Breastfeeding Self-efficacy of Mothers and the Affecting Factors
La autoeficacia de las madres en cuanto a la lactancia y los factores que la afectan
A autoeficacia das mães quanto à lactancia e os fatores que a afetam
Recibido: 21 de julio de 2013
Enviado a pares: 05 de noviembre de 2013
Aceptación por pares: 11 de julio de 2014
Aprobado: 15 de julio de 2014
DOI: htpp://dx.doi.org/10.5294/aqui.2014.14.3.5
Cinar Nursan1
Köse Dilek2
Altinkaynak Sevin3
1 Sakarya University, School of Health Sciences, Division of Nursing, Department of Pediatric Nursing, Sakarya, Turkey.
ndede@sakarya.edu.tr
2 Sakarya University, School of Health Sciences, Turkey.
dkose@sakarya.edu.tr
3 Sakarya University, School of Health Sciences, Turkey.
saltinkaynak@sakarya.edu.tr
Para citar este artículo / To reference this article / Para citar este artigo
Nursan C., Dilek K. Sevin A. Breastfeeding Self-efficacy of Mothers and the Affecting Factors. Aquichan; 2014. 14(3): 327-335. DOI: 10.5294/aqui.2014.14.3.5
|
ABSTRACT Objectives: The purpose of this study was to determine the breastfeeding self-efficacy of mothers in the 0-3 month period and the affecting factors. Material and methods: The study was conducted between January-April 2011. The universe of the study consisted of all the mothers who were living in the center of Sakarya province and had infants ages 0-3 months. The sample used in the study consisted of 152 mothers who agreed to participate. The data were collected through face-to-face interviews with the mothers, using the "Personal Information Form" developed by the researchers and the "Breast-feeding Self-efficacy Scale-Short Form / BSES-SF" developed by Dennis. Turkish validity and reliability of the scale were done by Tokat et al. (2010). The data were evaluated with the SPSS program, using percentages, averages, the t-test, chi-square and ANOVA. Results: The average total score from the "taken BSES-SF" was determined as 58.61 ± 8.93, min = 16, max = 70. No significant differences were found between the scale score and maternal age (F = 0.437, p = 0.781), maternal education (F = 0.625, p = 0.645), economic status (F = 0.253, p = 0.777) and mode of delivery (t = 0.922, p = 0.358). The mean scores were determined as being higher for mothers who indicated having received training for breastfeeding compared to others who indicated having received no such training, and the difference between the scale score was statistically significant (X2 = 50.848, p = 0.010). Conclusions: Requirements for developing breastfeeding adequacy among mothers were determined. Nurses can give the necessary support to low breast-feeding mothers by assessing and identifying those requirements with help of this scale. KEYWORDS Breastfeeding, self-efficacy, affecting factors, nursing, 0-3 month old infant. (Source: DeCS, Bireme). |
RESUMEN Objetivos: el objetivo de este estudio fue determinar la autoeficacia de las madres en cuanto a la lactancia durante el período de 0-3 meses y los factores que la afectan. Materiales y métodos: el estudio se realizó entre enero y abril de 2011. El universo del estudio estuvo compuesto por todas las madres que vivían en el centro de la provincia de Sakarya y tenían niños lactantes de 0-3 meses. La muestra utilizada en el estudio estuvo conformada por 152 madres que aceptaron participar. Los datos fueron recolectados a través de entrevistas cara a cara con las madres, utilizando el "Formulario de Información Personal" desarrollado por los investigadores y el "Formulario de Escala de Autoeficacia en Lactancia - versión abreviada/ BSES-SF" desarrollado por Dennis. La validez y confiabilidad de la escala usada en Turquía fueron medidas por Tokat et al. (2010). Los datos fueron evaluados a través del programa SPSS, utilizando los porcentajes, los promedios, la prueba t, el chi-cuadrado y ANOVA. Resultados: el puntaje total promedio de la "BSES-SF tomada" se determinó como 58,61 ± 8,93, min. = 16, máx. = 70. No se hallaron diferencias significativas entre el puntaje de la escala y la edad materna (F = 0,437, p = 0,781), la educación materna (F = 0,625, p = 0,645), la situación económica (F = 0,253, p = 0,777) y el tipo de parto (t = 0,922, p = 0,358). Los puntajes promedio fueron mayores para las madres que indicaron haber recibido capacitación para la lactancia materna en comparación con otras que indicaron no haber recibido dicha formación, y la diferencia entre el puntaje de la escala fue estadísticamente significativa (X2 = 50,848, p = 0,010). Conclusiones: los requisitos para el desarrollo de un nivel adecuado de lactancia materna entre las madres fueron identificados. Las enfermeras pueden dar el apoyo necesario a las madres con bajo nivel de lactancia mediante la evaluación y la identificación de los requisitos con la ayuda de esta escala. PALABRAS CLAVE Lactancia materna, auto-eficacia, factores que la afectan, enfermería, niños de 0-3 meses de edad. (Fuente: DeCS, BIREME). |
