Management of Continuous Positive Airway Pressure in the Newborn:
Impact of Lecture-based Interactive Workshops on Training for Neonatal Intensive Care Nurses
Manejo de la presión positiva continua en las vías respiratorias en el recién nacido:
el impacto de talleres interactivos basados en conferencias sobre la formación de las enfermeras de cuidados intensivos neonatales
Manejo da pressão positiva contínua nas vias respiratórias no recém-nacido:
o impacto de oficinas interativas baseadas em conferências sobre a formação das enfermeiras de cuidados intensivos neonatais
Recibido: 05 de noviembre de 2015
Enviado a pares: 21 de noviembre de 2015
Aceptado por pares: 27 de enero de 2016
Aprobado: 29 de enero de 2016
Öznur Tiryaki1
Nursan Cinar2
1 Sakarya Maternity and Children's Hospital, Neonatal Intensive Care Unit, Sakarya/TURKEY.
oznuritiryaki@gmail.com
2 Sakarya University School of Health Sciences, Department of Peadiatric Nursing, Sakarya/TURKEY.
ndede@sakarya.edu.tr
Para citar este artículo / To reference this article / Para citar este artigo
Tiryaki O, Cinar N. Management of Continuous Positive Airway Pressure in the Newborn: Impact of Lecture-based Interactive Workshops on Training for Neonatal Intensive Care Nurses. Aquichan. 2016; 16(2): 159-168. DOI: 10.5294/aqui.2016.16.2.4
|
ABSTRACT Objectives: The aim of this study was to determine how training imparted via structured workshops related to management of continuous positive airway pressure in the newborn affects the knowledge of neonatal intensive care nurses. Methods: A group of nurses attended an interactive lecture-based workshop on management of continuous positive airway pressure in the newborn. The nurses in question had accepted an invitation to the presentation prior to the training event. Information on the participants' differentiating features was collected via a questionnaire prepared by the researchers themselves. An evaluation of the nurses' knowledge on the subject was performed through a multiple choice questionnaire (MCQ) prepared by the researchers in relation to the literature. After the MCQ was prepared, it was mailed to experts in Turkey (7 people) and experts from abroad (5 people), and their opinions were considered. In light of their suggestions, the MCQ was given its final form and the number of questions was set at 20. The MCQ consisting of 20 questions was answered by the participants before and after the interactive workshop. The participants were not informed as to whether or not the test would be repeated after the training. Results: Thirty-six nurses from the neonatal unit took part in the study. Each question in the MCQ was considered as one (1) point. The maximum possible score on the test was 20. There was a significant improvement in the mean test score after the lecture, when compared to the pre-lecture score (Mean = 19.6, SD=0.8 vs. Mean =13.1, SD=3.0, P<0.001). Conclusions: A lecture-based inter active workshop on management of continuous positive airway pressure in newborns helps to improve nurses' knowledge. It also helps to overcome deficiencies in nurse training. KEYWORDS Continuous positive airway pressure, newborn health services, nurse, training, knowledge (Source: DeCS, BIREME). |
RESUMEN Objetivos: el objetivo de este estudio fue determinar cómo la formación impartida a través de talleres estructurados relacionados con el manejo de la presión positiva continua en las vías respiratorias en el recién nacido afecta el conocimiento de las enfermeras que trabajan en cuidados intensivos neonatales. Métodos: un grupo de enfermeras asistieron a un taller interactivo basado en una conferencia sobre el manejo de la presión positiva continua en las vías respiratorias en el recién nacido. Las enfermeras en cuestión habían aceptado una invitación para asistir a la presentación antes del evento de capacitación. La información sobre las características diferenciadoras de los participantes se recogió a través de un cuestionario elaborado por los propios investigadores. Una evaluación de los conocimientos de las enfermeras sobre el tema se llevó a cabo a través de un cuestionario de selección múltiple (CSM), el cual fue elaborado por los investigadores en relación con la literatura. El CSM fue enviado por correo a unos expertos en Turquía (siete personas) y unos expertos en el exterior (cinco personas), y sus opiniones fueron tomadas en cuenta. A la luz de sus sugerencias, al CSM se le dio su forma final y el número de preguntas se fijó en 20. El CSM, que consta de 20 preguntas, fue respondido por los participantes antes y después del taller interactivo. A los participantes no se les dijo si la prueba se repitió después del taller de formación. Resultados: treinta y seis enfermeras de la unidad neonatal participaron en el estudio. Cada pregunta en el CSM se consideró como un (1) punto. La puntuación máxima posible en la prueba fue 20. Hubo una mejora significativa en la puntuación de la prueba media después de la conferencia, si se compara con la puntuación preconferencia (media = 19,6, SD = 0,8 vs. media = 13,1, SD = 3.0, P <0,001). Conclusiones: un taller interactivo basado en una conferencia sobre el manejo de la presión positiva continua en las vías respiratorias en el recién nacido ayuda a mejorar el conocimiento de las enfermeras. También ayuda a superar las deficiencias en la formación de enfermeras. PALABRAS CLAVE Presión positiva continua en las vías respiratorias, servicios de salud para el recién nacido, enfermera, formación, conocimiento (Fuente: DeCS, BIREME) |
