), 503-509.
25. OPS. (2004). Análisis de la situación del cáncer cervicouterino en América Latina y el Caribe. Retrieved January 25, 2007, from http://www.paho.org/Spanish/AD/DPC/NC/pcc-ccsit-lac.pdf
26. Hou, S. I., & Luh, W. M. (2005). Psychometric properties of the cervical smear belief inventory for Chinese women. International Journal of Behavioral Medicine, 12(3), 180-191.
27. Byrd, T. L., Peterson, S. K., Chavez, R., & Heckert, A. (2004). Cervical cancer screening beliefs among young Hispanic women. Preventive Medicine, 38(2), 192-197.
28. SERNAM. (2008). Avanza participacion femenina. Retrieved May 29, 2008, from http://www.sernam.cl/opencms/opencms/sernam/regiones/2/noticias/news_0036.html
29. Blake, D. R., Weber, B. M., & Fletcher, K. E. (2004). Adolescent and young adult women's misunderstanding of the term Pap smear. Archives of Pediatric & Adolescent Medicine, 158(10), 966-970.
30. McMullin, J., De-Alba, I., Chavez, L., & Hubell, A. (2005). Influence of beliefs about cervical cancer etiology on Pap smear use among Latina immigrants. Ethnicity and Disease, 10(1), 3-18.
31. Rico, Ana María, & Iriart, Jorge Alberto Bernstein. (2013). "Where there's a woman, there's a Pap smear": the meanings assigned to cervical cancer prevention among women in Salvador, Bahia State, Brazil. Cadernos de Saúde Pública, 29(9), 1763-1773. Retrieved September 20, 2014, from http://www.scielosp.org/scielo.php?script=sci_arttext&pid=S0102311X2013001300016&lng=en&tlng=en.10.1590/0102-311X00146512.
32. Oshima, S., Masaji., M. (2013). Perception of cervical cancer screening among Japanese university students who have never had a Pap smear: a qualitative study. Asian Pacific Journal of Cancer Prevention, 14(7), 4313-4318.
33. Laranjeira., C.A. (2013). Portuguese women's knowledge and health beliefs about cervical cancer and its screening. Social Work in Public Health, 28(2), 150-7
34. Lartey, M., Joubert, G., & Cronje, H. S. (2003). Knowledge, attitudes and practices of rural women in South Africa regarding the Pap smear. International Journal of Gynecology and Obstetrics, 83(3), 315-316.
35. CDC. (2005 ). Breast and cervical cancer early detection. Retrieved December 3, 2006, from http://www.cdc.gov/programs/cancer01.htm