RESUMO Objetivos: o objetivo deste estudo foi determinar a autoeficácia das mães quanto à lactancia durante o período de 0-3 meses e os fatores que a afetam. Materiais e métodos: o estudo foi realizado entre janeiro e abril de 2011. O universo do estudo esteve composto por todas as mães que moravam no centro da província de Sakarya e tinham crianças lactantes de 0-3 meses. A amostra utilizada no estudo esteve conformada por 152 mães que aceitaram participar. Os dados foram coletados por meio de entrevistas cara a cara com as mães, utilizando o "Formulário de Informação Pessoal" desenvolvido pelos pesquisadores e pelo "Formulário de Escala de Autoeficácia em Lactancia - versão abreviada BSES-SF" desenvolvido por Dennis. A validade e confiabilidade da escala usada na Turquia foram medidas por Tokat et al. (2010). Os dados foram avaliados por meio do programa SPSS, utilizando as porcentagens, as médias, a prova t, o qui-quadrado e Anova. Resultados: a pontuação total média da "BSES-SF tomada" foi determinada como 58,61 ± 8,93, min. = 16, máx. = 70. Não se constataram diferenças significativas entre a pontuação da escala e a da idade materna (F = 0,437, p = 0,781), da educação materna (F = 0,625, p = 0,645), da situação econômica (F = 0,253, p = 0,777) e do tipo de parto (t = 0,922, p = 0,358). As pontuações médias foram maiores para as mães que indicaram ter recebido capacitação para a lactancia materna em comparação com outras que indicaram não ter recebido essa formação, e a diferença entre a pontuação da escala foi estatisticamente significativa (X2 = 50,848, p = 0,010). Conclusões: os requisitos para o desenvolvimento de um nível adequado de lactancia materna entre as mães foram identificados. As enfermeiras podem dar o apoio necessário às mães com baixo nível de lactancia mediante a avaliação e a identificação dos requisitos com a ajuda dessa escala. PALAVRAS-CHAVE Lactancia materna, autoeficácia, fatores que a afetam, enfermagem, crianças de 0-3 meses de idade. (Fonte: DeCS, BIREME). |
Introduction
Breastfeeding is an important health-promoting behavior, conferring numerous health benefits to both mothers and infants (1). Mother's milk is the most appropriate food for infants. There is no other food to replace it (2). Breastfeeding is the normal way of providing young infants with the nutrients they need for healthy growth and development (3).
Today, many international and national organizations strongly advocate breastfeeding (4). According to the United Nations Children's Fund (UNICEF), breast milk is the baby's "first immunization" and helps to protect against causes of diarrhea, ear and chest infections, and other health problems (5).
Exclusive breastfeeding is recommended up to six (6) months of age, with continued breastfeeding, along with appropriate complementary foods, up to two years of age or beyond (3).
Many programmes have been developed throughout the world to promote breastfeeding initiation and duration (6). Launched by WHO and UNICEF in 1991, the Baby-friendly Hospital Initiative (BFHI) was inspired by the Innocenti Declaration of 1990. The initiative is a global effort to implement practices that protect, promote and support breastfeeding, so as to ensure that all maternity wards become centres for breastfeeding support. To be designated as 'baby-friendly,' it is necessary to refuse free or low-cost breast milk substitutes, feeding bottles or teats, and to have implemented the "10 steps to support successful breastfeeding" (7).
In Turkey, data from a national demographic health survey (2008) showed that 41.6% of infants are breastfed exclusively for the first six (6) months postpartum. Unfortunately, breastfeeding rates decline rapidly in the first eight (8) to 12 weeks pos tpartum, with fewer than 68.9% of Turkey's mothers breastfeeding exclusively at <2 months and 42% of Turkey's mothers breastfeeding exclusively at 2-3 months (8).
Breastfeeding self-efficacy, in particular, is a potentially modifiable variable that has been shown to predict longer breastfeeding duration and increased exclusivity. Breastfeeding self-efficacy is a concept based on Bandura's (1997) social cognitive theory (9). It is defined as a mother's confidence in her ability to breastfeed her child. 10 Efficacy beliefs are important to address in health promotion research, as people must have motivation and perseverance to maintain a health behavior, beyond simply the knowledge of the health benefits (1, 11).