RESUMO Objetivos: o objetivo deste estudo é determinar como a formação ministrada nas oficinas estrturadas relacionadas com o manejo da pressão positiva contínua nas vias respiratórias no recém-nascido afeta o conhecimento das enfermeiras que trabalham em cuidados intesivos neonatais. Métodos: um grupo de enfermeiras participaram de uma oficina interativa baseada numa conferência sobre o manejo da pressão contínua nas vias respiratórias no recém-nascido. as enferemeiras em questão tinham aceitado um convite para comparecer à apresentação antes do evento de aperfeiçoamento. a informação sobre as características diferenciadoras dos participantes foi coletada por meio de um questionário elaborado pelos próprios pesquisadores. Uma avaliação dos conhecimentos das enfermeiras sobre o tema foi realizado mediante questionário de múltipla escolha (QME), o qual foi elaborado pelos pesquisadores de acordo com a literatura. o QME foi enviado por e-mail a sete especialistas na Turquia e a outros cinco no exterior, e suas opiniões foram consideradas. À luz das sugestões, o QME, que consta de 20 perguntas, foi respondido pelos participantes antes e depois da oficina interativa. Resultados: 36 enfermeiras da unidade neonatal participaram do estudo. Cada pergunta do QME foi considerada como (1) ponto. A pontuação máxima possível na prova foi 20. Houve uma melhora significativa na pontuação da prova média depois da conferência, se comparada com a pontuação pré-conferência (media = 19,6, SD = 0,8 vs. media = 13,1, SD = 3.0, P < 0,001). Conclusões: uma oficina interativa baseada numa conferência sobre o manejo da pressão positiva contínua nas vias respiratórias no recém-nascido ajuda a melhorar o conhecimento das enfermeiras e a superar as deficiências na sua formação. PALAVRAS-CHAVE Pressão positiva contínua nas vias respiratórias, serviços de saúde para o recém-nascido, enfermeira, formação, conhecimento (Fonte: DeCS, BIREME). |
Introduction
The most common admission to neonatal intensive care units (NICU) is due to respiratory problems. The causes of respiratory distress are respiratory distress syndrome (RDS), transient tachypnea of the newborn (TTN), meconium aspiration syndrome (MAS) and pulmonary infection (1). The most commonly used treatment for supporting the respiration of a newborn and the first-preferred treatment option at the third level NICU is continuous positive airway pressure (CPAP) administration (2).
CPAP was first defined in the literature by Gregory et al. in 1971 (3) and was used to support respiration in infants diagnosed with RDS (4). In general, several centimeters of water (cmH2O) are applied through the nose to the airways for CPAP (5). This application also is used for preventing atelectasis and conserving the functional residual capacity (FRC) remaining in the alveolar due to positive pressure in the newborn with spontaneous respiration (6).
CPAP through the nose can be applied with single or double prongs, in either short (into the nose) or long (nasopharynx) form and with masks (6,7). CPAP is generated by exhalation against a constant opening pressure; this produces positive endexpiratory pressure (PEEP) (8). The treatment usually starts with 5 cmH2O pressure and can go up to 10 cmH2O pressure, depending on the clinical condition of the infant (7). Among the CPAP methods, the most popular and the most frequently used are bubble CPAP (in B-CPAP, the positive pressure in the circuit is achieved by simply immersing the distal expiratory tubing in a water column to a desired depth rather than using a variable resistor) and ventilatory CPAP (in V-CPAP, a variable resistance in a valve is adjusted to provide resistance to the flow of air) (9).
CPAP develops a synchronisation between thorax and abdominal movement and improves the function of the diaphragm (3), increases the formation of surfactant and FRC, and reduces the need for intubation and surfactant treatment (10). It is also a popular alternative to intubation (11).
CPAP decreases the need for ventilation in infants born between 25 and -28 weeks of pregnancy, and the need to be transferred to hospitals with third level intensive care units for infants born before the 32nd week of pregnancy (3). Early CPAP use also decreases the incidence of bronchopulmonary dysplasia (BPD) and the administration of oxygen at home following discharge (12).