Maternal breastfeeding self-efficacy is a mother's perceived ability to breastfeed her infant and has been shown to predict breastfeeding duration and exclusivity rates among women in the immediate postpartum period. The Breastfeeding Self-efficacy Scale-Short Form (BSESSF) was developed to measure a mother's confidence in her ability to breastfeed her new infant and has been successfully translated and psychometrically tested among women from diverse cultures (1, 3, 6, 12-14). In the Turkish study, Cronbach's alpha coefficient for internal consistency was 0.86 postnatally (6).
The purpose of this study was to determine the breastfeeding self-efficacy of mothers in the 0-3 month period and the affecting factors.
Methods
Ethical Considerations
This descriptive study was approved by the Ethical Board at Sakarya University and the study began after approval was received from related local authorities. The data were collected subsequent to approval of the study by the Ethics Committee. The participating mothers were informed of the purpose of the study and the methods to be used, and signed an informed consent statement. Participation was voluntary and could be terminated at any point in time.
The mothers were asked to answer all the questions honestly, and were reassured about the anonymity and confidentiality of the information.
Design and Sample
The study was conducted between January-April 2011. The universe of the study consisted of all the mothers who were living in the center of Sakarya province and had infants ages 0-3 months. The study sample consisted of 152 mothers who agreed to participate.
Participants
Participation criteria: mothers who were over 18 years old and had healthy infants between ages 0-3 months, had no communication problems and agreed to participate voluntarily in the study. Mothers with premature babies or multiple babies were excluded from the study. The data were obtained from mothers who came to two family health centers and outpatient clinics of a state hospital.
Data Collection Procedures and Instruments
The data were collected through face-to-face interviews with mothers, using the "Personal Information Form" developed by the researchers and the "Breast-feeding Self-efficacy Scale-Short Form / BSES-SF" developed by Dennis. The Personal Information Form included personal characteristics (gender, age, education, economical status), delivery - postpartum characteristics (type of delivery, obstetric interventions/complications) and infant feeding characteristics (breast only, breast with occasional supplement, breast with supplement at every feeding, breastfeeding duration).
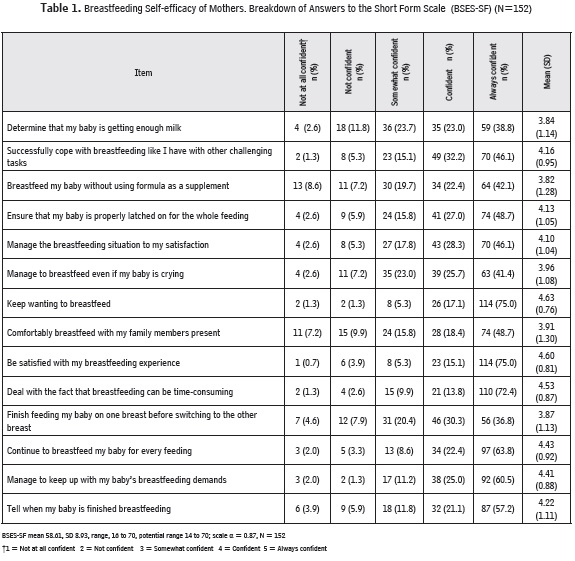
The BSES-SF is a 14-item instrument developed to measure breastfeeding confidence. All the items are preceded by the statement ''I can always'' and are anchored by a 5-point Likert-type scale, with 1=not at all confident and 5=always confident. All the items are presented positively and the scores are summed up to produce a final score ranging from 14 to 70, with the higher scores indicating better breastfeeding self-efficacy. Turkish validity and reliability of the scale were done by Tokay, Okumu§ and Dennis (2010). In the same study, Cronbach's alpha coefficient for internal consistency was 0.87 antenatally and 0.86 postnatally. The antenatal and postnatal BSES-SF scores were significant predictors of breastfeeding duration and exclusivity at 12 weeks after birth (6). In our sample study, Cronbach's alpha coefficient was 0.87.
Data Analysis
The data were evaluated with the SPSS program (version 17), using percentages, averages, the t-test, chi-square and ANOVA.