A health staff (a doctor, a nurse) is needed for CPAP administration. The nurse should be informed about the side effects of CPAP (pneumothorax, distension, nasal injuries, etc.), and should be able to diagnose the presenting problem (4). Being an inexpensive and safe application, CPAP can be administered by nurses following short-term training; thus, its effectiveness or failure is related to adequacy of the nurse's care and knowledge (4, 13, and 14). This study was performed starting with the hypothesis that this type of interactive training carried out via a PowerPoint presentation, prepared according to the literature and in light of expert views, would be effective and meet the needs on the issue. We became interested in this subject given the lack of sources in Turkish resources on CPAP and its administration, and the fact that neonatal nurses require education on the subject. This study aims to determine how the training imparted to NICU nurses via an interactive workshop on the care of newborns requiring CPAP affects their level of knowledge. Our hypothesis in this study is that the MCQ score for participating nurses increases after the interactive workshop.
Materials and methods
This pre / post- test experimental study was conducted in a city in the Marmara region during April 2014. Approval for the study was obtained from the University Ethical Committee in that city. Required approval for the nurses who would participate in the study was obtained from a university, a state hospital and two private hospitals. Some of the participating nurses had to be on duty while the study was conducted, so it was possible to reach a total of 73.4% (36/49) of the intended population. The sample group was comprised of 36 nurses who volunteered to take part in the study. Information on the participants' identifying features was collected via a questionnaire prepared by the researchers themselves. The evaluation of the data obtained from the participants was done by the researchers using a multiple choice questionnaire (MCQ) prepared in light of the literature. After the MCQ was prepared, it was presented to 14 experts for their opinion; 12 of those experts responded (85.7%). It was sent to seven (7) people in Turkey and five (5) people abroad who were considered to be experts on the subject, and their opinions were obtained. The experts found the MCQ to be appropriate for specific research content. Three expression changes were proposed and all 20 questions were found to be appropriate. Based on their suggestions, the MCQ was given its final form and the number of questions was set at 20 (Attachment A). Every true answer received 1 point, and every false answer was scored as 0. The lowest possible score on the MCQ is 0 and the highest is 20.
The participating nurses attended an interactive lecture-based workshop on CPAP management in newborns. They had accepted an invitation to the presentation prior to the training event. The study was conducted in the conference hall of a university hospital with the participation of 36 nurses who were working in neonatal departments. Their participation in the study was voluntary. A pre-lecture MCQ test was completed by the nurses to test their existing knowledge. The questions in the MCQ were derived from the topic covered in the presentation. Following the lecture, the MCQ test was repeated to assess retention and application of the knowledge derived from the interactive lecture. The participants did not know they would be tested with an MCQ, which would be repeated at end of the workshop. The lecture consisted of a PowerPoint presentation. It was followed by an interactive session of discussions, questions and answers, which continued until it was noted the participants had increased their knowledge.
Statistical Analysis
The data were analyzed with SPSS 16. The Kolmogrov Simirnow test was used to determine if the data show a normal distribution. The Wilcoxon signed rank test was used, since the data did not show a normal distribution. Pre-test and post-test results were found to be statistically significant, according to the Wilcoxon s rank test (Z= -5.239, p=.000).
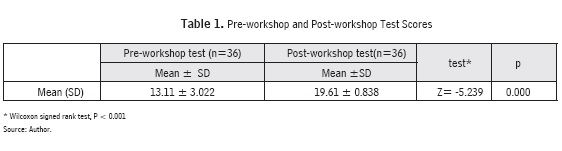
The Wilcoxon signed test was used because we compared the total score before and after the lecture, rather than each answer in the questionnaire, and the data did not have a normal distribution. The test is two dimensional, which meets the hypothesis that there is a difference (Table 1).
Findings
Thirty-six female nurses participated in the study. In all, 36.1% (13/36) of the nurses had a graduate degree, 50% (18/36) had been working at the NICU for 1-5 years, 44.4% (16/36) had NICU nursing certificates, and 33.3% (12/36) had neonatal resuscitation program certificates. Thirty-six nurses attended the workshop. There was a statistically significant improvement in their test scores after the lecture, when compared to the prelecture scores (Pre-test min. 6 points/max.19 points mean: 13.11 SD:3.022, Post-test min.17 points/max.20 points mean:19.61 SD: 0.838, Z= 5.239, p=.000) (Table 2).
Discussion
This study was conducted to determine the levels of knowledge nurses have with respect to CPAP and to evaluate the effects of the training imparted on this subject. In general, the nurses were keen on the study since they found it interesting.
The participants in this study were at nurse training grades, had been qualified four years previously, and were actively working at NICUs. Consequently, they would be expected to have a reasonable understanding of CPAP management in newborns.