Results
As for the mothers, 49.4% (n=75) were found to be between the ages of 18-26, 46.1% (n = 70) were primary school graduates and 89.5% (n = 136) were unemployed. In addition, 62.5% (n = 95) of the families described their economic situation as moderate, 36.2% (n=55) of the women were primiparous, 38.8% (n=38.8) of the multiparous mothers had just given birth to their second child, 17.8% (27) had just given birth to their third child, 7.2% (11) had just given birth to their fourth child or more than four. All of the multiparous mothers had breastfeeding experience. The majority of the deliveries (n=86, 56.6%) were by cesarean section and 43.4% (n = 66) of the mothers had delivered vaginally. In this study, 81.6% (124) of the mothers indicated having received training for breastfeeding and 18.4% (n=28) indicated they had received no such training.
Cronbach's alpha coefficient (internal reliability) for the general scale was 0.87. The average total score taken from the "BSESSF" was (X= 58.61 ± 8.93, min = 16, max = 70), respectively.
There was no significant difference between the scale score and maternal age (F = 0.437, p = 0.781), nor were significant differences found between scale score and maternal education (F = 0.625, p = 0.645) and economic status (F = 0.253, p = 0.777) (Table 2).
When mode of delivery was compared to the scale score, no significant differences were found (t = .922, p= .358). Although there was no difference between the scale score and mode of delivery, caesarean the mothers who gave birth by section had higher scores for breastfeeding self-efficacy (M=59.20 SD=9.01) than those who had given birth vaginally (M=57.85 SD=8.84). There was a significant difference between the scale score and previous breastfeeding experience (t=2.055 p= .042). Breastfeeding self-efficacy was found to be low among the mothers who had no prior breastfeeding experience. The mean scores were higher for the mothers who breastfed their infants exclusively compared to those who breastfed partially, and the difference between the scale score was statistically significant (t=4.036 p= .000). (Table 3).
The mean scores were found to be higher for mothers who indicated having received training in breastfeeding compared to others who indicated having received no such training, and the difference between the scale score was statistically significant (X2=50.848 p= .010).
Discussion
The BSES-SF was developed to measure a mother's confidence in her ability to breastfeed her baby. The Cronbach's alpha coefficient for the sample used in the study was 0.87.
In the Turkish study, Cronbach's alpha coefficient for internal consistency was 0.86 postnatally (6). The same result taken from the study by Wutke and Dennis (2007) was 0.89 (13). Cronbach's alpha coefficient for the scale was 0.94 (Spaulding and Dennis 2010), 0.90 (Gregory et al. 2008) and 0.92 (Roig et al. 2012) (1, 12, 15). Nevertheless, the studies by Dodt et al. 2012 and Zubaran et al. 2010 showed 0.74 and 0.71 (7, 14), respectively.
Maternal demographic factors play a broad role in breastfeeding behaviour, with improvements seen with better schooling and previous breastfeeding experience (4, 7).
There was no significant difference between the BSES-SF score and maternal age in this study (F = 0.437, p = 0.781) (Table 2). Similarly, no relationship was found between the scale score and maternal age in the others studies (1, 4, 6, 12, 13, 15). However, the study by Dodt et al. (2012) indicated a strong correlation (7). Not only the study by Dodt et al. (2012), but also the one by Wutke and Dennis (2010) identified a weak correlation between the scale score and maternal age (2010) (7, 13).
In this study, no relationship was found between the BSES-SF score and maternal education (F = 0.625, p = 0.645). Although a relationship between the scale score and maternal education was indicated only in the study by Tokat, Okumuç and Dennis (2010), the results of other studies (4, 7, 12-14) coincide with our result.
When the BSES-SF score was compared to economic status, there was no significant difference (F = 0.253, p = 0.777). This was similar to other studies (1, 4, 7, 14) in terms of economic status. However, the previous study in Turkey indicated there is a relationship between the scale score and economic status (6).
There was no significant difference in this study between the BSES-SF score and mode of delivery (t = 0.922, p = 0.358) (Table 3). Although a relationship between the scale score and mode of delivery was indicated in the study by Tokat, Okumuç and Dennis (2010) (6) and in the one by Dennis in 2003 (4), the results of other studies (1, 12-14) coincide with our result.
In this study, the mothers who gave birth by caesarean section had higher breastfeeding self-efficacy scores (M = 59.20 SD=9.01) than the mothers who gave birth vaginally (M = 57.85 SD=8.84). However, in the studies by Dennis (2003) and Tokat, Okumuç and Dennis (2010), the women who gave birth vaginally showed higher BSES-SF scores than mothers who had a caesarean section (4, 6).
There was a significant difference between the scale score and previous breastfeeding experience (t=2.055 p=.042). The mean BSES-SF score for women with previous breastfeeding experience was significantly higher (M = 59.72 SD: =7.91) than the BSES-SF scores for women who had no prior breastfeeding experience (M=56.65 SD=10.28). A relationship between the scale score and previous breastfeeding experience was found in the studies by Tokat, Okumuç and Dennis (2010), Gregory et al. (2008) and Wutke and Dennis (2007) (6,12,13).
Conclusion
The Turkish version of the BSES is of diverse utility in clinical practice. Use of this scale gives nurses and midwives an excellent opportunity to increase a mother's breastfeeding self- efficacy.
In addition, any mother who has been identified as having low breastfeeding self-efficacy should have the opportunity to receive additional support.
In this study, breastfeeding self-efficacy was found to be low among mothers who had no prior breastfeeding experience. It is required that health practitioners provide more support to new mothers.
Limitations of the Study
The limitation of this study concerns the fact that its results are based on data from only the Sakarya district. Consequently, it cannot be generalized for Turkey. Similar studies on various populations in Turkey and in other countries should be conducted.
Acknowledgements
The authors wish to thank the mothers who participated in this study.
Conflict of Interest
The authors declare they have no competing interests.
Authors' Contributions
Study concept and design: Cinar N, Kose D, Altinkaynak S
Acquisition of subjects and data: Cinar N, Kóse D
Data analysis and interpretation: Cinar N
Preparation of the manuscript: Cinar N, Kóse D, Altinkaynak S
All the authors have read and approved the final version of
the manuscript.
References
1. McCarter- Spaulding DE, Dennis CL. Psychometric testing of the breastfeeding self- efficacy scale- short form in a sample of black women in the United States. Research in Nursing & Health 2010; 33: 111-9.
2. Çinar ND, Sözeri CU, Altinkaynak S. Basarili nesiller için anne sütü. Saglicakla Aylik Saglik Dergisi 2009; 12: 20-21.
3. Dennis CL. The breastfeeding self-efficacy scale: psychometric assessment of the short form. JOGNN 2003; 32 (6): 734-44.
4. World Health Organization (WHO). Breastfeeding. Available at: 28.06.2012 Available from: URL: http://www.who.int/topics/breastfeeding/en/
5. United Nations Children's Fund (UNICEF). Facts for life. New York: UNICEF; 2002.
6. Tokat MA, Okumus H, Dennis CL. Translation and psychometric assessment of the breastfeeding self- efficacy scale-short form among pregnant and postnatal women in Turkey. Midwifery 2010; 26: 101-8.
7. Dodt ECM, Ximenes LB, Almeida PC, Oria MOB, Dennis CL. Psychometric and maternal sociodemographic assessment of the breastfeeding self-efficacy scale- short form in a Brazilian sample. Journal of Nursing Education and Practice 2012; 2(3): 66-73.
8. Türkiye Nüfus ve Saglik Arastirmasi (TNSA). Ankara; 2008.
9. Bandura A. Self-efficacy: Toward a unifying theory of behavioral change. Psychological Review 1977; 84(2): 191-215.
10. Dennis C, Faux S. Development and psychometric testing of the Breastfeeding Self- Efficacy Scale. Research in Nursing & Health 1999; 22(5): 399-409.
11. Bandura A. Health promotion from the perspective of social cognitive theory. In: P. Norman, C. Abraham, & C. Conner (Eds.), Understanding and changing health behavior. Amsterdam: Overseas Publishers Association, 2000: (pp. 299-339).
12. Gregory A, Penrose K, Morrison C, Dennis CL, MacArthur C. Psychometric properties of the Breastfeeding Self-efficacy Scale-Short Form in an ethnically diverse U.K. sample. Public Health Nursing 2008; 25(3): 278-84.
13. Wutke K, Dennis C. The reliability and validity of the Polish version of the Breastfeeding Self-efficacy Scale-Short Form: Translation and psychometric assessment. International Journal of Nursing Studies 2007; 44(8): 1439- 46.
14. Zubaran C, Foresti K, Schumacher M, Thorell MR, Amoretti A, Muller L, et al. The Portuguese version of the Breastfeeding Self-efficacy Scale - Short Form. J Hum Lact 2010; 26: 297-303.
15. Roig AO, d'Anglade-González ML, Garcia-Garcia B, Silva-Tubio JR, Martinez MR, Dennis CL. The Spanish version of the Breastfeeding Self-efficacy Scale-Short Form: Reliability and validity assessment. International Journal of Nursing Studies 2012; 49: 169-73.