The pre-test score on the 20 questions prepared through the suggestions of experts in light of the literature was low (Mean: 13.1 SD: 3.022 ), indicating the nurses did not have enough knowledge on the subject. The participants were shown an interactive PowerPoint presentation containing the answers of those questions, and a post-test was applied with the same questions. The post-lecture test score showed a significant increase (Mean: 19.61 SD: 0.838). It is observed that these kinds of studies aimed at the nurse's skills and knowledge aid improvement through appropriate practice (15,16,17).
Suggestions
It is inevitable to have regular updates for nurses who perform a significant role in newborn care and to provide the necessary evidence-based nursing applications in CPAP practice, which is being used increasing on a regional and international basis. The effectiveness of the teaching method, which can be used to meet this need, was examined in this research. The questions here can be used in both regional and international studies and in nurse training, if updated according to the literature.
Limitations of the Study
One of the limitations of this study was that all the nurses working in the study area related to the subject could not be reached. There are 49 nurses working at neonatal departments. A total of 74.3% (36/49) were able to participate in the study. Some of the nurses could not take part, because they were on duty at the time the study was conducted. To compensate for this drawback, a new workshop program was planned for the nurses who could not participate initially.
These kinds of educational studies conducted with small groups are an effective way to make up for a lack of information and to correct false beliefs. The methods applied and the information obtained could help future researchers set a base and establish more sample groups. It is possible to improve the quality and safety of newborn care by having nurses acquire sufficient knowledge and skills. The method used in this study proved to be efficient, since it helped to increase the knowledge of the nurses who took part. The nurses in our study were assessed only as to the extent of their knowledge. It is suggested that other studies be conducted to evaluate their skills on the subject in question.
Acknowledgements
We wish to thank our esteemed specialists and nurses who participated and supported us by evaluating the multiple choice questions used in the study.
References
1. Yagui ACZ, Vale LAPA, Hadda LB et al. Bubble CPAP versus CPAP with variable flow in newborns with respiratory distress: A randomized controlled trial. Journal de Pediatria 2011;87:499-503.
2. Roberts CL, Badgery-Parker T, Algert CS et al. Trends in use of neonatal CPAP: A population-based study. BMC Pediatrics 2011;11:89.
3. Sankaran K, Adegbite M. Noninvasive respiratory support in neonates: A brief review. Chin J Contemp Pediatr 2012; 14:643-652.
4. Bonner KM, Mainous RO. The nursing care of the infant receiving bubble CPAP therapy. Advances in Neonatal Care 2008;8:78-95.
5. Morley C. Which neonatal nasal CPAP device should we use in babies with transient tachypnea of the newborn? Journal de Pediatria 2011; 87:466-467.
6. Petty J. Factsheet: Understanding neonatal noninvasive ventilation. Journal of Neonatal Nursing 2013;19:10-14.
7. De Paoli AG, Morley C, Davis PG. Nasal CPAP for neonates: What do we know in 2003? Arch Dis Child Fetal Neonatal Ed 2003;88:168-172.
8. Duke T. CPAP: A guide for clinicians in developing countries. Paediatr Int Child Health 2014;34(1):3-11.
9. Bijari BB, Malekiyan A, Niknafs P et al. Bubble-CPAP vs. ventilatory-CPAP in preterm infants with respiratory distress. Iran J Pediatri 2011; 21: 151-158.
10. DiBlasi RM. Neonatal noninvasive ventilation techniques: Do we really need to intubate? Respir Care 2011;56:1273-1294.
11. De Winter JP, De Vries MAG, Zimmermann LJI. Clinical practice noninvasive respiratory support in [the] newborn. European Journal of Pediatrics 2010;169:777-782.
12. Tood AD, Wright A, Broom M et al. Methods of weaning preterm babies <30 weeks gestation off CPAP: A multicentre randomised controlled trial. Arch Dis Child Fetal Neonatal Ed 2012;97:236-240.
13. Koyamaibole L, Kado J, Qovu JD et al. An evaluation of bubble-CPAP in a neonatal unit in a developing country: Effective respiratory support that can be applied by nurses. Journal of Tropical Pediatrics 2006;52:249-253.
14. Heuvel MVD, Blencowe H, Mittermayer K et al. Introduction of bubble CPAP in a teaching hospital in Malawi. Annals of Tropical Paediatrics 2011;31:59-65.
15. Altun I, Çinar ND, Barin ŐC. Best practice techniques for administration of injections: Impact of lecture based interactive workshops on training of nurses. Pakistan Journal of Medical Sciences 2010;26:152-157.
16. Altun I, Zencirci AD. Management of fever and hyperthermia: Impact of lecture based interactive workshops on training of nurses. Libyan Journal of Medicine 2010;5:5140.
17. Altun I, Zencirci AD. Knowledge and management of pressure ulcers: Impact of lecture-based interactive workshops on training of nurses. Advances in skin & wound care, Journal for Prevention and Healing 2011;24:262-266.